- Introduction
- The menstrual cycle
- The ovarian cycle
- The uterine cycle
- Summary of the 1st gestational week
- Pregnancy week by week
Introduction
Week 1 of the 40 weeks of gestation begins with the last menstrual period and before conception. To gain a better understanding of the processes that lead to pregnancy, let us briefly discuss the menstrual cycle.
Menstrual cycle
The menstrual cycle has two components: the ovarian cycle and the uterine cycle. Both of these components are coordinated by the hormonal changes taking place within the body. They start and end with the menstrual period, and function together to allow pregnancy to occur.
The ovarian cycle
The ovarian cycle is the cyclical event co-ordinated by a complex series of hormonal interactions that bring about the release of an egg (ovum) ready for fertilisation (union of the egg and sperm).
It can be divided into three phases:
- Follicular phase;
- Ovulation; and
- Luteal phase.
The follicular phase is the most variable part of the cycle, generally occurring over a 10- to 14-day period. The onset of the follicular phase coincides with the beginning of the menstrual period (bleeding). During the follicular phase, the hormonal changes see the development of a number of follicles, each of which contains an immature ovum or egg. Follicles reside within the ovaries. By Day 5–7, one of these follicles becomes dominant – usually the follicle with the richest blood supply, the greatest oestrogen production, and the greatest amount of an enzyme required for oestradiol production. Throughout the remainder of the follicular phase, this dominant follicle matures into an ovum (egg) and awaits ovulation.
The release of the egg from the ovarian follicle into the fallopian tubes occurs 24–36 hours after a rise in luteinising hormone (LH). This is known as ovulation.
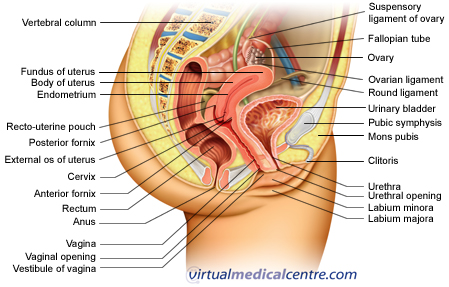
 |
For more information, see Anatomy of the Female Reproductive System. |
The luteal phase is the time between ovulation and the onset of menses (the menstrual period). Unlike the follicular phase which has a variable time course, the luteal phase is usually constant and approximately 14 days duration. During this period, the site from which the egg was released forms what is called the corpus luteum. The corpus luteum is responsible for the production of large amounts of oestrogen and progesterone, which support pregnancy if conception occurs.
Should pregnancy occur, a hormone released from placental tissue, human chorionic gonadotrophin (hCG), stimulates continued release of hormones from the corpus luteum.
If pregnancy does not occur, the levels of oestrogen and progesterone from the corpus luteum fall, resulting in changes in the endometrium (inner lining of the uterus) and hence menstrual bleeding.
Book your health appointments online
Find and instantly book your next health appointment with Healthengine
The uterine cycle

- Menstrual phase;
- Proliferative phase; and
- Secretory phase.
The menstrual phase is the first of the uterine cycles and refers to the period of time in which the endometrium sloughs off and sheds, expelling the blood and endometrial cells through the vagina. The 1st day of menstruation marks the beginning of the menstrual cycle. Menses (active menstrual bleeding) typically lasts 4–5 days.
The proliferative phase coincides with follicular growth in the follicular phase of the ovarian cycle. In this phase, the endometrium is renewed from cells growing and dividing from its base layer. There is a two- to three-fold increase in both the thickness of the endometrium and its water content. The proliferative phase typically lasts about 9 days.
The secretory phase coincides with the formation, function and growth of the corpus luteum in the ovarian cycle. In this phase, endometrial glands produce a glycogen-rich substance. The increase in secretions from the endometrium in this phase of menstruation creates an ideal environment in the uterus for the implantation of the blastocyst (the beginning of the embryo produced by cellular division and replication of the fertilised egg) if fertilisation has occurred. The secretory phase typically lasts about 13 days.
|
Menstruation occurs in cycles. The ovaries prepare an egg (oocyte) for release and the womb (uterus) prepares a lining to nourish the egg if it is fertilised. When the egg is not fertilised, the lining of the womb is shed and a woman gets her period (menstrual bleeding). Menstruation typically occurs in 28 day cycles so most women get their period every 28 days. However, some women have longer cycles and may only get their period every 40 days, while other have shorter menstrual cycles and may get their periods as often as every 21 days. The menstruation calculator determines when your next period is due based on a 28 day menstrual cycle. All you need to do is enter the date when your last menstrual bleeding began, and the calculator will tell you when to expect your next period. |
|
| 1. Select your menstrual cycle length: days | |
|
2. Select your last Menstrual Date:
|
Next Menstrual Date Due:
|
|
The information presented here is for general purposes only and should not be used to make diagnosis or treatment decisions. For specific information about your health you should see a health professional. Reference
|
|
 |
For more information, see Menstruation. |
Summary of the 1st gestational week
The first gestational week of pregnancy is marked by the first day of your last menstrual period (LMP). Active bleeding (menses) continues for 4–5 days in total. The menstrual period is followed by regrowth of the endometrium, which occurs during the proliferative stage. Endometrial regrowth is initiated in week 1, but not completed until the end of week 2. The ovaries are in their follicular stage of development, and by the end of week 1, a single dominant follicle should be formed.
Pregnancy week by week
 |
To go back, see Stages of Pregnancy: Introduction. |
 |
For more information, see 2 Weeks Pregnant: Ovulation. |
More information
 |
For more information on foetal development and maternal changes during pregnancy, see Stages of Pregnancy. |
 |
For more information about pregnancy, including preconception advice, stages of pregnancy, investigations, complications, living with pregnancy and birth, see Pregnancy. |
References
- Emans SJH, Laufer MR, Goldstein DP (eds). Pediatric and Adolescent Gynecology (5th edition). Philadalphia: Lippincott Williams & Wilkins; 2005. [Book]
- Speroff L, Fritz MA. Clinical Gynecologic Endocrinology and Infertility (7th edition). Philadelphia: Lippincott Williams & Wilkins; 1994. [Book]
- Johnson LR, Byrne JH. Essential Medical Physiology (2nd edition). Philadelphia: Lippincott-Raven; 1998. [Book]
- Moore KL, Persaud TVN. The Developing Human: Clinically oriented embryology (7th edition). Philadelphia: Saunders; 2003. [Book]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.