Treatment of psoriasis
Psoriasis is a disease which affects multiple systems within the body, predominantly the skin and the joints. Skin disease which can present in multiple different ways and degrees of severity is the hallmark of psoriasis. The severity of psoriasis is defined in terms of which body parts and how much body surface area are involved. When the hands, feet, face and/or genital regions are involved, the impact on the individual and how they go about their daily activities is more significant.
Research from around the world has estimated that between 1–3% of the population have psoriasis. In Australia, between 0.3 and 2.5% of people are affected. It is well established that there are different types of psoriasis with psoriasis vulgaris being the most common form. Other subtypes include flexural psoriasis, guttate psoriasis, erythrodermic psoriasis, generalised pustular psoriasis, palmoplantar psoriasis in addition to psoriasis that involves certain body sites including the scalp and nails.
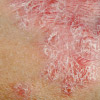 |
For more information about the different types of psoriasis and the characteristics that define them, see Psoriasis Subtypes. |
So what is the best treatment for psoriasis? Your treating doctor will decide how to treat your psoriasis based on your age, your type of psoriasis, the site and extent of skin involvement, any previous treatment you may have had and any other medical problems you may have.
Several treatment options exist which include newer biologic agents, topical medications, phototherapy and systemic agents. However, there is no available treatment for curing psoriasis; all of the therapies described below instead aim to reduce or eliminate symptoms.
Biologic agents
Within this class of drugs, there are several separate agents available which work on different pathways in the inflammatory cascades;
- IL-12/IL-23 inhibitors including ustekinumab (e.g. Stelara) and briakinumab (not currently available in Australia);
- TNF alpha antagonists such as etanercept (e.g. Enbrel), adalimumab (e.g. Humira) and infliximab (e.g. Remicade);
- T cell modulators including alefacept and efalizumab (neither is currently available in Australia).
IL-12/IL-23 inhibitors
Ustekinumab is the newest biologic agent for the treatment of moderate to severe psoriasis. This agent targets two inflammatory molecules and stops them from participating in the inflammatory process involved in psoriasis.
Ustekinumab was approved by the FDA in 2009. It is given via an injection under the skin at 0 and 4 weeks and then repeated every 12 weeks. This agent has shown promising results in early research trials.
When compared to placebo, ustekinumab has comparable side effects with serious adverse events reported in less than 1% of individuals receiving this treatment. The long term safety of this agent is only now becoming available and, similar to other biological agents, it carries a warning with regards to potentiating infection and underlying cancer. However, a trial looking at the long term safety of ustekinumab in people exposed for up to 3 years failed to demonstrate an increased risk of infection or malignancy when compared to the general population.
TNF alpha antagonists
These agents bind with tumour necrosis factor (TNF) a key molecule involved in the inflammatory process. Importantly this class of drugs suppresses the immune system and therefore predisposes individuals to developing severe infections, including tuberculosis and cancers. While these serious side effects occur in less than 1% of people, they have the potential to be lethal. Other possibly side effects are localised redness at the injection site affecting 4–24% of individuals. Approximately 22% of individuals receiving infliximab via an infusion experienced a reaction consisting of chills, headache, flushing and breathing difficulty. Uncommon side effects include liver damage, kidney damage and blood disorders.
T cell modulators
Two biological agents, alefacept and efalizumab, are classified within this category although neither is currently available in Australia. They work on a subset of lymphocytes known as the T cells and thereby inhibit the inflammatory process responsible for psoriasis. Efalizumab was withdrawn from the market in 2009 due to adverse neurological side effects in a small group of individuals.
Alefacept is given as an injection once a week for 12 weeks. A second 12 weeks course can be given as long as the individual’s lymphocyte count is within the normal range. Repeat courses of alefacept have been shown to almost double or markedly increase the response rate. Lymphocyte counts need to be checked every 2 weeks through a blood test while using this agent. The main side effects are fatigue and joint pains which occur in approximately 20% of individuals.
Topical therapy

Topical therapy has many advantages including that they can be applied directly to the problematic area, are generally safe and well tolerated. Disadvantages include the time required to apply the cream/lotion and the need to apply the cream/lotion on a regular basis over time. Research has shown that up to 40% of individuals find it difficult to adhere to a program of regular application of topical agents. The most common reasons cited for this are frustration with medication effectiveness, unclear instructions on how to apply the cream/lotion, inconvenience and time constraints. Your treating doctor can assist in creating a regime which works best for you and provide simple instructions on how to apply the cream/lotion.
The four main types of topical agents available are topical corticosteroids, vitamin D analogues, tazarotene and calcineurin inhibitors which are explained below.
