Spinal cord compression (SCC) is a common oncological emergency that requires early detection and prompt treatment as it can result in permanent neurological deficits. It is the second most frequent neurological complication of cancer due to vertebral metastases (brain metastases is the most common complication). 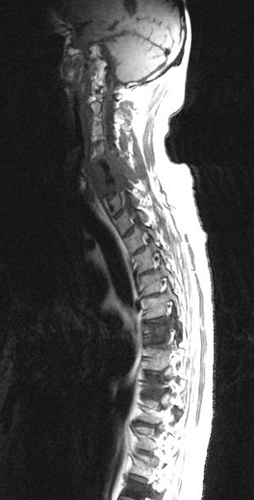
Patients with melanoma, renal cell carcinoma, sarcoma, and multiple myeloma are also at risk of developing Spinal Cord Compression. Image: MRI scan illustrates multiple vertabral metastases causing spinal cord compression.
Spinal Cord Anatomy and Physiology
The spinal cord is a long, cylindrical structure located in the vertebral column that extends from the foramen magnum at the base of the skull to the level of the first lumbar vertebrae. It is part of the central nervous system and is approximately 1cm in diametre, 42-45cm long and weighs around 30 grams. The spinal cord provides a two way conduction pathway, conducting sensory and motor impulses to and from the brain and controlling many reflexes. There are 31 pairs of spinal nerves that leave the spinal cord at regular intervals: 8 cervical, 12 thoracic, 5 lumbar, 5 sacral, and 1 coccygeal. The spinal cord is protected by bone, cerebrospinal fluid and the meninges. The vertebrae (7 cervical, 12 thoracic, 5 lumbar, 1 sacral and 1 coccyx) support the body, the vertebral column surrounds and protects the spinal cord. The meninges are membranes that cover the brain and the spinal cord, there are three: the dura mater (outer), arachnoid (middle) and pia mater (inner). The space between the vertebral column and the outer surface of the dura mater is called the epidural space. The subdural space is next between the inner surface of the dura mater and the arachnoid membrane. Below this is the subarachnoid space, this lies between the arachnoid membrane and the pia mater and is attached to the spinal cord. The cerebrospinal fluid is located in the subarchnoid space which begins in the brain and continues down the spinal cord.
Signs and Symptoms of SCC
Pain: Back pain is usually the first symptom of SCC, it is often constant, dull, aching and sometimes radiating. The pain may increase or progress slowly, it is often referred to as crescendo pain (pain that waxes and wanes). It is exacerbated by movement, especially when flexing the neck or raising the legs, coughing, sneezing, or straining. It is not relieved by lying down although it can be sometimes relieved by sitting the patient upright. Leg pain may occur and be unilateral or bilateral in nature that radiates from the back.
Motor Weakness: This usually follows pain, the time frame for this sign is often variable, from hours to days, weeks or months. Patients may experience stiffness and heaviness of the affected extremity, they may present with an unsteady gait or ataxia (failure of muscle co-ordination) and foot drop.
Sensory Impairment: This usually follows motor weakness, symptoms include loss of sensation, numbness, tingling, pins and needles type feeling and coldness in the affected area.
Autonomic dysfunction: This will occur if the SCC progresses. Loss of bladder control results in urinary retention, frequent small voids, overflow or incontinence. Loss of bowel control such as the urge to defecate, may lead to constipation or incontinence. Loss of sphincter control is often a later sign that is associated with a poor prognosis. Sexual impotence may also manifest. Without identification of the above signs and symptoms and a delay in the appropriate treatment, complete and irreversible paraplegia may develop within hours to days.
Tests and Investigations
Laboratory tests such as a full blood count (FBC) with differential and a biochemistry profile may be ordered by the patients doctor. The results will be useful when differentiating SCC from an infection. A plain x-ray of the spine may be requested in patients suspected of having SCC. As a plain X-ray may not indicate any abnormalities further radiological investigations may be ordered. A bone scan, computerized tomography scan (CT) with contrast, a myelogram or a magnetic resonance imaging scan (MRI) will enable a more definitive diagnosis to be confirmed. The diagnostic test of choice is a MRI as this is a non invasive procedure that provides the best definition of spinal lesions.
Treatment
SCC is an oncological emergency that requires prompt treatment, a delay may result in complete and irreversible paralysis. The goal of treatment is for pain relief, restoration of any neurological deficits, stabilization of the spinal cord and tumour control. Treatment depends on the type of tumour, its location, the speed of onset, the level and severity of the compression and the patients functional level before the onset of symptoms. Treatment in the early stages of SCC is usually effective and includes the following: Radiation therapy is the standard treatment, it resolves pain by decreasing the tumour mass which relieves the SCC. Patients may experience relief of their symptoms within days of starting the therapy and pain is sometimes relieved within hours of commencement. Corticosteroid therapy (dexamethasone) is given to decrease the oedema and cord compression caused by the tumour thus assisting in relieving the patients pain.
It may also assist in improving neurological function. Surgery (laminectomy) may be considered for patients with spinal instability, rapidly progressing neurological deficits, the inability or failure to respond to radiotherapy or a pathological fracture that is causing instability or compression to the spinal cord. Chemotherapy is occasionally used in patients with chemo sensitive tumours such as Hodgkin’s disease or lymphoma. It may be used as adjuvant therapy with radiotherapy or surgery in patients with breast or prostate cancer and multiple myeloma. Palliative care is a treatment option for patients that have failed to respond to either chemotherapy or radiotherapy and are not suitable for surgery. These patients are treated with analgesia, nerve blocks and corticosteroids. Overall the patients prognosis for recovery depends largely on the degree of disability at the time of diagnosis. Around 80% of ambulatory patients will remain so if treated immediately, approximately 30% of non ambulatory patients may regain the ability to walk after treatment. In situations where SCC has already caused complete paralysis the chances of regaining the ability to ambulate are 0 to 10%.
References
Kindly Supplied by Virtual Nursing Education.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







