Introduction to oral mucosa

The oral mucosa has several functions. Its main purpose is to act as a barrier. It protects the deeper tissues such as fat, muscle, nerve and blood supplies from mechanical insults, such as trauma during chewing, and also prevents the entry of bacteria and some toxic substances into the body.
The oral mucosa has an extensive innervation of nerves, which allows the mouth to be very receptive of hot and cold, as well as touch. Taste buds are also located in oral mucosa and are important for recognition of taste.
The major secretion associated with the oral mucosa is saliva, produced by the salivary glands. The major salivary glands secrete most of the saliva via ducts that pass through the oral mucosa.
There is a degree of permeability that allows for rapid absorption into the body in certain circumstances e.g. the permeability of the oral mucosa is utilised in the rubbing of orange juice, or another sugary drink when diabetics suffer from a low-blood sugar.
The oral mucosa
The oral mucosa consists of two layers: the corium (or lamina propria) and the epithelium. The epithelium is the surface layer, and where there is a disease of the oral mucosa, often it is the epithelium that is most affected.
Epithelial proliferation is the term given to the ability of any epithelium to be able to renew itself after cells die, that is, the ability to turnover cells. This occurs in the stratum basale, which is situated on deepest layer of cells in thin epithelia (e.g. the bottom of the mouth), and in the lower two to three cells layers of thicker epithelia (e.g. buccal mucosa or inside of the cheek).
There are two types of cells that contribute to renewing cells in any epithelium:
- A small population of cells appear to cycle slowly and tend to be the stem cells of the epithelia, whose function is to produce more cells that will be able to turnover cells; and
- The large population of cells appear to be composed of “amplifying cells”, whose function is to increase the number of cells that are able to “mature,” and eventually die as part of the normal cycle of cell turnover.
Each type of cell undergoes cell division, and consequently each resultant cell recycles in stem cell population, or matures.
In general, maturation can undergo two different patterns:
The most common cells that are required to undergo cell turnover are called keratinocytes. As the keratinocyte matures, it undergoes modification in its structure that causes it to progress towards the surface of the epithelium, and eventually die. Keratinocytes mature to different degrees. In some areas of the mouth, the keratinocytes will fully mature (orthokeratinisation), whereas in other areas the keratinocytes will only partially undergo keratinisation (parakeratinisation).
For each dividing cell, one cell is lost from the surface, thus, the integrity of that area is maintained. The rate in the oral cavity is much faster than on skin (approximately twice as fast), and areas such as the inside of the cheek will turnover in about 20 days.
The hard surface of some mucosa (such as the top of the mouth (hard palate), the gums (gingivae), and some areas on the bottom of the tongue (dorsum of the tongue) is inflexible, tough, resistant to abrasion, and tightly bound to the underlying tissue.
The mucosal surface shows evidence of a surface layer of keratin, which is the end product of keratinisation (in fully keratinised areas). Under a microscope, there are several distinct layers that can be grouped together.
In the fully keratinised situation:
- The cells start at the basal layer (deepest part of epithelium), which is comprised of square and rectangular shaped cells and is right next to the underlying lamina propria.
- These undergo division and migrate towards the surface, into the stratum spinosum, which contains a high number of small attachments that allow cells to communicate with each other. The cells in the prickle cell layer appear elliptical and are given this name as under a microscope they appear “prickly”.
- As the cells of the stratum spinosum migrate to the surface they begin to flatten and intensely staining granules give the characteristic appearance to the stratum granulosum in keratinised epithelia, also known as the granular layer. These granules are known as keratohyalin granules.
- Finally, at or near the surface of the epithelium, the inside of the cell begins to disintegrate and a lot of its structure is lost. It is now fully matured to be part of the stratum corneum. At this stage, the cells are lost into the mouth.
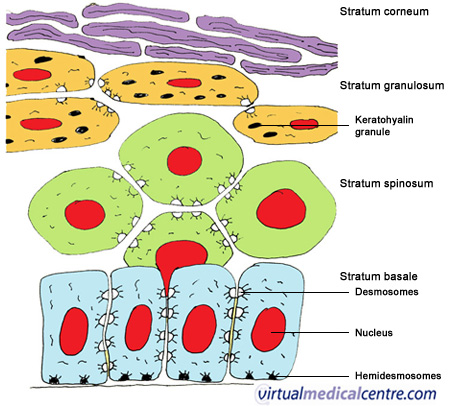 |
| Figure 1: The process of (ortho)keratinisation. Stratum basale is the area of epithelium where new cells are formed to replace ones that have been shed; stratum spinosum is the area where cells appear like “prickles” under a microscope; stratum granulosum is where the cells flatten out and keratohyalin granules appear; and stratum corneum is the most superficial layer where nuclei degenerate and keratohyalin granules disappear. |
The process of keratinisation does not take place in all areas of the mouth. It occurs on the lips, soft palate (back of the mouth), floor of the mouth, ventral surface of tongue (top of the tongue), and alveolar mucosa (near the gums) and essentially differs in the process of keratinisation because:
- Keratohyalin granules are not formed and thus the granular layer is not formed; and
- The inside of each cell can be seen microscopically in the outside layers of the epithelium.
The basal and prickle cell layers are similar in appearance to keratinised areas, although the cells can be a bit larger. The epithelium can be considerably thicker in areas of non-keratinised compared to keratinised mucosa.
In partially keratinised mucosa (parakeratotic epithelium), the inner contents of cells may be visible microscopically in some cells, but not in all of them. There is essentially a spectrum ranging from complete non-keratinisation at one extreme, through varying degrees of parakeratinisation, to full orthokeratinisation at the other.
Other cells that may be found in oral mucosa include:
| Cell Type | Level in Epithelium | Function |
|---|---|---|
| Melanocyte | Basal | Synthesis of melanin pigment, which is responsible for the colour of skin |
| Langerhans cell | Mostly basal | Part of the immune system; is presented with foreign things such as virus’, and bacteria, and is able to alert the immune system |
| Merkel cell | Basal | Ability to feel things |
| Lymphocyte | Variable | Associated with inflammatory response in mucosa |
In the corium and submucosa lie:
- Minor salivary glands and other secretory glands of the oral cavity;
- Blood vessels;
- Fat;
- Fibrous tissue; and
- Scattered cells of different white blood cells.
Kindly written by Dr Akhil Chandra BDSc. (Hons UWA)
Dentist, Whitfords Dental Centre and Editorial Advisory Board Member of the Virtual Dental Centre
References
-
Nanci A. Ten Cate’s Oral Histology: Development, Structure, and Function (6th edition). St Louis: Mosby, 2003.
- Field A, Longman L. Tyldesley’s Oral Medicine (5th edition). Oxford: Oxford University Press, 2003.
- Dowden J (ed). Therapeutic Guidelines: Oral and Dental (1st edition). North Melbourne: Therapeutic Guidelines Limited, 2007.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







