- Introduction
- Psoriasis in summer
Prevalence
- Risk factors
- Comorbid conditions associated with psoriasis
- Quality of life
- Preventive measures
- Treatment
Introduction
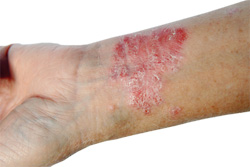
Psoriasis is a skin condition underpinned by dysfunction of the immune system. It occurs in phases of relapse, remission (no symptoms) and exacerbation (severe symptoms). The primary symptom is papulosquamous skin rash, which is a red, scaly rash. Elbows, knees, scalp and trunk are the most commonly affected body parts; however, the disease can affect any body part. In mild cases the rash covers < 2% of the person’s body surface area. Disease is typically considered severe if it affects more than 10% of skin surface area. Up to 20% of people who have psoriasis have extensive skin rash. Joints are often also affected. The skin rash and other symptoms (e.g. those affecting the joints) which psoriasis causes are uncomfortable and may cause itching and burning sensations They also cause embarrassment which can have a serious impact on a person’s wellbeing.
 |
For more information about psoriasis including types, treatments, videos and more, see Psoriasis. |
Psoriasis in summer
The skin symptoms of psoriasis are more likely to improve spontaneously (without treatment) in summer, compared to other times of the year. However, the psychological effects of the condition may be worse during summer due to the need to expose more skin in warm conditions. Because skin rash is a highly visible symptom, it is difficult to hide from other people during summer. However, exposing the skin can be embarrassing and lead to stigma and discrimination.
People with psoriasis may be too embarrassed to participate in summer recreation activities which require the removal of clothing, such as swimming and other sports. In one study, a large proportion of people with psoriasis reported avoiding swimming and/or other sporting activities as a result of their condition. 64% reported that they avoided buying summer clothes such as short sleeved shirts, summer dresses and/or shorts. Wearing seasonally inappropriate clothing (e.g. long sleeves in summer) in an attempt to hide psoriatic skin rash is one measure people resort to in order to hide their condition. However, this strategy is also likely to draw unwanted attention.
Prevalence
Psoriasis is a common condition. Studies from different developed countries have reported that it affects between 1 and 4% of the total population. InAustraliaprevalence is estimated to be between 0.3–2.5% of the population. It is the reason for some 0.3–0.6% of doctor visits overall and 2.6% of all skin-related doctor visits.
Prevalence is low (0.55%) in patients < 10 years of age and increases with increasing age. Men and women are just as likely to have psoriasis; however, young females (< 20 years) have a higher risk of the disorder compared to young males. While it is uncommon to develop psoriasis in childhood or adolescence, those individuals who do tend to have more severe disease. They usually also have family members affected by psoriasis. The psychological effects of the disorder may be greater in patients who develop the condition later in life.
Risk factors
Genetic factors

Race
Caucasians are more likely to experience psoriasis compared to other races. Individuals of Asian ethnicity have a lower risk than Caucasians and the condition is very rare in those of African ethnicity. The disease is also very rare in individuals of Native American descent.
Nutritional disorders
The risk of psoriasis is increased in individuals with type 2 diabetes or metabolic syndrome and those who are obese.
Stress
Emotional stress is associated with acute attacks of psoriasis. In one study 60% of people reported a stressful life event in the month prior to acute symptoms of psoriasis.
Injury
There is clear evidence that injury is a risk factor for the development of psoriasis.
Location
Psoriasis is less common in regions characterised by warm sunny weather conditions.
Biological factors
Biological factors (factors relating to the person’s body), including infection and medication use, also play a role in the development of psoriasis.
