- What is amniocentesis
- Reasons for having amniocentesis
- What to expect during and after the investigation
- What do the results mean?
- Possible side effects/risks
What is amniocentesis
| The amnion, also known as the amniotic membrane or amniotic sac, is a sac which encloses the fetus (the unborn baby), rather like a balloon. This sac is filled with fluid which surrounds the fetus, it is known as amniotic fluid. This is shown in the diagram on the right. |
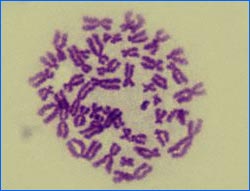
Amniocentesis is a procedure which involves draining a small amount of amniotic fluid. Amniotic fluid contains a few cells from the fetus. Chromosomes in the cells, which contain the genetic information of the fetus, are examined for abnormalities. This is done through karyotyping of the cells. The karyotype of the cell is a photograph of the cell’s chromosomes. The cells karyotype shows the number, size and shape of the chromosomes. An abnormal karyotype is an indication of genetic abnormalities. Thus, the main aim of amniocentesis is to diagnose genetic abnormalities in the fetus. An example of a karyotype is shown the figure below. Amniocentesis is usually performed between 15 and 17 weeks gestation (i.e. 16 weeks into the pregnancy). Amniocentesis is used to diagnose chromosomal abnormalities such as Down’s Syndrome and hereditary conditions such as muscular dystrophy. It is 99% accurate.
Reasons for having amniocentesis
You may consider amniocentesis for the following reasons:
- You, your partner or another family member has a hereditary condition that might be passed onto your children.
- You or your partner is a woman aged 35-37 years or older
- A prenatal screening test (ultrasound, first trimester screening or maternal serum screening) has indicated an increased risk for a birth defect and/or hereditary condition.
The choice of whether or not to have amniocentesis should be made by you and your partner in consultation with your Doctor.
What to expect during and after the investigation
- Amniocentesis is an outpatient procedure that takes 15-30 minutes to complete.
- First, the doctor uses ultrasound to find a suitable part of the amniotic sac to sample.
- The skin over the spot to be sampled is cleaned with antiseptic.
- A thin, hollow needle is inserted through the mother’s abdomen into the uterus and through the amniotic sac to obtain a sample of amniotic fluid.
- Amniotic fluid is withdrawn and placed into a suitable container for testing.
- The fluid is sent to the lab to undergo testing such as karyotyping.
- If you are Rhesus negative you will need an anti-D injection after the procedure.
- Results are usually available in 2-3 weeks.
You will be awake and aware during the procedure and should experience little or no pain. There may be some discomfort which has been described as a slight pressure or menstrual like cramp. Afterwards there may be tenderness where the needle was inserted. It is recommended that you rest for about 20 minutes after the procedure and take things easy for a few days. Bed rest, however, is not necessary.
What do the results mean?
- A negative result excludes the prescence of the condition which is being tested for. This does not guarantee the absence of a different birth defect and/or hereditary condition.
- A positive result confirms the prescence of the condition being tested for. If a condition is diagnosed, your doctor will explain to you what the condition is and what the implications are. It is important to consider the choices available to you and to make an informed decision.
Possible side effects/risks
There is a 1% risk of miscarriage– as a result of amniocentesis. There is very little risk of the needle hurting the baby, particularly when the needle is guided by ultrasound. If you experience any abdominal pain, loss of blood or fluid from the vagina following the procedure, please consult your doctor.
More information
 |
For more information about pregnancy, including preconception advice, stages of pregnancy, investigations, complications, living with pregnancy and birth, see Pregnancy. |
 |
For more information about different pregnancy investigations, including pregnancy tests, obstetric ultrasound, amniocentesis and chorionic villus sampling as well as useful tools and animations, see Pregnancy Investigations. |
References
- Ball, R. H. ‘Invasive fetal testing’, Current Opinion in Obstetrics and Gynaecology. 2004; 16(2):159-62.
- Boyle, M. Antenatal Investigations. Cheshire, Books for Midwives Press, 1995.
- Chudleigh, T. and Thilaganathan, B. Obstetric ultrasound: How, Why and When. London, Elsevier Churchill Livingstone, 2004.
- Dugoff, L. and Hobbins, J. C. ‘Invasive Procedures to Evaluate the Fetus’, Clinical Obstetrics and Gynaecology. 2002; 45(4):1039-53.
- Gosden, C., Tabor, A., Leck, I., Grant, A., Alfirevic, Z. and Wald, N. Amniocentesis and Chorionic Villus Sampling. In: Antenatal & Neonatal Screening. Oxford, Oxford University Press, 2000.
- Maiques, V., Garcia-Tejedor, A., Perales, A. and al., e. ‘HIV detection in amniotic fluid samples: amniocentesis can be performed in HIV pregnant women?’ European Journal of Obstetrics and Gynaecology and Reproductive Biology. 2003; 106:137-41.
- MRC Working Party on Amniocentesis. ‘An assessment of the hazards of amniocentesis’, British Journal of Obstetrics and Gynaecology. 1978; 85(suppl. 2):1-41.
- Papp, C. and Papp, Z. ‘Chorionic villus sampling and amniocentesis: what are the risks in current practice?’ Current Opinion in Obstetrics and Gynaecology. 2003; 15:159-65.
- Tabor, A., Philip, J., Madsen, M., Bang, J., Obel, E. and Norgaard-Pedersen, B. ‘Randomised controlled trial of genetic amniocentesis’, Lancet. 1986; 1(1287-93.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







