- What is Lung Cancer (Adenocarcinoma of the Lung)
- Statistics on Lung Cancer (Adenocarcinoma of the Lung)
- Risk Factors for Lung Cancer (Adenocarcinoma of the Lung)
- Progression of Lung Cancer (Adenocarcinoma of the Lung)
- Symptoms of Lung Cancer (Adenocarcinoma of the Lung)
- Clinical Examination of Lung Cancer (Adenocarcinoma of the Lung)
- How is Lung Cancer (Adenocarcinoma of the Lung) Diagnosed?
- Prognosis of Lung Cancer (Adenocarcinoma of the Lung)
- How is Lung Cancer (Adenocarcinoma of the Lung) Treated?
- Lung Cancer (Adenocarcinoma of the Lung) References
What is Lung Cancer (Adenocarcinoma of the Lung)
Lung cancers are tumours arising from cells lining the airways of the respiratory system. Adenocarcinoma of the lung is one of the main types of lung cancers. Adenocarcinoma of the lung arises from the secretory (glandular) cells located in the epithelium lining the bronchi.
Statistics on Lung Cancer (Adenocarcinoma of the Lung)
Lung cancer is common. One in every 28 Australians will develop lung cancer during their lifetime. Lung cancer is also deadly: it is the commonest cause of cancer death in Australia, accounting for around 23% of male and 15% of female cancer deaths. Lung cancer is more than twice as common in men as in women. Geographically, the tumour is found worldwide, but it is especially common in countries with a high tobacco consumption. Adenocarcinoma of the lung is the commonest type of lung cancer, accounting for 32% of all cases of lung cancer.
Risk Factors for Lung Cancer (Adenocarcinoma of the Lung)
Cigarette smoking is the main predisposing factor. In recent years, it has been recognised that passive smoking (e.g. from a first degree relative in a house of smokers) can also put people at risk. Generally, the risk increases with the number of cigarettes smoked. The link between cigarette smoking and adenocarcinoma is weaker than the link between smoking and other types of lung cancer, but is still the most significant risk factor identified.
Exposure to asbestos increases the risk of developing this tumour. The combination of asbestos exposure plus cigarette smoking is particularly harmful. Other occupational exposures such as exposure to metals including arsenic, chromium and nickel can also increase risk.
Some studies have suggested that diet can play a role in lung cancer risk. Though it is not known how it works, diets high in fruits and vegetables seem to decrease risk.
Radiation exposure damages the DNA material within the cells and can also cause lung cancer. Radon (a radioactive gas) exposure from our normal surrounding environment, if higher than normal, can predispose to lung cancer. This evidence is mainly based upon population studies which show that people living in areas with a high radon content are prone to increased incidences of a variety of cancers.
Progression of Lung Cancer (Adenocarcinoma of the Lung)
Adenocarcinomas tend to be slow-growing. Spread of the tumour can occur by the lymphatic vessels to lymph nodes located within the lung, mediastinum and thorax. If spread by the blood stream, it can lead to deposits of tumour in the liver, opposite lung, bone and brain.
Example of Lung Cancer. The image to the right is that of a cancerous lung post mortem, showing local growth of the tumour.
Symptoms of Lung Cancer (Adenocarcinoma of the Lung)
Patients with adenocarcinoma of the lung may notice:
- Coughing (8-75%)
- Weight loss (0-68%)
- Shortness of breath (3-60%)
- Chest pain (20-49%): if the tumour involves the chest wall, pain may be localised to this area
- Haemoptysis (coughing up blood): sputum may be streaked with blood
- Non-specific symptoms: fever, weakness, lethargy.
Rarely, patients may present with difficulty swallowing or wheezing.
How is Lung Cancer (Adenocarcinoma of the Lung) Diagnosed?
Blood tests:
- Full blood picture: this may reveal anaemia (low haemoglobin).
- Liver function tests: abnormal liver function tests may suggest that the tumour has spread to the liver.
- Urea and electrolytes: low levels of sodium in the blood may indicate inappropriate secretion of ADH (SIADH), a complication of some types of lung cancer.