Infection
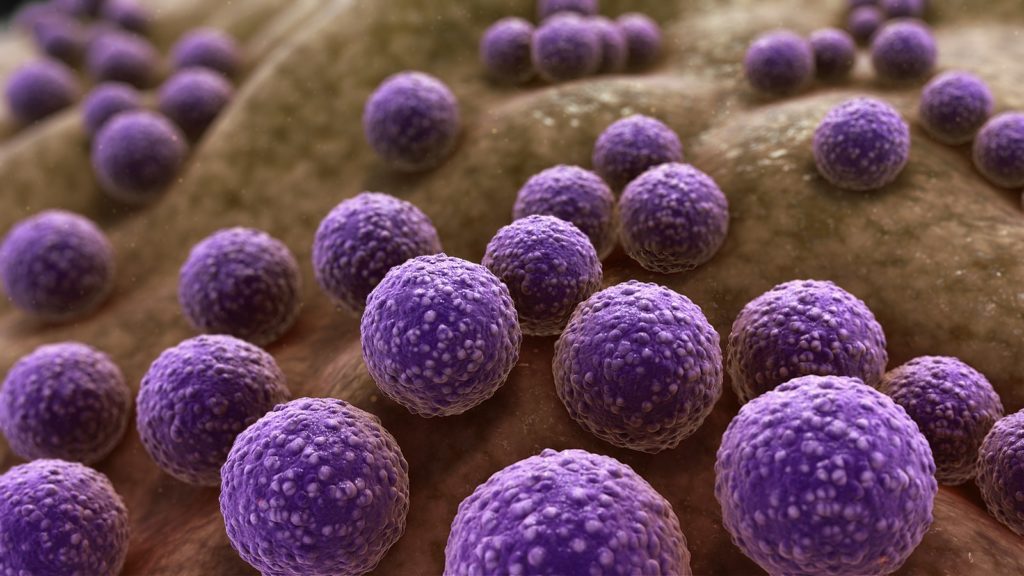
Individuals infected with HIV and those with chronic streptococcal infection have an increased risk of developing psoriasis. Those who already have psoriasis when they are infected with HIV or streptococci are likely to experience worsening psoriasis.
Medications use
Using some medications can trigger the symptoms of psoriasis to worsen. Medicines known to have this effect include:
- Lithium;
- Anti-malarials;
- Corticosteroids (if a person stops taking them too quickly); and
- Beta blockers.
Smoking
Smoking is an important modifiable risk behaviour for psoriasis. In one study smokers were 1.3 times more likely to develop psoriasis compared to non-smokers.
Alcohol
Alcohol consumption has affects on most body systems and organs, including the skin. Psoriasis has also been associated with alcohol consumption in some studies, although others have found no association.
Comorbid conditions associated with psoriasis

- Cardiovascular disease;
- Psoriatic arthritis a form of arthritis which affects 25% of psoriasis patients;
- Metabolic syndrome and diabetes mellitus;
- Hypertension;
- Hyperlipidaemia;
- Obesity;
- Cancer, particularly skin cancer and lymphoma, although it is unclear if psoriasis or its treatment underlies the increased risk of cancer;
- Psychological conditions including depression and mood disorders;
- Alcoholism;
- Other conditions underpinned by immune dysfunction including colitis and Crohn’s disease.
Epidemiological evidence shows that the risk of some conditions (diabetes and obesity) increases with increasing psoriasis severity.
Quality of life
How quality of life is affected
Psoriasis skin rash is typically itchy and changes the appearance of skin causing redness and scaling. Psoriatic rash is physically uncomfortable, but also associated with a range of psychological problems. It is often misinterpreted by others to be a symptom of a contagious skin disorder or other condition. For example 57% of people with psoriasis report others believe their condition to be contagious, and 9% that their psoriasis rash was mistakenly interpreted to be a symptom of acquired immune deficiency syndrome (AIDS). Psychosocial problems are particularly likely and more severe in people with affected skin on the face, hands or other commonly exposed body areas. They may also be worse in summer, when warm conditions lead to many people exposing greater amounts of skin. People with psoriasis may resort to wearing clothing which is inappropriate for hot weather to hide their rash.
