- What is bed wetting?
- Statistics
- Risk factors
- Progression
- Symptoms
- Clinical examination
- How is it diagnosed?
- Prognosis
- Treatment
- Bed wetting prevention
- References
What is bed wetting?

Bed wetting can be further classified into primary or secondary bed wetting. The primary form occurs in a child who has never achieved night-time dryness. The secondary form refers to wetting in children who have previously established dryness for a period of 6 months.
Anatomy of the urinary tract
The urinary system is divided into upper and lower sections. The upper urinary system is made up of the kidneys and a tube called the ureter which transports urine from the kidney to the bladder. The lower urinary system consists of the bladder and another tube called the urethra which transports urine from the bladder out of the body. The function of the urinary system is to remove waste products from the body, regulate water and salt balance, and store and transport urine.
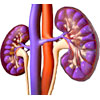 |
For more information on the upper urinary tract, see Anatomy of the Renal System. |
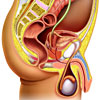 |
For more information on the lower urinary tract in males, see Anatomy of the Male Urogenital System. |
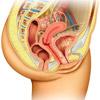 |
For more information on the lower urinary tract in females, see Anatomy of the Female Urogenital System. |
How does the urinary system work?
The process of urination is controlled by a complex circuit of nerves which relay messages between the bladder, the spinal cord and the brain.
Until approximately 2–5 years of age, a simple circuit is involved in the process of urination. At this age, the central nervous system is immature and urination is therefore an involuntary process over which the individual has no control. As the brain develops with age, we develop the ability to control this process and choose an appropriate time and place to urinate.
Micturition, also referred to as urination or voiding, refers to the act of emptying the bladder of urine. It has two phases, known as the filling and voiding phases. Urine collecting in the bladder during the filling phase causes the bladder wall to stretch and sends a signal to the spinal cord. Nerve pathways from the brain to the spinal cord have the ability to block the process of passing urine until it is necessary to void. When voiding is appropriate, the spinal cord sends a message back to the bladder, causing its muscular wall to contract and the external sphincter to relax, forcing urine out of the body via the urethra.
 |
For more information on how urine is produced, stored and voided, see Urinary Tract. |
Impact of bed wetting
Bed wetting is a distressing disorder that carries a significant burden for the affected child and their family. Half of children who wet their bed are teased by their peers, and feelings of bewilderment and humiliation are common. Low self-esteem results from tension in families, social marginalisation and treatment failure. There is often a social impact in that the child is reluctant to participate in sleepovers, school trips and family holidays. Research shows that children with NMNE experience greater distress and have lower self-esteem than children with MNE.
A Swedish study compared self-esteem between children who wet their beds and those who didn’t, and found that bed wetting had a significant impact on self-esteem. Another study examining the psychological impact of bed wetting found that primary school aged children ranked it as the third most distressing out of a series of 11 critical life events. Divorce and strident parental fighting were the only two events that ranked as more distressing to this group of children. Bed wetting was more distressing than being teased frequently, which ranked fourth.
Where a person wets the bed as an adult, the impact is much greater and can affect one’s career, personal relationship and social life. A Hong Kong study looked at bed wetting in a large group of adults, and found that rates of depression, low self-esteem and sleep disturbance were much higher in the bed wetting group. Furthermore, those with MNE were less likely to reach university education level.
The impact of bed wetting on the parents of the child is also significant. Research has shown that the greatest concern of parents of children who wet their beds is the impact on their child’s emotional and social development. Parents of younger children understood that the child could not control the wetting episodes. However, parents of older children thought that the child had control over the episodes and this impacted negatively on their relationship with the child. In some circumstances, parents resorted to punishing the child, particularly in migrant populations.