Imaging tests:
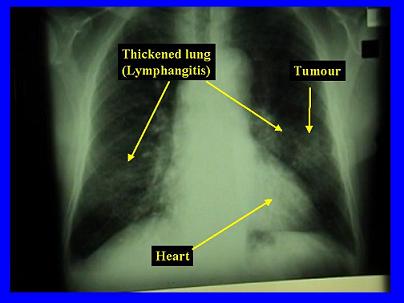
- Chest x-ray: lung cancer may be seen on chest x-ray as a solitary pulmonary nodule or mass. As many as 80% of solitary pulmonary nodules (<4cm diameter) in the over-50 age group are cancer. Chest x-ray may also be used to evaluate the size of the tumour and possible involvement of lymph nodes in the chest. See the example image below.
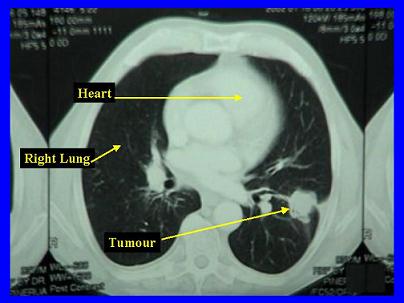
- CT: this is more accurate than chest x-ray, and may be particularly useful in identification of lymph node involvement. See the example image below.
- PET scanning can help to distinguish between benign and malignant solitary pulmonary nodules seen on chest x-ray. PET scanning may also be used in the assessment of nodal spread and metastatic disease.
- Imaging of other organs: if it is suspected that the cancer has spread to other organs, scans of the liver, brain or bone may be required. While imaging tests are helpful in raising the suspicion of lung cancer, diagnosis requires that cancer cells are seen under a microscope. There are a number of ways of obtaining samples of suspected cancer cells:
- Fine needle aspiration biopsy through the skin may be used to investigate suspected lung tumours located on the outside of the lungs.
- Sputum cytology: cells from the sputum (spit) are examined for signs of malignancy (cancer). Sputum cytology may not be very useful in adenocarcinoma of the lung, because the tumours are usually in the periphery of the lung, meaning tumour cells are less likely to be coughed up.
- Bronchoscopy with washings, brushings and biopsy: a bronchoscopy is a camera tube placed through the throat into the airways of the lungs. Samples of the cells from the airways can be taken with washing, brushing, or biopsy.
Prognosis of Lung Cancer (Adenocarcinoma of the Lung)
The prognosis (probable outcome) depends on the stage of the tumour. Cancer staging is a tool which allows prediction of patient outcomes, and helps decide on the best treatment options. It takes into account various features of a tumour in an individual patient, which can then be compared to other patients with similar tumour features. Staging of adenocarcinoma of the lung is based on the TNM (Tumour, Node, Metastasis) system. ‘Tumour’ refers to tumour size, which is measured in centimetres. ‘Node’ refers to the presence of cancerous cells in regional lymph nodes. ‘Metastasis’ refers to the spread of cancer beyond regional lymph nodes to other organs of the body.
Tumour size (T):
- Tx: Primary tumour not able to be assessed
- T0: No evidence of primary tumour, ie. cancer cells seen on sputum sampling or bronchial washing only
- Tis: Carcinoma in situ
- T1: Tumour 3 cm or less, surrounded by pleura, without evidence of invasion more proximal than the lobar bronchus.
- T2: Tumour with any of the following features:
- >3cm in greatest dimension
- Involves main bronchus, 2cm or more distal to the carina
- Invades visceral pleura
- Associated with atelectasis or obstructive pneumonitis, extending to the hilar region but not involving the entire lung.