Impact on quality of life
The quality of life impact of psoriasis is often significant and people aged < 55 years are most likely to experience negative quality of life effects. The majority of people affected by the condition (79%) report that the condition negatively affects their quality of life. It may affect social, intimate and work relationships, daily living and self perception. Women are more greatly affected in terms of quality of life compared to men.
Relationships
Psoriasis is reported to affect people’s relationships with family members, friends and intimate partners. Those affected by the condition report feeling physically and sexually unattractive. Sexual activity is also often affected, particularly amongst those ≤ 54 years, amongst whom 27% report the condition negatively affects their sex life. People with psoriasis may also have difficulty interacting with family or friends and difficulty maintaining friendships. Some 7% of those affected report that they have been excluded from public facilities such as swimming pools, gymnasiums and hair dressing salons and 40% report difficulty getting equal service or treatment at these facilities. This may also affect their ability to maintain social relationships. In one study, 11% of people with psoriasis reported not wanting to have children for fear that they would inherit the condition.
Work
Psoriasis is associated with difficulties finding employment and 6% of workers with psoriasis report experiencing discrimination at work. Those who had a job reported that the condition negatively affected their ability to interact with colleagues and was the cause of an average of 2.3 days off work each year. Absenteeism from work was reported to be the source of some 40% of the total costs associated with the disease (US $11.25 billion annually in theUnited States) in one study. In another, 35% of people with psoriasis reported the condition affected their career and 20% that it impaired their functioning at work. Work-related stress appears to be greater in men with psoriasis compared to women.
Daily living
Daily living activities such as those requiring the use of hands and walking are impacted by psoriasis in a significant minority of those affected (19% and 14% respectively). Of those who also have psoriatic arthritis, 66% experienced difficulty using their hands and 63% experienced difficulty walking. Sleep is also impacted in many people, with > 20% reporting sleep difficulties associated with the condition. Sitting or standing for long periods of time or performing duties at work is also difficult for some people affected by psoriasis.
Patients with severe psoriasis report their daily living is affected 10% of the time. Treating psoriasis may be time consuming and on average those using topical treatments like skin creams report spending 26 minutes per day applying the treatments. The impact on physical and mental functioning associated with the condition is comparable to that associated with arthritis, depression, cancer and heart disease.
Economic hardship
Psoriasis creates economic hardship for those affected by limiting their ability to work and their income earning capacity, and also due to the cost associated with managing the condition. In a study of patients in theUnited Kingdom, 31% reported the condition caused them financial distress. Treatment may be expensive, particularly new biological therapies.
Psychological health

Preventive measures
Psoriasis is a chronic disease for which there is currently no cure. Those affected will be affected for life. While nothing can cure the immune dysfunction which causes psoriatic skin rash, lifestyle measures reduce the severity of the symptoms for many people.
Avoiding triggers
Avoiding things which trigger psoriasis skin symptoms is an important preventive measure. Common triggers include:
- Stress;
- Some drugs, particularly lithium, beta-blockers, interferons and anti-malarials).
Reducing alcohol consumption
Increasing alcohol consumption is associated with increasing disease severity in men, and both men and women who consume alcohol have an increased risk of psoriasis. Therefore, reducing alcohol consumption is an important behaviour for preventing psoriatic skin rash.
Smoking
Smokers are 1.3 times more likely to develop psoriasis compared to non-smokers. Quitting smoking is a key lifestyle measure for reducing risk of the disease. Quitting smoking (and reducing alcohol consumption) are both important parts of treatment, as use of either reduces the likelihood that treatment will be effective. Individuals who drink too much alcohol are less likely to take their psoriasis medicines correctly and thus are less likely to get the full benefit of their treatment.
Treatment of psoriasis
Treatment options for people with psoriasis have developed considerably since 2007 and there is now a greater choice of effective therapies on offer. The best choice of treatment depends on the individual being treated and factors like:
- The extent, severity and site of their psoriatic lesions;
- Things which trigger psoriasis symptoms;
- The impact of the disease on quality of life and daily functioning;
- Comorbid disease; and
- factors which may affect treatment compliance.
