- Introduction to allergy and the immune system
- Innate immune responses and allergy
- Hyper-responsiveness of the innate immune system and allergy
- Sensitisation: Development of abnormal adaptive immune response and allergy
- Perpetuation of abnormal allergic resonse
- Allergy, immunity and heredity
- Common allergens
- Allergic diseases
- Some helpful terms
Introduction to allergy and the immune system

Both the innate and adaptive immune systems play a role in allergy, which occurs as a result of sensitisation to harmless substances in the environmental (e.g. dust and pollen), and hypersensitive reactions upon subsequent exposure to these particles. The innate (also called non-specific) immune system acts in response to all foreign particles entering the body and involves:
- Epithelial barriers (skin and mucous membranes which line the bodies cavities including the nose, mouth and bowel);
- Body encasements such as the scull and thoracic cage which protect the internal organs from exposure to pathogens;
- Inflammatory responses involving proteins produced by body cells which mount an attack on pathogens which enter the body.
The adaptive (also called humoral or specific) immune system is typically only involved in immune responses to bacteria, bacterial toxins and virus antigens. It involves the production of antibodies (also called immunoglobulins) against a specific target. The target of an antibody is called an antigen. The antibodies circulate in the blood and react with their specific antigens, for example an antibody produced to mount an attack on the bacteria salmonella, will only attack salmonella and not other types of bacteria.
For the most part, the immune system protects the body from bacteria and foreign particles and are well controlled and directed against harmful pathogens. The immune response usually results in the pathogen being cleared from the body and subsequent resolution of the inflammatory processes which are involved in the immune reaction. However, in some individuals the innate immune system responds abnormally and mounts a response to particles in the environment which would not normally stimulate a response. This abnormal immune response causes allergy.
Innate immune responses and allergy
The innate immune system regulates the body’s initial response to pathogen exposure and is responsible for catalysing the sensitisation process which leads to allergic reactions. This is a non-specific response which involves recognition of molecules entering the body that are shared by a group of pathogens. The immune system recognises these molecules because they are not found in the cells of the human body. This type of immune reaction is distinct from the reactions which occur in recognition of specific pathogens such as salmonella.
Innate immunity is developed in the human body at birth and does not adapt or improve with ageing, unlike acquired immunity which develops throughout life as a result of pathogen exposure. For example, the skin and mucosa are tough, intact anatomical barriers which provide innate immunity and are in place at birth, as are mechanisms for mechanical removal of pathogens (e.g. sneezing and coughing, vomiting, mucus removal). On the other hand, antibodies to pathogens like salmonella only develop upon exposure to those pathogens, for example when an individual eats food contaminated with salmonella.
While anatomical barriers of the innate immune system can be seen with the naked eye, the innate immune system also functions at the cellular and molecular level. Important cells and molecules involved in innate immune responses include:
- Phagocytic cells which are white blood cells and include neutrophils, eosinophils and macrophages. These cells are attracted to foreign pathogens in the body by inflammation and remove harmful pathogens in the blood by ingesting them;
- Inflammatory mediators including basophils and mast cells. These cells regulate the body’s inflammatory responses and signal the body to mount an inflammatory response if a foreign particle invades. The inflammatory response catalyses other immune responses, such as activation of phagocytic cells;
- Natural killer cells which are also involved in adaptive immune processes. In the innate immune system these cells recognise cells under stress or invasion from pathogens and binds to them. The natural killer cells are capable of inducing apoptosis (death, or the last phase of the cell cycle) in the stressed cells and the pathogens they contain; and
- Molecules including complement proteins and cytokines. Molecules are produced by the cells of the human body but also influence responses of the immune system. For example, cytokines are pro-inflammatory, meaning that they stimulate inflammatory processes.
Hyper-responsiveness of the innate immune system and allergy
There are some circumstances where an exaggerated adaptive immune response is mounted against an otherwise harmless molecule. The harmless molecule is ignored by the innate immune system in the majority of people, but in some leads to an exaggerated response which causes tissue damage in the person’s body and in rare cases death. When these exaggerated and inappropriate immune reactions involve allergens such as dust and pollen they are termed allergic reaction or type 1 hypersensitivity reaction.
Sensitisation: Development of abnormal adaptive immune response and allergy
Allergic responses occur following sensitisation; that is, development of adaptive immunity (antibodies) to a particle (e.g. dust, pollen) which would not normally cause an immune response. Sensitisation occurs when an individual is exposed to a specific particle for the first time, and the body mounts an inflammatory response. If the body mistakes a harmless particle for a harmful substance the initial response by the innate immune system causes the production of IgE antibodies by the acquire immune system. The IgE antibodies produced are specific to the antigen, for example if it is pollen from a sunflower; the IgE antibodies produced only attack particles of pollen from sunflowers.
