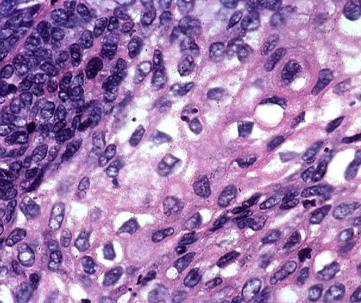
- Cancer: Incidence and disease burden
- The cell cycle
- What causes unregulated cell growth?
- Tumour grade
Cancer: Incidence and disease burden
Cancer, a condition of abnormal cell growth, is the second most common cause of death in developed countries. In the year 2000, there were some 6.2 million cancer related deaths, accounting for 12% of all deaths globally. In the same year, ten million new cases of cancer were diagnosed (5.3 million in men and 4.7 million in women). Around one third of new cancers could be prevented through the modification of lifestyle factors, particularly smoking, diet and alcohol consumption. Cancer treatment could be more effective if cancer was diagnosed earlier – up to a third of cancer related deaths could be prevented through early detection of cancer.
In Australia, cancer is responsible for more than 7% of all illnesses and deaths. In 2001, there were 88,398 new incidents of cancer in Australia (excluding skin cancers, which are much more common) and 33,319 deaths caused by cancer. The most common type of cancers in Australia are cancers of the colon and rectum (bowel), followed by breast cancers, prostate cancer, melanoma and lung cancer.
The cell cycle
Normal cell growth in our bodies is carefully regulated so that the number of new cells produced is equal to the number of cells lost naturally through cell death or injury. The body produces new cells in a process known as the cell cycle. Understanding how the cell cycle works can help you understand how tumours form and how cancer treatment works.
The cell cycle is a complex sequence of events. The first stage of the cell cycle is a process known as mitosis, in which the cell nucleus (which contains DNA) divides to form two separate cells. Mitosis (denoted M in the cell cycle) is followed by a gap phase (denoted G1) in which the cell prepares enzymes that will allow its DNA to duplicate. The DNA in the cell then divides in the synthesis phase, denoted (S). During a second gap phase (G2), the cell produces proteins that enable it to undergo the first/final stage, mitosis (M). Immediately following mitosis, most cells leave the cell cycle and become dormant (phase denoted G0). Cells will eventually leave the cycle forever and die, which is known as the process of apoptosis.
At any time, cells may fall into one of 3 categories:
|
Cancer cells
While cancer cells undergo the same cell cycle process as normal cells, they differ from normal cells because:
- Cancer cells replicate in an uncontrolled manner, meaning that more new cells are produced than die.
- Cancers cells can survive amongst cells of different types, and can therefore move from one part of the body to another (e.g. the kidney to the pancreas). This is known as metastasis. Healthy cells, by contrast, stick with other like cells (e.g. kidney with kidney cell).
Tumours form when an excess of cancerous cells build up as a result of the unregulated division of existing cells. Not all tumours are cancerous – those that are localised and cannot move to other sites (i.e. cannot metastasise) are known as benign and are not considered cancers. Malignant tumours, on the other hand, are those that spread, or metastasise, to distant sites in the body; these are considered cancerous.
What causes unregulated cell growth?
Some individuals are said to have a genetic predisposition for cancer; they inherit defective genes, which either fail to switch off cell growth, or initiate growth too easily.
However, most cases of cancer are a result of exposure to so-called carcinogenic factors (i.e. things that cause cancer), such as smoking, obesity and alcohol consumption.
Tumour grade

Methods of classification:
After cancer is diagnosed, a doctor will usually classify the cancer into a stage which indicates how severe the cancer is and how likely it is that treatment will be successful.
- The TNM system of staging is a method of classifying tumours based on the size of the primary tumour (T), the extent to which cancer has spread to lymph nodes (N), and the presence or absence of metastasis (M). The combination of scores for T, N and M will tell the doctor which stage the cancer is at. A cancer’s stage does not change, even if the cancer gets worse – the stage always refers to the characteristics of the cancer when it was diagnosed. The TNM staging system is used for all cancers except lymphoma, cancers of the brain, and non-Hodgkin’s lymphoma.
- The Ann Arbor system is used for classifying lymphoma.
- The Dukes’ system can be used to classify colorectal cancers.
- The Gleason score is used for classifying prostate cancers.
More information
 |
For more information on breast cancer, types of breast cancer and its investigations and treatments, as well as some useful videos, see Breast Cancer. |
 |
For more information on gastric cancer, see Gastric Cancer. |
 |
For more information on kidney cancer, see Kidney Cancer. |
 |
For more information on prostate cancer, including diagnoses, types of treatments, and some useful tools, videos and animations, see Prostate Cancer. |
References
- Parkin DM, Bray FI, Devesa SS. Cancer burden in the year 2000. The global picture. Eur J Canc. 2001; 37(Suppl 8): S4-66.
- Mathers CC, Vos ET, Stevenson CE, Begg SJ. The Australian Burden of Disease Study: Measuring the loss of health from diseases, injuries and risk factors. MJA. 2000; 172(12): 592-96.
- Cancer in Australia 2001 [online]. Australian Institute of Health and Welfare. 15 December 2004 [cited 9 May 2008]. Available from URL: www.aihw.gov.au/ publications/ index.cfm/ title/ 10083
- Collins J, Jacks T, Pavletich NP. The cell cycle and cancer. Proc Nat Acad Sci USA. 1997; 94(7): 2776-8.
- Pierobin M, Geho D, Belluco C, Liotta L. Invasion and metastasis. In: Martin A [ed]. The Cancer Handbook. London: John Wiley and Sons Inc, 2007 [online]. Wiley Interscience. 30 Jan 2008 [cited 9 May 2008]. Available from URL: http://www3.interscience.wiley.com
- Delia D, Buscemi G. Regulation of the cell cycle, cell cycle checkpoints and cancer. In: Martin A [ed]. The Cancer Handbook. London: John Wiley and Sons Inc, 2007 [online]. Wiley Interscience. 30 Jan 2008 [cited 9 May 2008]. Available from URL: http://www3.interscience.wiley.com
- Boffetta P, Hashibe M. Alcohol and cancer. Lancet Oncology. 2006; 7(2): 149-56.
- Greene FL, Page DL, Fleming ID, Fritz AG, Balch CM, et al [eds]. American Joint Committee on Cancer Staging Manual [6th edition]. New York: Springer, 2002.
- Rosenburg SA. Validity of the Ann Arbor staging classification for the non-Hodgkin’s lymphomas. Cancer Treat Rep. 1977; 61(6): 1023-7.
- O’Dowd G, Veltri RW, Miller MC, Strum SB. The Gleason score: A significant biologic manifestation of prostate cancer aggressiveness on biopsy [online]. Prostate Cancer Research Institute. January 2001 [cited 28 November 2008. Available from URL: http://www.prostate-cancer.org/ education/ staging/ Dowd_GleasonScore.html
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.