Although severity of disease influences a person’s psychological response and the quality of life impact they experience, different people respond to psoriasis in different ways. Some people with mild psoriasis are seriously affected by psychological complaints, while others with severe psoriasis have few psychological complaints.
As many different factors influence the best choice of treatment, individuals with psoriasis must speak openly with their doctor about how the disease affects them physically and psychologically. They also need to discuss their treatment priorities with the doctor. While treatment aims to relieve the skin symptoms, people receiving treatment may also be concerned (and in some cases may be more concerned) about improving quality of life, or finding a treatment that is convenient.
It’s also important to speak to the doctor about the aims of treatment and to understand that treatment may alleviate the symptoms of psoriasis, but cannot cure the underlying immune dysfunction which causes the disease. Psoriasis is a life-long condition and is associated with significant morbidity (ill health). However, people with the condition may underestimate the severity of their condition and the impact psoriasis has on their health. For example, in one study 39% of people reported psoriasis affected > 10% of skin surface; however, only 17% classified their disease as severe.
Understanding the severity of the disease is important for ensuring the best treatment is chosen, particularly for those whose psoriasis fails to respond to topical treatments (those applied directly to the skin rash) like creams and gels. These people need to weigh up the risks and benefits of systemic treatments such as medicines and phototherapy, which can have significant side effects and in some cases require frequent doctor appointments. If the impact of psoriasis is underestimated, the benefits of treatment may also be underestimated in the risk benefit analysis.
Pharmacotherapy
Topical treatments

Topical treatments are used by 87% of people with severe psoriasis. In cases of mild psoriasis (affecting < 5% of body surface area) they are highly effective. Topical therapies also play an important role in the management of moderate-severe disease because when people use creams and gels, they do not need to use as much medicine or other forms of systemic treatment which have greater side effects and/or are less convenient to use. When used alone, creams and gels are generally not enough to control severe psoriasis.owever the majority of people with severe disease report never having used more intensive photo and systemic therapies. This indicates that those with severe disease there is a greater role for topical treatments to be used in combination with more intensive therapies. Individuals who fail to control their skin rash, should consider and discuss with their doctor, using systemic therapies.
Phototherapy
Phototherapy should be considered by all adults with extensive psoriatic skin rash which does not improve adequately with topical treatment. Two options are available. UVB therapy (which uses UVB rays) is most appropriate for patients with localised skin rash (restricted to a particular area of the body) while PUVA photochemotherapy is most appropriate for thick psoriatic rash.
Phototherapy is a highly effective form of treatment. 64% of people who had used phototherapy in oneUKstudy reported a good or excellent response. However, only a minority (23%) of people with severe psoriasis have used phototherapy. One thing which limits the use of phototherapy is the need for treatment to be administered in a specialised facility. For the individual being treated this means time, travel and inconvenience. However, in cases of severe disease the benefits of treatment might outweigh the time and inconvenience involved in using it.
Systemic treatments
Systemic treatments are medicines which affect the entire body, not only the site of psoriatic skin lesions. For example, medicines which are swallowed enter the blood stream and are distributed throughout the entire body. They are typically only used to treat psoriatic skin rash which affects > 5% of the body surface area and cannot be adequately controlled using topical or phototherapy. They include:
- Corticosteroids (cyclosporin);
- Folic acid antagonists (methotrexate); and
- Retinols (acitretin).
Methotrexate is considered the best choice and 70% of people with psoriasis who use it report a good or excellent response to the treatment. However, it is used by only a minority (27%) of people with severe disease.