- T3: Tumour of any size,
- directly invading the chest wall, diaphragm, mediastinal pleura or parietal pericardium; or tumour in the main bronchus; or
- in the main bronchus, less than 2cm distal to the carina, but without involvement of the carina; or
- with associated atelectasis or obstructive pneumonitis of the entire lung
- T4: Tumour of any size, invading the mediastinum, heart, great vessels, trachea, oesophagus, vertebral body, carina; or with separate tumour nodules in one lobe, or with malignant pleural effusion
Regional lymph nodes (N):
- NX: Regional lymph nodes not able to be assessed
- N0: No regional lymph node metastasis
- N1: Metastasis in ipsilateral peribronchial and/or ipsilateral hilar lymph nodes and intrapulmonary nodes, including involvement by direct extension
- N2: Metastasis in ipsilateral mediastinal and/or subcarinal lymph nodes
- N3: Metastasis in contralateral mediastinal, contralateral hilar, ipsilateral or contralateral scalene, or supraclavicular lymph nodes
Distant Metastasis (M):
- MX: Distant metastasis not able to be assessed
- M0: No distant metastasis
- M1: Distant metastasis, including separate tumour nodule(s) in a different lobe (ipsi- or contralateral).
Using this classification, non-small cell lung cancers are grouped into stages as follows:
- Stage 0: TIS N0 M0
- Stage Ia: T1 N0 M0
- Stage Ib: T2 N0 M0
- Stage IIa: T1 N1 M0
- Stage IIb: T2 N1 M0, T3 N0 M0
- Stage IIIa: T1 N2 M0, T2 N2 M0, T3 N1 M0, T3 N2 M0
- Stage IIIb: any T N3 MO, T4 any N M0
- Stage IV: any T any N M1
Using this system, outcomes are best for patients with early stages of disease, with small tumours, no spread to lymph nodes, and no distant spread (metastasis) to other organs. Outcomes are also better for younger patients. Overall, despite treatment, 5-year survival for all types of lung cancer in Australia is not good: 11% for males and 14% for females. Adenocarcinoma has the best prognosis of any type of lung cancer.
How is Lung Cancer (Adenocarcinoma of the Lung) Treated?
- Surgery offers the best chance of cure, but is usually only possible with small tumours that have not yet spread (stage I or II). In some cases, lobectomy may be more appropriate than limited resection.
- If surgical treatment is to be given, the lymph nodes draining the tumour should be sampled and removed if the cancer has spread.
- Patients with tumours which are not suitable for surgical resection can benefit from radiotherapy to the chest.
- Patients with early disease (Stage I or II cancer) who have had the tumour completely surgically removed do not usually need radiotherapy.
- Chemotherapy can increase survival for patients with advanced cancer who are otherwise medically fit. Chemotherapy may also have improve quality of life for these patients.
- If chemotherapy is to be used, combination regimes (using more than one drug together) are better than single-drug regimes. Chemotherapy using platinum-based drugs produces the best results.
New classes of treatment agents, such as biological therapies, are finding a place alongside chemotherapy. Watch this site for breaking news regarding this treatment.
Palliative care
Lung symptoms commonly reported by patients with incurable lung cancer include shortness of breath from pleural effusion, coughing, or haemoptysis (coughing up blood). Pain may be from the lung tumour itself, or from spread (metastasis) to other organs, including bone. Treatment is available for all of these symptoms. In some cases, radiotherapy may be used to manage cancer pain. Spinal cord compression is a complication of bony metastasis which requires urgent treatment.
Lung Cancer (Adenocarcinoma of the Lung) References
- Alberg AJ, Samet JM. ‘Epidemiology of lung cancer’, Chest. 2003, 123:21S-49S
- Beckles MA, Spiro SG, Colice GL, Rudd RM. ‘Initial evaluation of the patient with lung cancer: symptoms, signs, laboratory tests and paraneoplastic syndromes,’ Chest. 2003, 123:97S-104S
- Braunwald, Fauci, Kasper, Hauser, Longo, Jameson. Harrison’s Principles of Internal Medicine. 16th Edition. McGraw-Hill. 2005.
- Cotran RS, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- The Cancer Council Australia. ‘Clinical Practice Guidelines for the Prevention, Diagnosis and Management of Lung Cancer’ [online]. National Health and Medical Research Council. 2004. Available at URL: http://www.nhmrc.gov.au/publications (last accessed 1/4/07)
- Talley NJ, O’Connor S. Clinical Examination Fourth Ed. MacLennan & Petty 2001.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.