Bed wetting also creates an additional workload for parents in the form of washing and drying bed linen, and this is associated with significant financial costs. One study estimated the financial burden associated with a child who wets their bed to be $1,000 USD per year.
 |
For more information about how bed wetting can impact on the psychological wellbeing of an individual, and how these impacts can be minimised, see Impact of Bed Wetting. |
Statistics

An Australian study looked at bed wetting in children aged 5–12 years and found that 18.9% of these children wet their beds. Of this group, 15% wet at night with no daytime symptoms, and 4% wet at night and during the day. Bed wetting was more common in males, who made up 60% of the bed wetters in this study. Most of these children wet their bed less than once a month.
A study conducted in Hong Kong showed that bed wetting persisting into adulthood affected 1.9% of adults. Of these adults, 53% wet the bed more than 3 nights per week and 26% wet the bed every night.
A British study found that the percentage of children who wet their bed declined from 30% at 54 months to 9.5% at 115 months. Bed wetting was most pronounced between 54 and 65 months of age. In this large study, 68.5% of bed wetters had MNE versus 31.5% who had NMNE.
Risk factors
Bed wetting is likely to result from many different factors, including both genetic predisposition and environmental factors. Where daytime wetting is concerned, predisposing factors include a family history of daytime symptoms, infections of the urinary tract, neuropathic bladder, disorders of the urinary system, and psychiatric disorders.
Family history
Research has shown that children with parents who wet the bed are more likely to be bed wetters themselves. In families where both parents were bed wetters as children, their own child has a 77% risk of wetting the bed. Where only one parent wet the bed, the risk is 43%, and where no parents wet the bed, the risk is 15%.
A family history of bed wetting is also strongly associated with the age at which the child will become dry. Children who have two first-degree relatives who wet the bed became dry 1.5 years later than those children with no family history of bed wetting.
Genes
Bed wetting has been linked to several genetic defects, although the relationship between these defects and bed wetting is poorly understood. Recently a gene known as ENUR1 has been identified as having a possible link to bed wetting, although more research is required for the link between the gene and bed wetting to be better understood.
Obstructive sleep apnoea
A close relationship exists between bed wetting and obstructive sleep apnoea (OSA). It is thought that OSA results in altered pressures within the ribcage while sleeping, and that this affects the production of a hormone known as atrial natriuretic peptide. This hormone plays a role in increasing the amount of water and salt that the kidneys excrete through urine. Studies examining the relationship between OSA and bed wetting have yielded inconsistent results to date.
Progression
Research has shown that the rate of bed wetting reduces with time. One Chinese study found that the rate reduced from 16.1% in 5-year-olds to 10.1% in 7-year-olds and 2.2% in 19-year-olds. Those with severe bed wetting are less likely to become dry, with only 60% of severe bed wetters achieving dryness before adulthood. This same study suggested that bed wetting that persists into adulthood is usually severe, with 43.9% of 19-year-old bed wetters wetting the bed 7 nights per week.
Children who wet their bed are more likely to develop bladder problems, including incontinence, as adults.
Symptoms
What causes bed wetting?

- Difficulty rousing from deep sleep (arousal difficulties);
- Producing too much urine at night (nocturnal polyuria); and
- Overactivity of the detrusor muscle, which makes up part of the bladder wall.
 |
For more information about the causes of bed wetting view the video: Causes of Bedwetting. |
Impaired arousal
Difficulty waking from deep sleep is thought to be one of the key factors involved in bed wetting. Children who wet their beds are often described by their parents as being very deep sleepers who are difficult to rouse. New research has identified an area of the brain, known as the locus ceruleus, which is responsible for arousal from sleep. It is closely related to the part of the brain that controls bladder function, and may be disturbed in children who wet their beds.
 |
For more information about how the bladder and the brain communicate and what goes wrong when children have difficulty rousing view the video: Causes of bedwetting- difficulty rousing from sleep. |
Nocturnal polyuria (overproduction of urine at night)
Over-production of urine at night is thought to be the result of reduced levels of a hormone known as anti-diuretic hormone (ADH), which is released from the pituitary gland in the brain. ADH works to reduce the amount of urine produced by the kidneys. Under normal circumstances, the level of this hormone produced is significantly greater at night, thus limiting the production of urine overnight. Children who wet their bed do not demonstrate this increase in ADH levels, resulting in large quantities of urine being produced over night. These children typically have bladders which fill in the first third of the night, and as a result tend to flood the bed during the early parts of the night and don’t usually wet the bed again that night. Children with this pattern of bed wetting are more likely to respond to desmopressin, which is a form of ADH found in certain medications used to treat bed wetting.