Biological agents
Novel biologic agents for psoriasis treatment target the processes which underpin the development of psoriatic lesions. Psoriasis is underpinned by a dysfunctional immune response, so biological agents target cells in the immune system including cytokines and T cells. These cells play a role in regulating the immune system’s response, including the dysfunctional (overactive) immune responses which cause psoriatic rash to develop. Targeting these cells modifies (reduces) the immune system response and reduces psoriatic skin rash.
Because biological agents interfere with the immune system, it is important for people who use these treatments to undergo screening for infectious disease before they begin using them. Any severe infections, including tuberculosis and hepatitis B or hepatitis C should be treated before biological therapy commences.
Alternative therapies
Due to the high rate of side effects with conventional psoriasis treatment, many people with the condition consider using alternative therapies. In one survey almost half (43%) of the respondents reported trying over-the-counter medications or alternative therapies including herbal remedies, acupuncture and relaxation to treat psoriasis. 10% of the people were using some form of alternative therapy at the time of the survey. The majority (52%) reported no improvement in their condition with use of alternative therapy. There is little evidence to suggest that alternative therapies are effective in treating psoriasis. However, those who are interested in trying alternative therapies should discuss the available evidence with their doctor.
Diet
Dietary modifications may reduce the severity of psoriatic rash; however, evidence is limited. As the condition is underpinned by inflammation, an anti-inflammatory diet may be of benefit. Such a diet is based on the consumption of omega-3 fatty acids, whole grains, legumes, and fresh fruit and vegetables and avoidance of omega-6, saturated and trans fats and processed foods. It should also include the use of spices with anti-inflammatory properties such as ginger, cumin, basil and turmeric.
Identifying and avoiding food allergens which trigger psoriasis is another possible strategy. Many people with psoriasis are gluten intolerant and a gluten-free diet may be beneficial for this group. Obesity is a risk factor for the condition and maintaining a healthy weight is important.
Dietary supplements

Topical therapies
A range of non-pharmaceutical topical therapies have also been shown to improve psoriasis. Cream containing aloe vera extract reduced the extent of psoriatic lesions compared to no treatment in one study. Emollients (skin softeners), particularly those containing ceramides (fatty acids which hold water), regulate the water-holding capacity of the skin and have been show to reduce the scaliness of psoriasis.
Lifestyle treatments
Lifestyle measures which may assist in the treatment of psoriasis include:
- Bathing and sun bathing at theDead Seafor a period of 4 weeks;
- Increasing physical activity, particularly outdoor physical activity;
- Weight management for those with excessive body mass index (BMI) (who are overweight or obese);
- Quitting smoking;
- Reducing alcohol consumption; and
- Stress management.
Treatment of comorbid conditions
Psychotherapy is essential for people who experience ongoing psychological difficulties as a result of their psoriasis. Medical treatment may not be appropriate as many medicines used for psychological conditions may worsen psoriasis. People who also have alcohol dependence disorder (are alcoholic) are less likely to respond to treatment and less likely to comply with their treatment plan (e.g. take their medicine as scheduled). These people may also need to access alcohol rehabilitation services.
