- What is Perennial Allergic Rhinitis
- Statistics on Perennial Allergic Rhinitis
- Risk Factors for Perennial Allergic Rhinitis
- Progression of Perennial Allergic Rhinitis
- Symptoms of Perennial Allergic Rhinitis
- Clinical Examination of Perennial Allergic Rhinitis
- How is Perennial Allergic Rhinitis Diagnosed?
- Prognosis of Perennial Allergic Rhinitis
- How is Perennial Allergic Rhinitis Treated?
- Perennial Allergic Rhinitis References
What is Perennial Allergic Rhinitis
Allergic rhinitis is an allergic disease which affects many people worldwide. Rhinitis means ‘inflammation of the nose’, whilst the term allergic describes ‘a normal but exaggerated response to a substance’. It may be perennial, which means symptoms are present throughout the year, or seasonal, with symptoms peaking during the months of spring and summer when pollen levels are at their highest.
Perennial rhinitis is characterised primarily by nasal symptoms including watering or congestion of the nose and sneezing. It occurs due to an exaggerated response to an environmental trigger which results in inflammation of the lining of the nose. It is similar to hayfever, however, the substances which cause the allergic reaction are present all year round.
Common causes include the faecal matter of the house dust-mite, animal proteins from domestic pets, and industrial dusts and fumes.
Statistics on Perennial Allergic Rhinitis
The prevalence of perennial allergic rhinitis varies worldwide. Many people do not seek treatment and the exact figures for perennial rhinitis are often under-reported, although it is universally acknowledged that it is an extremely common condition.
The 2004-05 National Health Survey stated that 3.2 million Australians (approximately 16.1% of the population) self-reported experiencing symptoms of hay-fever and perennial rhinitis. The prevalence was found to be highest amongst those aged 25-34 and was slightly higher among females (1.7 million) than males (1.5 million).
Number of people with allergic rhinitis (by age)
| Age | 0-14 | 15-24 | 25-34 | 35-44 | 45-54 | 55-64 | 65-74 | >74 | Male | Female | Total |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Prevalence (thousands) |
303.4 | 521.8 | 618.6 | 601.7 | 528.6 | 315.1 | 158.2 | 118.3 | 1463.5 | 1702.2 | 3165.7 |
Percentage of the population with allergic rhinitis (by state)
| State | NSW | Vic | Qld | SA | WA | Tas | ACT | Aust |
|---|---|---|---|---|---|---|---|---|
| % Population | 13.8 | 18.2 | 14.1 | 20.9 | 18.8 | 14.7 | 21.6 | 16.1 |
Risk Factors for Perennial Allergic Rhinitis
Atopy
Atopy describes a syndrome of over-active immune responses, in which individuals are more likely to develop allergy-related diseases including allergic rhinitis, asthma, and eczema. These individuals have higher levels of IgE antibody in their blood which is responsible for the inflammatory response seen in allergies.
Predisposing factors to atopy include:
- Genetics: Atopy is inherited as an autosomal dominant condition.
- Maternal and neonatal factors: Such as smoking in pregnancy and early childhood, low birth weight, birth during the pollen season (though this is still being debated), early introduction of formula and food.
There is much research underway into other factors which may predispose to atopy in childhood, including early exposure to allergens in the environment, and maternal and early childhood diet. Exposure to allergens is the second component of allergic rhinitis.
Perennial allergic rhinitis is caused by house-dust mite faeces, domestic pets (saliva or skin proteins), industrial dust, vapours and fumes. In those with perennial rhinitis, cigarette smoke, washing powders, detergents, strong perfume, and traffic fumes may exacerbate the condition.
Progression of Perennial Allergic Rhinitis
Some people are predisposed to have an exaggerated response to a substance that is usually tolerated by the body. When these substances promote an allergic reaction they are known as allergens. In susceptible individuals, allergens initiate an immune response which is controlled by immune cells in the body (such as mast cells). The allergen binds to a protein called IgE on the surface of mast cells, causing them to release potent inflammatory agents such as histamine.
In the case of allergic rhinitis, the early response to allergens results in a runny nose, itching, and sneezing. The late response is similar, however the nose is usually more congested.
Perennial allergic rhinitis results in symptoms all year round, as the allergens causing the disease (dust-mite, pets) are always present in the environment.