 |
For more information about overproduction of urine view the video: Causes of bedwetting- overproduction of urine. |
Detrusor muscle overactivity (overactive or twitchy bladder)
The third factor thought to contribute to bed wetting is that of an overactive detrusor muscle. Children with this disorder usually pass small amounts of urine and void more frequently. This is often associated with an urgent desire to pass urine, and incontinence associated with not reaching the toilet in time. Bed wetting occurs when an abnormally small bladder fills up or contracts suddenly at night, resulting in a very variable wetting pattern and often several bed wetting episodes per night.
 |
Learn how an overactive bladder can cause children to wet the bed by viewing the video: Causes of Bedwetting: Overactive or Twitchy Bladder. |
Seeing your health practitioner for the first time
The first point of contact with your health practitioner will focus on obtaining some information about your child’s medical history and their pattern of bed wetting. This is important for ruling out any underlying medical problems that may be contributing to your child’s bed wetting and establishing the best way to manage the bed wetting.
Some topics that your health practitioner may wish to discuss include:
- How long the bed wetting has been a problem for;
- The pattern of bed wetting (i.e. how many nights a week, how many times a night, whether or not your child has daytime wetting or other bladder symptoms);
- Factors that may contribute to bed wetting, including constipation, diabetes, learning difficulties or behavioural problems; and
- The impact that bed wetting is having on your child and family.
Clinical examination
Most children who wet their bed have a normal physical examination. Your health practitioner may wish to examine your child’s spine to exclude nervous system abnormalities, and their tummy to exclude constipation. Examination of the child’s rectum and genitals are not usually necessary and should only be performed if the child and family feel comfortable with this being done.
How is it diagnosed?
Urine sample

Urinary tract ultrasound
As a general rule, an ultrasound of the urinary system is not required in children with straightforward bed wetting. Children thought to have NMNE or an underlying abnormality of the urinary system may require an ultrasound. This can detect if there is any obstruction to the flow of urine, reflux of urine from the bladder back up to the kidneys, or thickening of the bladder wall.
Bed wetting diary
Another useful tool that your health practitioner might discuss is a diary to record how much your child drinks, how often your child uses the toilet, how often they wet and how much urine they pass each time they use the toilet. Ideally the diary should be kept for a period of 1 week.
Other investigations
Other tests that may be requested by your health practitioner include an x-ray of the tummy or the spine, and special tests that measure urine flow and volume before and after using the toilet. These tests are usually only required in complicated cases of bed wetting or where your health practitioner suspects that there may be an underlying medical problem contributing to your child’s bed wetting.
Prognosis
Studies of children who wet their bed over time have shown that the rate of bed wetting reduces with age. Even in children who receive no treatment, 14% will overcome their bed wetting each year. Research shows that treatment in the form of a bed wetting alarm or medication is often successful. When used properly, a bed wetting alarm results in dryness in about two-thirds of children. Treatment with desmopressin results in complete dryness in 30% of children and partial dryness in 40% of children, with the average child wetting the bed 1.34 less nights per week. Relapse rates are higher with desmopressin therapy than alarm therapy, with 54% versus 35% of children wetting the bed after a period of dryness.
A Chinese study looking at 16,512 children and adolescents found that severe enuresis in childhood was associated with a poor prognosis and often persisted into adulthood. At 19 years of age, 48.3% of bed wetters had severe enuresis, which was described as wetting the bed 7 nights per week. Adolescent boys over the age of 10 years were more likely to have associated daytime wetting than younger boys. Bed wetting continuing into adulthood has a much greater impact and can affect career choice, personal relationships and social life.