Topical corticosteroids
Topical corticosteroids are the most commonly prescribed agent for mild psoriasis. Corticosteroids work through reducing inflammation, the process involved in the development of psoriasis. Steroids come in varying strengths, with lower dose steroids being reserved for the face and skin folds, thin skinned areas and for use on children. Medium to high strength steroids are used on other areas of the skin and in adults. The dose of steroid which is delivered to the skin can also be increased through using dressings over the affected areas.
The most common side effects associated with steroids are those relating to skin fragility. These include thinning of the skin, telangiectasia, stretch marks and acne, folliculitis and bruising. Application of steroid creams may also exacerbate other skin conditions that you have including rosacea, dermatitis and fungal infections.
Non-skin related side effects are not as common and are more likely to occur when high strength steroids are applied to large body surface areas. When steroids are used over a prolonged period of time side effects may include Cushing’s syndrome, osteonecrosis of the femoral head, cataracts and glaucoma. All of the topical steroids are pregnancy category C and are not recommended while breastfeeding.
Vitamin D analogues
The vitamin D analogues include calcipotriene, calcipotriol (e.g. Daivonex, Daivobet) and calcitriol. These work by binding to the vitamin D receptor which blocks the overproduction of skin cells responsible for psoriasis. These agents are generally considered to be less effective than topical steroids but are often used in combination with these agents to reduce the skin related side effects associated with topical steroids. The combination of the vitamin D analogue calcipotriene and the topical corticosteroid betamethasone propionate (e.g. Diprosone, Eleuphrat) has demonstrated superior results in mild to severe psoriasis when compared to either agent used on its own. The recent introduction of calcitriol, another form of vitamin D, offers a less irritating option for sensitive skin areas including the face and skin creases.
In plaque-type psoriasis 70 to 74% of people treated with either calcitriol or calcipotriene ointment showed a marked improvement in skin disease as compared with 18 to 19% in the placebo group. Sixty percent of scalp psoriasis treated with calcipotriene solution showed clearance or marked improvement, compared to 17% in the placebo group. Vitamin D analogues, however, have a slower onset of action than topical corticosteroids but tend to work for a longer period of time. One study found that 48% of individuals treated with calcitriol ointment had no skin disease 8 weeks later as opposed to only 25% of individuals treated with topical corticosteroids.
Local skin irritation is the most common side effect of vitamin D analogues, affecting up to 35% of people taking these medications. These side effects often subside with ongoing treatment. Vitamin D analogues can also cause low calcium levels and suppression of parathyroid hormone but these side effects are rare if the recommended dose is used.
Tazarotene
Calcineurin inhibitors
The most common side effect of the calcineurin inhibitors is burning and itching that generally reduces with ongoing use and appears to be worse with tacrolimus. The US Food and Drug Administration implemented a warning for both of these agents in 2005 as little is known about their long term safety and the potential development of cancers. Research to date, however, fails to identify a relationship between calcineurin inhibitors and cancer. Both agents are not recommended in pregnancy or in breastfeeding mothers.
Other topical agents
Other topical preparations including tar, anthralin and salicylic acid which played important roles in the treatment of psoriasis historically have now been superseded by more effective and cosmetically acceptable agents.
Phototherapy
UVB is the treatment of choice for initial phototherapy in younger people and in people whose psoriasis improves with exposure to sunlight. In cases that have not responded well to treatment with topical steroids or where the area affected is too large or widespread, phototherapy may be considered. UVB has been used successfully in the treatment of pregnant women and is considered first line therapy for pregnant women with plaque and guttate psoriasis. Research looking at the use of UVB in children is limited and this mode of treatment should therefore be used with caution.
If your doctor recommends phototherapy they will need to perform a thorough examination to exclude conditions that could be made worse by phototherapy including systemic lupus erythematosus, xeroderma pigmentosum, skin disorders made worse by exposure to sunlight, skin cancer or a suppressed immune system.
UVB phototherapy
Traditional broad band UVB radiation has been used in the treatment of psoriasis for more than 75 years. UVB works through several mechanisms which results in reduce production of skin cells responsible for inducing psoriasis.
In recent years, normal band UVB (NB-UVB) has replaced broad band (BB-UVB) in most phototherapy centres as it has shown to be more effective. NB-UVB is generally given on three separate occasions in a week. Moderate psoriasis can be cleared with around 6 weeks of phototherapy and its effects will last from 3–6 months. Both eye goggles and genital shields need to be worn during phototherapy to protect these sensitive regions. Your doctor will determine the correct dose of phototherapy based on your skin type.
Short-term side effects associated with UVB include redness, itching, burning and stinging of the skin. Reactivation of herpes simplex virus is another potential side effect of this treatment. Premature aging of the skin as occurs with prolonged exposure is a long-term side effect. Long-term exposure has the potential to cause genital cancers which is why wearing genital shields is important. The biggest barriers to phototherapy are the inconvenience of frequent treatments, the travel to specialised facilities and the significant time commitment involved.