Nasal polyps occur in some people with perennial rhinitis; they are smooth, round, soft structures attached to the lining of the nose. They can cause obstruction of the nose, and loss of smell. Occasionally they need to be surgically removed due to extreme discomfort.
Over time, people with perennial rhinitis may experience a reduced sense of smell, headaches, and recurrent infections. Other potential complications include infections of the middle ear and sinuses.
Symptoms of Perennial Allergic Rhinitis
When diagnosing perennial allergic rhinitis, the doctor asks a number of questions relating to the onset, duration and character of the symptoms. This can help identify substances that trigger the allergic response and confirm a diagnosis of rhinitis. The presence of risk factors, including a history of asthma or other allergic diseases, would also support this diagnosis.
Unlike in seasonal rhinitis, the symptoms of perennial allergic rhinitis will usually be present throughout the entire year. Symptoms are usually confined to the nose: sneezing, watery or runny nose, nasal blockage, decreased sense of smell. Perennial rhinitis may be complicated by sinusitis, resulting in facial pain and localized headaches.
Clinical Examination of Perennial Allergic Rhinitis
Initial observation may reveal a dull, nasal voice resulting from blockage of the nose. The eyes may be red and watery, and dark circles may be evident below the eyes due to congestion of the nasal veins. A horizontal crease may be noticeable on the outside of the nose, particularly in children, as a result of frequent wiping.
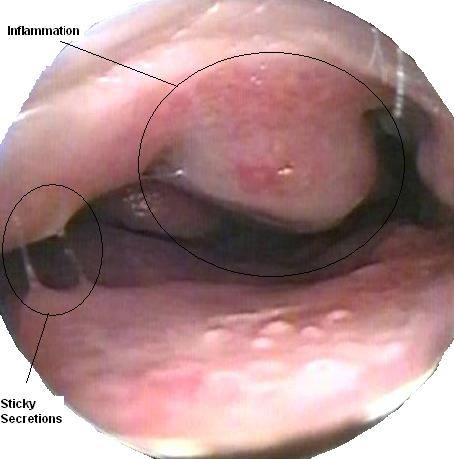
The nose is examined using a nasal speculum or an otoscope with an attachment for the nose. This allows the inside of the nose to be viewed directly. In people with allergic rhinitis the lining of the nose is usually pale and swollen, however there may be areas of redness, which may be due to infection or rhinitis medicamentosa‘ (inflammation of the nose caused by intrasnasal medications).
Secretions are usually thin, watery and colourless. Thicker mucous which is yellow or green may indicate an infection.
The nasal septum which separates the two sides of the nose should also be examined to look for any deviation or perforation. The doctor will also look for evidence of any masses, such as nasal polyps, which may restrict the flow of air through the nose and cause breathing difficulties.
The ears and throat should be examined to look for signs of inflammation or infection such as redness or pus. The GP may press gently on your forehead and cheeks. If this is painful there may be an infection of the underlying sinuses.
Examination of the neck should also be performed to feel for enlarged lymph nodes which may indicate an infection or tumour. It is also important to listen to the lungs as there is a strong relationship between allergic rhinitis and asthma.
How is Perennial Allergic Rhinitis Diagnosed?
Skin prick tests are used to confirm if a patient is allergic to a substance. Small quantities of various allergens are injected under the skin of the forearm to see if they evoke an allergic response. A positive test will show a ‘wheal and flare’ response which includes redness, swelling and itching.
Radio Allergo Sorbent Testing (RAST testing) is similar to a skin prick test. However, it is more expensive and so is only used if the skin prick test is not suitable (eg. where there is a high risk of anaphylaxis) or unavailable. Various allergens are exposed to a blood sample taken from a patient and the levels of IgE produced are measured.
Prognosis of Perennial Allergic Rhinitis
Perennial allergic rhinitis is a benign condition and can be well-managed with appropriate treatment. Nevertheless, it can be a frustrating disease to live with. Atopic patients are also more likely to develop a serious allergy to other substances (eg. peanuts and other food allergies) and thus may be at risk of anaphylactic reactions which are associated with significant mortality.
There is also a strong relationship between allergic rhinitis and asthma; patients with allergic rhinitis are three times more likely to develop asthma and effective treatment of allergic rhinitis has beneficial effects on asthma.
How is Perennial Allergic Rhinitis Treated?
The management of perennial rhinitis involves the avoidance of triggers such as house dust-mite faeces and animal proteins, in conjunction with pharmacological treatments.