Treatment

It is important to note that children who wet during the day in addition to wetting at night are less likely to respond to treatment. Treatment should first focus on addressing the daytime symptoms and excluding underlying medical problems. If your child wets during the day or has other medical problems that may be contributing to their bed wetting, your treating doctor may consider referring you to a specialist.
 |
View a video of Paediatrician Dr Mark Gibbeson discussing options for treating bedwetting in children. |
General advice
Your treating practitioner should discuss bed wetting with you and your child and the different treatment options that are available. It is important that the child is involved in this discussion and that both parties are motivated to make treatment work.
Your treating practitioner should also talk to you and your child about the importance of maintaining fluid intake, avoiding caffeinated drinks and eating a balanced diet to avoid constipation. Ensuring that the child is using a toilet at regular intervals throughout the day is important, and parents need to encourage this. Inadequate fluid intake or abnormal toileting patterns should be addressed before starting treatment and enuretic children should be encouraged to limit how much they drink bedtime and should use the toilet immediatly before they go to bed. Practical issues that should be considered before starting any treatment for bed wetting include making changes to sleeping arrangements if your child shares a bedroom or bed with another child, ensuring your child has easy access to the toilet during the night and also making sure your bedroom is close enough to your child’s to provide support during the night.
Waking or lifting your child out of bed at night to use the toilet can help overcome bed wetting in the short term, but won’t fix it in the long term.
If you wish to use a reward system, this shouldn’t be to reward dry nights as it places unnecessary pressure on the child. Rewards should instead be for drinking recommended levels of fluid during the day or using the toilet at regular intervals and before going to bed.
Children can be very sensitive to family problems and a stressful home enviroment may be a trigger for bed wetting. It is important that you address any family issues while you help your child manage their bed wetting.
Alarm therapy
The use of a bed wetting alarm should be considered in all children who wet their bed. Although poorly understood, the alarm is thought to work through heightening arousal and increasing the volume of urine that the bladder can hold at night. There are two types of alarm systems available in Australia which can be hired through local hospitals or community bed wetting services. The first system comprises a large pad which is placed in the bed and triggers a loud alarm when liquid comes into contact with it. The second system involves a personal alarm which is either clipped onto the child’s underpants or a pad placed inside the child’s underpants, with any liquid triggering the alarm.
Alarm therapy requires motivation on the part of the child and their parents and can take several weeks to be effective. When the alarm goes off, a parent needs to ensure that the child wakes, goes to the toilet to pass urine and then returns to bed and reattaches the alarm. This sequence needs to be followed every night for a period of 2–3 months. Consistency is the key. Once dryness is achieved, the alarm should be continued until 14 consecutive dry nights have been reached.
When used successfully, the alarm system results in dryness in about two-thirds of children. Two additional components, known as overlearning and dry night training, can help to reduce relapse rates. Overlearning requires that the child drinks a modest amount of extra water an hour before bed and repeats the same sequence as above. Dry bed training involves getting the child to go to the toilet repeatedly and changing their own sheets if they wet.Once the child has been dry for a month with overlearning, alarm therapy can be ceased.
If the child relapses after a successful course of alarm therapy, another course should be trialled. Alarm therapy requires time and motivation and is therefore not ideal where rapid success is required (for a school camp or family holiday) or in chaotic households.
 |
For more information about he use of a bed wetting alarm, how effective they are and when they should be used, see Alarm Therapy. |
Desmopressin
Desmopressin is available as a tablet, a melt that dissolves on the tongue, and a nasal spray. Desmopressin should ideally be taken 1 hour before sleep as this allows time for it to reach the kidneys. If successful, your doctor will discuss continuing desmopressin on a daily basis versus using it only for nights when it is important that your child remains dry, such as at school camps, sleepovers or family holidays. If your child continues desmopressin on a daily basis, it is important to discuss treatment duration with your doctor.