UVB can be used in combination with topical, systemic, PUVA and biological therapies. The addition of topical corticosteroids has no added benefit when used in combination with UVB therapy.
Targeted phototherapy

The advantage of targeted phototherapy is that it can selectively target affected psoriatic lesions without affecting surrounding healthy skin. Research into the use of lasers for psoriasis shows promising results with 84% of individuals achieving more than 75% clearance after two treatments and 72% of individuals being completely cleared of their psoriasis after an average of 6.2 treatments. The major limitation of laser treatment is that the psoriasis tends to recur 3–4 months after stopping therapy.
Research into the dose and frequency of laser administration in addition to its long term safety is limited. Data looking at dosage and scheduling of targeted phototherapy as well as long term safety are limited. The targeted nature limits adverse effects to the irradiated area which may include redness, burning and tanning of the skin. As with phototherapy, the laser should be used with caution in individuals who have skin conditions made worse by exposure to sunlight.
PUVA photochemotherapy
PUVA refers to the combination of oral psoralen and UVA light. PUVA is reserved for individuals who have had psoriasis for a long time in addition to individuals who have not responded to UVB therapy, those with thicker plaques and those who have psoriasis of the hands, soles or nails. PUVA can also be used in the form of a psoralen cream applied directly to the skin followed by subsequent exposure to UVA 30 minutes later.
The tablet form of psoralen should be taken 1.5 hours before exposure to the UVA radiation, preferably on an empty stomach to enhance absorption. Treatment is usually given 2–3 times a week with at least 48 hours between treatments in an effort to reduce side effects.
PUVA typically results in clearing of psoriasis within about 24 treatments with remissions lasting between 3 and 6 months. Some people then require maintenance with a regimen of one to two treatments per month, depending on the aggressiveness of the psoriasis. Two large studies conducted in Europe demonstrated that PUVA therapy was successful in 89% of individuals achieving complete clearance of psoriasis in an average of 20–25 treatments.
Common minor side effects of PUVA include redness, itchiness, dry skin, change to skin colour, nausea and vomiting. With long term PUVA therapy most individuals develop premature aging of the skin and there is an increased risk of cataract formation. As with other forms of phototherapy care should be exercised in people with skin conditions made worse by exposure to the sunlight and in individuals with a history of skin cancer.
Systemic therapy
Systemic therapy has been used for the treatment of psoriasis over the last 20 years. Two main agents exist within this category, namely cyclosporin and methotrexate. Your doctor will consider systemic therapy if your psoriasis is not adequately controlled with either topical agents or phototherapy.
Cyclosporin
Cyclosporin works by blocking the release of messengers between cells, known as cytokines, which are responsible for inducing inflammation. Cyclosporin is generally used in the setting of palmoplantar pustulosis, erythrodermic and nail psoriasis in addition to being the systemic treatment of choice in women who are pregnant or breast feeding. Although cyclosporin is ideally suited for short periods of time, it can also be used in some cases to control psoriasis over a longer period of time. Cyclosporin is also a good treatment option for people who also have hepatitis C.
Cyclosporin tends to work quickly in clearing psoriasis and while using this agent it is unlikely that the psoriasis will recur. The major side effects associated with this drug are high blood pressure and kidney damage, the risk of which increases with increasing doses of cyclosporin. For this reason it is recommended that treatment with cyclosporin be limited to 12–24 months of duration. If prescribed cyclosporin, your doctor will check your blood pressure and kidney function through blood tests on a regular basis to monitor for these side effects.
Methotrexate
Methotrexate is started at a low dose and gradually increased over a period of 4 weeks to reach a target dose of between 15 and 25 mg/week. To reduce the risk of side effects a second agent called folic acid is usually prescribed to be taken with methotrexate, for 1–3 days starting 48 hours after the first dose of methotrexate. Individuals who don’t tolerate the drug when taken orally have the option of receiving the drug via an injection.
Methotrexate is generally well tolerated and can be used in the long term. Liver damage is one of the main side effects and is proportional to drug dose. For this reason your doctor will usually perform a series of tests to monitor your liver function on a monthly basis initially and then second monthly after the first 6 months.
Acitretin
Acitretin (e.g. Neotigason, Acitretin Actavis) is an oral retinoid which interferes with the production of cells involved in the inflammatory process. It takes 3–6 months for this agent to reach its optimal effect. This agent does not suppress the immune system and can therefore be safely used in individuals who have long standing infections or a history of cancer. This agent is particularly useful for individuals with erythrodermic and pustular psoriasis. Acitretin can also be used in combination with topical agents (corticosteroids or vitamin D analogues) or phototherapy. Acitretin is known to cause birth defects and therefore cannot be used in pregnant women.