References
- Menter A, Gottlieb A, Feldman SR, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: Section 1. Overview of psoriasis and guidelines of care for the treatment of psoriasis with biologics. J Am Acad Dermatol. 2008; 58(5): 826-50. [Abstract]
- Herrier RN. Advances in the treatment of moderate-severe psoriasis. Am J Health Sys Pharm. 2011; 68: 795-806. [Abstract]
- GriffithsCE, Barker JN. Pathogenesis and clinical features of psoriasis. Lancet. 2007; 370(9583): 263-71. [Abstract]
- Dediol I, Buljan M, Buljan D, et al. Associations of psoriasis and alcoholism: psychodermatological issues. Psychiatria Danube. 2009; 21(1): 9-13. [Abstract | Full Text]
- Gelfand JM, Neimann AL, Shin DB, et al. Risk of myocardial infarction in patients with psoriasis. JAMA. 2006; 296(14): 1735-41. [Abstract | Full text]
- Krueger G, Koo J, Lebwohl M, et al. The impact of psoriasis on quality of life: Results of a 1998 National Psoriasis Foundation patient-membership survey. Arch Dermatol. 2001; 137(3): 280-4. [Abstract | Full text]
- Barankin B DeKoven J. Psychosocial effects of common skin disorders. Can Fam Phys. 2002; 48: 712-8. [Abstract | Full Text]
- Roberson EDO, Bowcock AM. Psoriasis genetics: breaking the barrier. Trends Genet. 2010; 26(9): 415-23. [Abstract | Full text]
- Lassus A, Geiger JM, Nyblom M, et al. Treatment of severe psoriasis with etretin. Br J Dermatol. 1987; 117(3): 333-41. [Abstract]
- Ramsey B, O’Reagan M. A survey of the social and psychological effects of psoriasis. Br J Dermatol. 1988; 118(2): 195-201. [Abstract]
- Swanbeck G, Inerot A, Martinsson T, et al. Genetic counselling in psoriasis: empirical data on psoriasis among first-degree relatives of 3095 psoriatic probands. Br J Dermatol. 1997; 137(6): 939-42.[Abstract]
- Magin P, Adams J, Heading G, et al. Patients with skin disease and their relationships with their doctors: a qualitative study of patients with acne, psoriasis and eczema. Medical Journal of Australia. 2011; 190: 62-64. [Abstract]
- Gelfand JM, Weinstein R, Porter SB, et al. Prevalence and treatment of psoriasis in the United Kingdom: A population-based study. Arch Dermatol. 2005; 141(12): 1537-41. [Abstract | Full text]
- OkaA, Mabuchi T, Ozawa A, Inoko H. Current understanding of human genetics and genetic analysis of psoriasis. Japan Dermatol Assoc. 2012; 39: 231-41. [Abstract | Full text]
- Traub M, Marshal K. Psoriasis- Pathophysiology, conventional and alternative approaches to treatment. Alt Med Rev. 2007; 12(4): 319-31. [Abstract | Full Text]
- Chuh A, Wong W, Zawar V. The skin and the mind. Aust Fam Phys. 2006; 35(9): 723-5. [Full Text]
- Neimann AL, Shin DB, Wang X, et al. Prevalence of cardiovascular risk factors in patients with psoriasis. J Am Acad Dermatol. 2006 Nov; 55(5): 829-35. [Abstract]
- Foulkes AC, Grindlay DJC, Griffiths CEM, Warren RB. What’s new in psoriasis? An analysis of guidelines and systematic reviews published in 2009-10. Clin Experimental Dermatol. 2011; 36: 585-9. [Abstract | Full text]
- Christophers E. Psoriasis: Epidemiology and clinical spectrum. Clin Exp Dermatol. 2001; 26(4): 314-20. [Abstract]
- Langham S, Langham J, Goertz H, Ratcliffe M. Large-scale, prospective, observational studies in patientswith psoriasis and psoriatic arthritis: A systematic and critical review. BMC Medical Research Methodology. 2011; 11: 32. [Abstract | Full Text]
- Murphy G, Reich K. In touch with psoriasis: topical treatments and current guidelines. J Eu Acad Dermatol Venereol. 2011; 25(S4): 3-8. [Abstract | Full text]
- Merideth F, Ormerod AD. Patient preferences for psoriasis treatment: process characteristics considered more important than outcome attributes. Exp Rev Pharmacoecon Outcomes Res. 2012; 12(2): 145-7. [Abstract | Full Text]
- Stern RS, Lunder EJ. Risk of squamous cell carcinoma and methoxsalen (psoralen) and UV-A radiation (PUVA): A metaanalysis. Arch Dermatol. 1998; 134(12): 1582-5. [Abstract | Full text]
- Sullivan R, Preda V. Treatments for severe psoriasis. Australian Prescriber. 2009; 32: 14-18. [Full Text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.