The main side effects associated with desmopressin are low salt levels in the blood, known as hyponatraemia. When the salt levels are very low, it can have adverse effects on the brain and result in seizures. To prevent salt levels becoming too low, you need to make sure that your child does not drink any liquid in the 2 hours before going to bed or during the night. If your child develops any signs of low salt levels, which can include headache, nausea or vomiting, you should seek medical attention promptly.
My dryness tracker app
 |
A free app for individuals being treated for bedwetting (nocturnal enuresis), or who plan to see a doctor about the condition. Features a bedwetting checklist, day-time and night-time voiding diaries, alarm therapy progress tracker, desmopressin progress tracker (restricted access), WetAlert® enuresis alarm ordering facility and treatment progress reports. Available from the App Store and Google play for use on smartphone and tablet. |
Anticholinergics
Anticholinergics are a group of drugs that work to relax the detrusor muscle of the bladder. This class of drugs is generally reserved for children who have not had success with either alarm or desmopressin therapy. The most commonly used agents in this class include oxybutynin (e.g. Ditropan), tolterodine (e.g. Detrusitol) and propiverine.
Expert opinion suggests that anticholinergics should be used in combination with desmopressin or TCAs in children who wet their bed. Research shows that when used alone, these drugs are not very successful. One study looked at 41 children who wet the bed, and found that the group who took anticholinergics in addition to desmopressin wet the bed 66% less. When anticholinergic medications were combined with a TCA, the number of wet nights was reduced from 6.1 to 1.7 per week.
Oxybutynin has been well researched in the setting of NMNE. An Italian study found that 50% of children were successfully treated with oxybutynin alone. In this same study, when oxybutynin was combined with desmopressin, the success rate was 71%.
Anticholinergic medication reaches its maximal effect after 2 months of use and is best taken at bed time. A study looking at side effects of this medication found that 76% of patients experienced side effects, which can include dry mouth, difficulty swallowing, dry eyes, blurred vision, diarrhoea, constipation and bloating. The most serious side effects are those that affect the brain and this can occur in up to 33% of children. These side effects include agitation, drowsiness, confusion, memory loss, nightmares and hallucinations.
Tricyclic antidepressants
Tricyclic antidepressants are a group of antidepressant medications that can be used to treat bed wetting. Due to their side effects, these drugs are usually reserved for children who have not had success with a bed wetting alarm, desmopressin or anticholinergics. Within this class of drugs, imipramine (e.g. Tofranil, Melipramine) is the one most commonly used for bed wetting.
Imipramine can have serious effects on the heart and, if taken in an overdose, can cause death. For this reason, your doctor will carefully examine your child for any heart problems and may ask whether or not there are any heart conditions that run in your family. Other common side effects include mood changes, nausea and difficulty sleeping.
If your doctor recommends this drug, it will generally be trialled for a period of 1 month. After this time, the dose may be adjusted depending on your child’s response. It is important that you see your doctor regularly to assess whether or not the drug is still required.
Other treatments
There is weak evidence from individual small studies to support the use of complementary interventions, including hypnosis, psychotherapy, acupuncture and chiropractic therapy. To date, there are no reliable studies that compare these treatments to the well-researched treatment methods mentioned above, which include alarm and desmopressin therapy.
Other simple measures, including reward systems and waking your child at night to use the toilet, have demonstrated some effect and can be trialled before using alarm or desmopressin therapy.
Bed wetting prevention
Limited knowledge about what causes bed wetting makes preventing the condition difficult. Bed wetting is a complex phenomenon resulting from the interaction of several factors, including underlying medical conditions, inherited genetic defects, and developmental and psychosocial factors. We also know that children who wet the bed are more likely to have impaired arousal from sleep, over-production of urine at night and an overactive bladder.