Conclusion
Treatment of psoriasis needs to take into account the age of the individual, the type of psoriasis, the site and extent of skin involvement, previous treatment and any associated medical problems. For mild to moderate disease, treatment options include topical corticosteroids, vitamin D analogues or oral retinoids. Where skin disease is more extensive or associated with disfigurement or disability, phototherapy, systemic therapy or biological therapy is indicated.
References
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: Section 6. Guidelines of care for the treatment of psoriasis and psoriatic arthritis: Case-based presentations and evidence-based conclusions. J Am Acad Dermatol. 2011;65(1):137-74. [Abstract]
- Murphy G, Reich K. In touch with psoriasis: Topical treatments and current guidelines. J Eur Acad Dermatol Venereol. 2011;25(Suppl 4):3-8. [Abstract | Full text]
- Weger W. Current status and new developments in the treatment of psoriasis and psoriatic arthritis with biological agents. Br J Pharmacol. 2010;160(4):810-20. [Abstract | Full text]
- Magin PJ, Adams J, Heading GS, Pond CD. Patients with skin disease and their relationships with their doctors: A qualitative study of patients with acne, psoriasis and eczema. Med J Aust. 2009;190(2):62-4. [Abstract | Full text]
- Green L. An overview and update on psoriasis. Nurs Stand. 2011;25(35):47-55. [Abstract]
- Reich K, Bewley A. What is new in topical therapy for psoriasis? J Eur Acad Dermatol Venereol. 2011;25(Suppl 4):15-20. [Abstract | Full text]
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 3: Guidelines of care for the management of psoriasis with topical therapies. J Am Acad Dermatol. 2009;60(4):643-59. [Abstract]
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 5: Guidelines of care for the management of psoriasis with phototherapy and photochemotherapy. J Am Acad Dermatol. 2010;62(1):114-35. [Abstract]
- Herrier RN. Advances in the treatment of moderate to severe plaque psoriasis. Am J Health Syst Pharm. 2011;68(9):795-806. [Abstract]
- Lapolla W, Yentzer BA, Bagel J, et al. A review of phototherapy protocols for psoriasis treatment. J Am Acad Dermatol. 2011;64(5):936-49. [Abstract]
- Sullivan JR, Preda VA. Treatments for severe psoriasis. Aust Prescr. 2009;32:14-8. [Full text]
- Paul C, Gallini A, Maza A, et al. Evidence-based recommendations on conventional systemic treatments in psoriasis: Systematic review and expert opinion of a panel of dermatologists. J Eur Acad Dermatol Venereol. 2011;25(Suppl 2):2-11. [Abstract]
- Maza A, Montaudié H, Sbidian E, et al. Oral cyclosporin in psoriasis: A systematic review on treatment modalities, risk of kidney toxicity and evidence for use in non-plaque psoriasis. J Eur Acad Dermatol Venereol. 2011;25(Suppl 2):19-27. [Abstract]
- Montaudié H, Sbidian E, Paul C, et al. Methotrexate in psoriasis: A systematic review of treatment modalities, incidence, risk factors and monitoring of liver toxicity. J Eur Acad Dermatol Venereol. 2011;25(Suppl 2):12-8. [Abstract]
- Garcia-Valladares I, Cuchacovich R, Espinoza LR. Comparative assessment of biologics in treatment of psoriasis: Drug design and clinical effectiveness of ustekinumab. Drug Des Devel Ther. 2011;5:41-9. [Abstract | Full text]
- Gordon KB, Papp KA, Langley RG, et al. Long-term safety experience of ustekinumab in patients with moderate to severe psoriasis (Part II of II): Results from analyses of infections and malignancy from pooled phase II and III clinical trials. J Am Acad Dermatol. 2012;66(5):742-51. [Abstract]
- Wolff K, Johnson R. Fitzpatrick’s Colour Atlas and Synopsis of Clinical Dermatology (6th edition). New York: McGraw Hill Medical; 2009. [Book]
- Psoriasis [online]. Melbourne, VIC: Therapeutic Guidelines; February 2009 [cited 28 May 2012]. [URL link]
- Foulkes AC, Grindlay DJ, Griffiths CE, Warren RB. What’s new in psoriasis? An analysis of guidelines and systematic reviews published in 2009-2010. Clin Exp Dermatol. 2011;36(6):585-9. [Abstract | Full text]
- Dediol I, Buljan M, Buljan D, et al. Associations of psoriasis and alcoholism: Psychodermatological issues. Psychiatr Danub. 2009;21(1):9-13. [Abstract | Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