The specific IgE antibodies then inhabit mast cells. Mast cells have a large role in both allergy and the immune system. Mast cells are partly responsible for linking the innate immune system (to do with inflammation) and the acquired immune system (which is very specific and tightly controlled by antibodies). Mast cells which have been inhabited by IgE antibodies cause allergy by perpetuating an increasingly sensitive allergic response upon future exposure to the specific antigen.
Perpetuation of abnormal allergic response
Following sensitisation, an allergic response regulated by the adaptive immune system occurs with each future exposure to the specific antigen. Allergic diseases are characterised by an allergic response that occurs within 15 minutes of exposure to a specific antigen. The response can be divided into early and late phases.
Early phase response
The early phase response is mediated by IgE antibodies. It usually recovers within 2-4 hours. Mast cells also have a large role in allergic reactions as IgE specific antibodies for antigens inhabit these cells following sensitisation. When an antigen enters rthe body on subsequent occasions it interacts with specific IgE antibodies on mast cells. This leads to mast cell degranulation (rupture) and the release of inflammatory mediators. When this interaction leads to allergic disease, the antigen is then called an allergen.
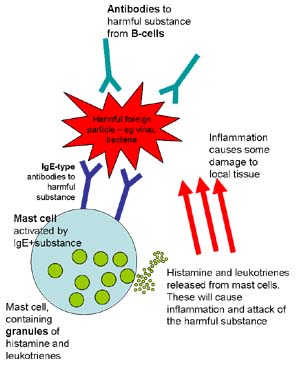
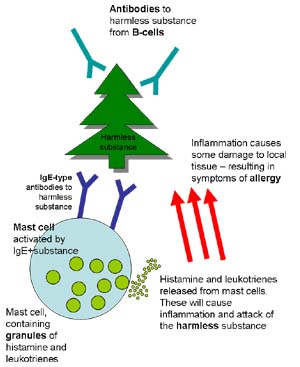
Late phase response
The late phase response occurs several hours later, usually starting 4 hours after contact with the allergen. It can last 12 to 24 hours in some individuals. This response occurs in response to inflammation, which catalyses the recruitment of phagocytic cells (white bloods cells including eosinophils and T lymphocytes) to the site of the allergy (e.g. the lungs in asthma). The white blood cells release inflammatory mediators, including mast cells, that lead to continued allergic symptoms. For example, mast cells produce cytokines which stimulate further IgE antibody production by B cells (cells that function to produce a wide range of antibodies).
Secondary immune response
IgE production by B cells during the late phase of allergic reactions causes a secondary immune response. Exposure to an allergen and the associated inflammatory response have a threshold-lowering effect in relation to future exposure; meaning that affected individuals become more sensitive to the allergen with increasing exposure.
Systemic immune response
The pathophysiological response which characterises allergic reactions also causes inflammatory mediators to circulate throughout the body (not only at the site of the allergic reaction). These inflammatory mediators may infiltrate tissues at other sites and cause comorbid allergic disease. For example, individuals with asthma often also experience allergic rhinitis.
Allergy, immunity and heredity
The tendency to develop allergic reactions has a strong hereditary factor. This tendency is termed atopy. Atopy is diagnosed in individuals who develop an allergic reaction to an allergen in a skin prick test (when the skin is pricked and exposed to the allergen). But not all individuals who develop allergic reactions to skin prick are affected by allergy to particles in the environment. Approximately 20–30% of the population is atopic, and two-thirds of atopic individuals have allergic disease.
It is still unknown why some people have this abnormal reaction to harmless substances in the environment, or why certain substances are more likely to cause allergies than others.
Common allergens
Some common allergens include:
- Pollens such as grass pollens;
- House dust mites;
- Animal dander such as cat, dog and horse;
- Moulds.
Allergic diseases
Important allergic diseases include allergic allergic asthma, allergic eczema, allergic rhinitis and conjunctivitis, food allergies and anaphylaxis.3 Diagnosis of these conditions is made on the basis of clinical history and examination in conjunction with skin-prick testing or measurement of IgE in a blood test
Some helpful terms
These are some of the terms you may hear when doctors discuss allergies:
- Allergen: An allergen is a name for any substance that causes an allergic reaction.
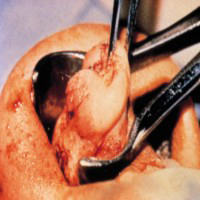
- Allergic rhinitis: This is group of symptoms of nose and upper airways caused by allergy, commonly including a runny nose, cough and an itchy sensation, also known as hay fever. Below is an image of polyps being removed from the nose, in a surgical operation. Polyps can form in some people who suffer from allergic rhinitis.