It is important that you and your child are aware that bed wetting is not a conscious act and that the child is not at fault. Punishing your child for wetting their bed is not appropriate and can make the problem worse.
 |
For more information about if and how bed wetting can be prevented, see Preventing Bed Wetting. |
References
- Nevéus T, von Gontard A, Hoebeke P, et al. The standardization of terminology of lower urinary tract function in children and adolescents: Report from the Standardisation Committee of the International Children’s Continence Society. J Urol. 2006;176(1):314-24. [Abstract | Full text]
- Bottomley G. Treating nocturnal enuresis in children in primary care. Practitioner. 2011;255(1741):23-6. [Abstract]
- Brown ML, Pope AW, Brown EJ. Treatment of primary nocturnal enuresis in children: A review. Child Care Health Dev. 2011;37(2):153-60. [Abstract]
- Fillingham S, Douglas J. Urological Nursing (3rd edition). Edinburgh: Baillière Tindall; 2004. [Book]
- Fowler CJ, Griffiths D, de Groat WC. The neural control of micturition. Nat Rev Neurosci. 2008;9(6):453-66. [Abstract | Full text]
- Blok B. Central pathways controlling micturition and urinary continence. Urology. 2002;59(5 Suppl 1):13-7. [Abstract]
- Schulpen TW. The burden of nocturnal enuresis. Acta Paediatr. 1997;86(9):981-4. [Abstract]
- Nørgaard JP, Djurhuus JC, Watanabe H, et al. Experience and current status of research into the pathophysiology of nocturnal enuresis. Br J Urol. 1997;79(6):825-35. [Abstract | Full text]
- Kuehhas FE, Djakovic N, Hohenfellner M. Infantile enuresis: Current state-of-the-art therapy and future trends. Rev Urol. 2011;13(1):1-5. [Abstract | Full text]
- Hägglöf B, Andrén O, Bergström E, et al. Self-esteem before and after treatment in children with nocturnal enuresis and urinary incontinence. Scand J Urol Nephrol Suppl. 1997;183:79-82. [Abstract]
- Van Tijen NM, Messer AP, Namdar Z. Perceived stress of nocturnal enuresis in childhood. Br J Urol. 1998;81(Suppl 3):98-9. [Full text]
- Yeung CK, Sihoe JD, Sit FK, et al. Characteristics of primary nocturnal enuresis in adults: An epidemiological study. BJU Int. 2004;93(3):341-5. [Abstract | Full text]
- Caldwell PH, Edgar D, Hodson E, Craig JC. Bedwetting and toileting problems in children. Med J Aust. 2005;182(4):190-5. [Abstract | Full text]
- Bower WF, Moore KH, Shepherd RB, Adams RD. The epidemiology of childhood enuresis in Australia. Br J Urol. 1996;78(4):602-6. [Abstract]
- Fonseca EG, Bordallo AP, Garcia PK, et al. Lower urinary tract symptoms in enuretic and nonenuretic children. J Urol. 2009;182(4 Suppl):1978-83. [Abstract]
- Butler RJ, Heron J. The prevalence of infrequent bedwetting and nocturnal enuresis in childhood: A large British cohort. Scand J Urol Nephrol. 2008;42(3):257-64. [Abstract]
- Su MS, Li AM, So HK, et al. Nocturnal enuresis in children: Prevalence, correlates, and relationship with obstructive sleep apnea. J Pediatr. 2011;159(2):238-42. [Abstract]
- Yeung CK, Sreedhar B, Sihoe JD, et al. Differences in characteristics of nocturnal enuresis between children and adolescents: A critical appraisal from a large epidemiological study. BJU Int. 2006;97(5):1069-73. [Abstract | Full text]
- Nevéus T. Nocturnal enuresis: Theoretic background and practical guidelines. Pediatr Nephrol. 2011;26(8):1207-14. [Abstract | Full text]
- Rittig S, Knudsen UB, Nørgaard JP, et al. Abnormal diurnal rhythm of plasma vasopressin and urinary output in patients with enuresis. Am J Physiol. 1989;256(4 Pt 2):F664-71. [Abstract]