Allergen avoidance
Mattresses and pillows may be encased in protective covers which are impermeable to dust mites, and bedding should be washed regularly. Air filters and regular cleaning of carpets, furniture and pets can help in reducing animal allergens, however optimal results can only be achieved through removal of the animal from the household.
Corticosteroids
E.g. Budesonide (Rhinocort), Mometasone furoate (Nasonex). Corticosteroids in the form of a nasal spray are the first-line treatment for perennial allergic rhinitis. Steroids reduce the inflammatory response caused by the allergic reaction, thereby helping to reduce the nasal symptoms such as itching and either congestion or watering of the nose. Intranasal corticosteroids are cheaper than antihistamines and provide better relief of nasal symptoms. The two can be used together for optimal symptom control.
The side effects of this treatment are minimal as the dose is small and acts locally on the lining of the nose. Oral corticosteroids, such as prednisolone may be required if the nasal spray does not help and these are associated with significant side effects with long-term use.
Antihistamines
E.g. Cetirizine hydrochloride (Zyrtec), Fexofenadine hydrochloride (Telfast). These drugs work by blocking the effects of histamine which is one of the main substances driving allergic reactions. Histamine is responsible for the sneezing, and itchy, runny nose experienced in perennial allergic rhinitis. Antihistamines block this effect, relieving the symptoms.
Older anti-histamines may cause unwanted effects such as drowsiness, fatigue and decreased concentration, and may also cause constipation, impotence and difficulty urinating. Newer antihistamines have fewer side effects and provide effective relief of symptoms, particularly when used with intranasal corticosteroids.
Decongestants
E.g. Phenylephrine hydrochloride (Sudafed). Decongestants may be taken orally or as a nasal spray to reduce the secretions and swelling of the lining of the nose by constricting the blood vessels in the nose. Decongestants can cause ‘rhinitis medicamentosa’ (worsening of symptoms when the medication is stopped) hence they should only be used for a limited period of time to open the nasal passages to allow the administration of other therapy, such as corticosteroids.
Oral decongestants are not suitable for everyone, such as those with high blood pressure or heart disease, and they may cause anxiety, restlessness and insomnia.
Anti-inflammatories
E.g. Sodium cromoglycate (Rynacrom). These drugs also block the inflammatory pathways that cause the symptoms of perennial rhinitis, however, they have not been found to be more effective than corticosteroids or antihistamines.
Eye drops
E.g. Ketotifen fumarate (Zaditen), Hydrocortisone acetate (Hycor). Eye drops containing anti-histamine or steroids may be used to control symptoms such as itchy or watery eyes.
Allergen desensitisation
This involves exposing the patient to small doses of allergens in an attempt to desensitize them and prevent an allergic response. This procedure must be performed by qualified practitioners with immediate access to resuscitation equipment as it may be associated with severe reactions including anaphylaxis. Most of the drugs used in the treatment of perennial allergic rhinitis are available over the counter from the pharmacy, however some may require a prescription from your GP.
(Kindly reviewed by Associate Professor Frank Thien MD FRACP FCCP; Consultant Respiratory and Allergy Physician; Department of Medicine; Alfred and Box Hill Hospitals; Monash University Central and Eastern Clinical School; Editorial Advisory Board Member of the Virtual Allergy Centre and Virtual Respiratory Centre.)
Perennial Allergic Rhinitis References
- Australian Bureau of Statistics. National Health Survey 2004-05: Summary of Results. Australia; 2006
- Kumar P, Clark M. Clinical Medicine. Sixth Ed. Elsevier Saunders, 2005. pp220, 895-8.
- Cookson WOCM, Hopkins JM. Dominant inheritance of atopic immunoglobulin I responsiveness. Lancet 1988; 1: 86-8.
- Bellussi L, et al. Natural history of allergic rhinitis: a review. Clinical and Applied Immunology Reviews 2001: 207-16.
- Pawankar R. Allergic rhinitis and asthma: the link, the new ARIA classification and global approaches to treatment. Current Opinion in Allergy and Clinical Immunology 2004; 4(1): 1-4.
- Basger B, et al. Optimising the management of allergic rhinitis: an Australian perspective. MJA 2005; 182(1): 28-33.
- Puy R. Diagnosing and treating allergic rhinitis. Medicine Today 2003; 4(10): 14-21.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