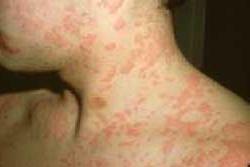
- Allergy: An allergy is an exaggerated immune reaction to substances that are normally harmless. Allergy can appear in many forms and cause many symptoms, such as sneezing, respiratory symptoms such as asthma or hay fever, itching, skin rashes, or generalised reaction such as anaphylaxis. Below is an image of a skin rash reaction to an food allergen.
- Anaphylaxis: Anaphylaxis is a dangerous generalised allergic reaction to an allergen.
- Antibody: Antibodies are proteins (also known as immunoglobulins) that are produced by B-cells after these cells have been stimulated by an antigen. Antibodies act specifically against that antigen in immune responses, which may be normal (such as fighting infection) or abnormal (such as allergy).
- Antigen: An antigen is a substance foreign to the body that causes an immune response.
- Asthma: Asthma is an inflammatory lung condition characterised by short periods of ‘bronchoconstriction’, or tightening of the airways, making it more difficult to breathe. This condition is often caused by allergy, or may be worsened by allergy.
- Asymptomatic: A word used to describe someone who has no symptoms.
- Atopy: People who are ‘atopic’ have a reaction to allergens on skin-prick tests or RAST, but they may or may not have symptoms of allergic disease.
- B-cell: A B-cell (sometimes called a B-lymphocyte) is a type of white blood cell that produces antibodies against foreign antigens.
- Desensitisation: A treatment of allergy where a person is exposed to small amounts of an allergen until they no longer produce an allergic reaction to the substance.
- Eczema: Eczema is an inflammatory skin condition characterised by redness, itching and oozing lesions that can become scaly, crusted or hardened, that is often caused by allergy.
- Eosinophil: An eosinophil is a type of white blood cell that is often elevated in people with allergic disease. Its name comes from a kind of dye called ‘eosin’ that can be used to show it up from the background when using a microscope.
- Histamine: Histamine is a local-acting hormone, only active for a short time, that is released by mast cells. Histamine causes many of the symptoms of allergy.
- Hypersensitivity: This term is used to describe exaggerated, inappropriate immune responses to usually harmless substances. This term may be used instead of ‘allergy’.
- IgE: A class of antibody (or immunoglobulin), that function especially in allergy. The other antibody classes are IgA, IgD, IgG and IgM.
- Leukotrienes: Leukotrienes are a group of fast-acting, short-range hormones that are released by mast cells. Leukotrienes cause many of the symptoms of allergy.
- Mast cell: A mast cell is a type of white blood cell involved in allergic reactions by releasing mediators such as histamine and leukotrienes in allergic reactions, and by being sensitive to the presence of IgE.
- Mediators: This term is almost interchangeable with hormone, but often means chemicals produced by cells of the body that have particular roles in communicating or controlling neighbouring cells, some of which are involved in allergic disease. Examples include leukotrienes and histamine.
- Perennial: A term meaning ‘occurring all year round’. Originally used to refer to plants that grow all year round, this is now commonly used in allergy, since many allergens are from plants – such as pollen.
- RAST: RadioAllergoSorbent Test (or RAST), often used to determine what antigens a patient is allergic to.
- T-cell: A T-cell (sometimes called a T-lymphocyte) a type of white blood cell involved in immune responses and often involved in allergic reactions.
- Seasonal: This word simply means ‘occurring at a particular time of the year’.
References
- Kaiser GE. The innate immune system. Doc Kaiser’s Microbiology Home Page. Community College Baltimore County. 2007. [cited 31 January 2012] Available from: [URL Link]
- Kaiser GE. Humoral immunity. Doc Kaiser’s Microbiology Home Page. Community College Baltimore County. 2007. [cited 31 January 2012] Available from: [URL Link]
- Kumar, P. Clark, M. Clinical Medicine. 5th ed. 2002. W. B. Saunders. Edinburgh.
- Marieb EN, Essential of Human Anatomy and Physiology. (7th edition). San Francisco: Benjamin Cummings; 2003.
- Baroody FM, Naclerio RM. World Allergy Org J. 2011; 4(1): S1-5. [Full Text]
- Peakman, M. Vergani, D. Basic and Clinical Immunology. 1997. Churchill Livingstone. New York.
- Ghaffar A, Hypersensitivity reactions. Chapter 17. Microbiology and immunology. [online]. University of South Carolina. 2010. [cited 26 January 2012]. Available from: [URL Link]
- Orahilly R, Muller F, Carpenter S, Swenson R. The nose and paranasal sinuses. Chapter 52. Basic Human Anatomy. R Swenson, Ed. Dartmouth Medical School. 2008. [cited 31 January 2012]. Available from: [URL Link]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.