- Yeung CK, Chiu HN, Sit FK. Bladder dysfunction in children with refractory monosymptomatic primary nocturnal enuresis. J Urol. 1999;162(3 Pt 2):1049-54. [Abstract]
- Neveus T, Eggert P, Evans J, et al. Evaluation of and treatment for monosymptomatic enuresis: A standardization document from the International Children’s Continence Society. J Urol. 2010;183(2):441-7. [Abstract | Full text]
- NICE clinical guideline 111: Nocturnal enuresis: The management of bed wetting in children and young people [online]. London: National Institute for Health and Clinical Excellence; October 2010 [cited 15 November 2011]. Available from: URL link
- Nunes VD, O’Flynn N, Evans J, et al. Management of bedwetting in children and young people: Summary of NICE guidance. BMJ. 2010;(341):936-9. [Abstract]
- Robson WL. Evaluation and management of enuresis. N Engl J Med. 2009;360(14):1429-36. [Abstract]
- Elsayed ER, Abdalla MM, Eladl M, et al. Predictors of severity and treatment response in children with monosymptomatic nocturnal enuresis receiving behavioral therapy. J Pediatr Urol. 2011. [Abstract]
- Glazener CM, Evans JH, Peto RE. Alarm interventions for nocturnal enuresis in children. Cochrane Database Syst Rev. 2009:CD002911. [Abstract | Full text]
- Glazener CM, Evans JH. Desmopressin for nocturnal enuresis in children. Cochrane Database Syst Rev. 2009:CD002112. [Abstract | Full text]
- Fergusson DM, Horwood LJ, Shannon FT. Factors related to the age of attainment of nocturnal bladder control: An 8-year longitudinal study. Pediatrics. 1986;78(5):884-90. [Abstract]
- Hjälmås K. Pathophysiology and impact of nocturnal enuresis. Acta Paediatr. 1997;86(9):919-22. [Abstract]
- Friman PC. A preventive context for enuresis. Pediatr Clin North Am. 1986;33(4):871-86. [Abstract]
- Glazener CM, Evans JH. Simple behavioural and physical interventions for nocturnal enuresis in children. Cochrane Database Syst Rev. 2009:CD003637. [Abstract | Full text]
- Van de Walle J, Van Herzeele C, Raes A. Is there still a role for desmopressin in children with primary monosymptomatic nocturnal enuresis?: A focus on safety issues. Drug Saf. 2010;33(4):261-71. [Abstract]
- Marieb EN, Hoehn KN. Anatomy and Physiology (3rd edition). San Francisco: Pearson Benjamin Cummings; 2008. [Book]
- Kwak KW, Lee YS, Park KH, Baek M. Efficacy of desmopressin and enuresis alarm as first and second line treatment for primary monosymptomatic nocturnal enuresis: Prospective randomized crossover study. J Urol. 2010;184(6):2521-6. [Abstract]
- Alloussi SH, Mürtz G, Lang C, et al. Desmopressin treatment regimens in monosymptomatic and nonmonosymptomatic enuresis: A review from a clinical perspective. J Pediatr Urol. 2011;7(1):10-20. [Abstract | Full text]
- Friedman BC, Friedman B, Goldman RD. Oxybutynin for treatment of nocturnal enuresis in children. Can Fam Physician. 2011;57(5):559-61. [Abstract | Full text]
- Austin PF, Ferguson G, Yan Y, et al. Combination therapy with desmopressin and an anticholinergic medication for nonresponders to desmopressin for monosymptomatic nocturnal enuresis: A randomized, double-blind, placebo-controlled trial. Pediatrics. 2008;122(5):1027-32. [Abstract | Full text]
- Caione P, Arena F, Biraghi M, et al. Nocturnal enuresis and daytime wetting: A multicentric trial with oxybutynin and desmopressin. Eur Urol. 1997;31(4):459-63. [Abstract]
- Glazener CM, Evans JH, Cheuk DK. Complementary and miscellaneous interventions for nocturnal enuresis in children. Cochrane Database Syst Rev. 2009:CD005230. [Abstract | Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







