- What are sperm?
- The role of sperm in fertilisation
- Male factor infertility
- What is sperm retrieval and when is it performed?
- How can sperm be retrieved?
- Semen analysis (sperm count testing)
- How is an abnormal semen analysis result determined?
- Treatment options for sub-optimal sperm production
- Sperm preparation for assisted reproduction techniques
What are sperm?
Sperm is the male gamete, that is, the male sex cell, or the cell in males which has the capacity to fertilise an egg (i.e. a female gamete, also known as an ovum or oocyte). Sperm are produced in the seminiferous tubes of the testes.
The pituitary gland at the base of the brain causes testosterone to be produced in the testes. Testerosterone causes sperms to be produced. The sperm production cycle takes approximately three months and a healthy man produces millions of new sperm each day.
Sperm are not visible to the human eye, however when viewed under a microscope they look a bit like tadpoles because they have a round head section and a long tail. The head of a sperm contains it nucleus, within which 23 chromosomes (i.e. tiny rod like structures which contain genetic information called DNA) are housed. The tail structure enables the sperm to move actively once it leaves the testicles. It helps propel sperm forward from the vagina (when sperm are expelled during sexual intercourse) toward the uterus in search of an oocyte in the fallopian tubes. The tail also provides the necessary motion for the sperm to bind to and penetrate an egg once it has been reached.
The role of sperm in fertilisation
In order to fertilise an egg and create an embryo, sperm must leave the testes and come into contact with a mature oocyte (i.e. an oocyte which is ready for fertilisation). Oocytes mature within ovarian follicles in a woman’s ovaries. Typically a single ovarian follicle will prepare an oocyte for release during each ovulatory cycle, and thus, a single mature oocyte will be released each time a woman ovulates. The oocyte is released from the follicle where it has matured, then leaves the ovaries and travels to the uterus via the fallopian tubes, usually every 28 days. For fertilisation to occur, sperm must enter the fallopian tubes while the mature oocyte is also there (i.e. just after the oocyte has been released from its follicle).
Sperm typically enter the fallopian tubes following unprotected sexual intercourse, during which a man’s testicles are stimulated to release sperm upon orgasm. Sperm leaves the testicles, via the epididymis and vas deferens (i.e. the tubes linking the testes to the urethra), where they combine with other fluids, known as the seminal fluids. The seminal fluid leaves the body via the urethral opening of the penis. If ejaculation occurs during unprotected sexual intercourse (i.e. while the man’s penis in inserted in the woman’s vagina without a protective barrier) the sperm will enter the vaginal cavity. If the sperm are motile (i.e. have the ability to move around or ‘swim’) they will travel up the vaginal tract to the cervical opening. Sperm must then travel through a layer of mucus which protects the cervical opening, before entering the woman’s uterus and fallopian tubes, where they may reach an egg.
In many cases the woman will not be ovulating at the time of sexual intercourse, therefore no mature oocyte will be present in the fallopian tubes and fertilisation will not occur. If there is a mature oocyte in the woman’s fallopian tubes and sperm are healthy, sperm will be attracted to the oocyte and attempt to swim to it, bind to its surface and eventually penetrate its zona pellucida (i.e. shell). Once the sperm has penetrated the zona pellucida it enters the nucleus of the egg, where the egg’s chromosomes (which contain the maternal DNA) are stored. When the sperm head penetrates the zona pellucida the 23 chromosomes contained in the sperm head join with the 23 chromosomes in the egg’s nucleus and form an embryo with 46 chromosomes (i.e. the number of chromosomes found in all normal human cells except gametes). The single celled embryo will then replicate to produce further 46 chromosome cells which will eventually form the foetus. It is this process of the egg and sperm combining their chromosomes which represents the end of the fertilisation process.
Male factor infertility

When a man produces a low number of sperm, the concentration of sperm in the ejaculate is much lower than in a man with healthy sperm production. Thus, the chance that one of the millions of sperm contained in the seminal fluid which is ejaculated upon orgasm will reach an oocyte in the woman’s fallopian tubes is greatly reduced.
The production of low quality sperm also reduces the chance of fertilisation. Low quality sperm are typically either immotile (i.e. they cannot move) or abnormally shaped, or both. Sperm which are immotile cannot travel up the vaginal tract and into the uterus, and thus cannot locate and fertilise a mature oocyte. Those which are abnormally shaped may or may not be able to move, however even if they manage to travel to an oocyte, they will usually be unable to bind to and penetrate its shell and the couple will be unable to conceive as a result.
In a minority of cases of male factor infertility, sperm production occurs normally in the testicles, but difficulties arise in the process of ejaculating sperm. Some men completely fail to ejaculate and this may result from spinal cord injuries, injuries to the testicles, or testicular conditions such as infection or cryptorchidism. Other men will be able to ejaculate, however their seminal fluid will not contain sperm. These cases are most commonly caused by obstructions in the epididymis and vas deferens (e.g. due to infection). In other cases of male factor infertility, ejaculation occurs however the sperm do not enter the woman’s vagina. For example retrograde ejaculation is a condition in which a man ejaculates into his bladder, and thus ejaculate is not expelled into a woman’s vagina, even if ejaculation occurs during sexual intercourse.
Male factor infertility can be diagnosed by a sperm analysis (sperm count test).
What is sperm retrieval and when is it performed?
Sperm retrieval is the process of retrieving sperm from a man for semen analysis testing or for use in assisted reproductive techniques.
Regardless of the intended use, sperm is of optimal quality when it is fresh, so whenever possible should be retrieved around an hour before it will be used. The sample should be collected after not less than 48 hours and not more than 7 days of sexual abstinence.
In cases where it is not practical or possible to retrieve sperm on the day of its intended us, sperm may be retrieved in advance, however it must then be cryopreserved and thawed immediately before use.
How can sperm be retrieved?

Ejaculation is the natural process through which a man’s body expels sperm and it occurs as a result of sexual stimulation, coinciding with the man’s orgasm. Masturbation is the technique most commonly used to induce ejaculation for sperm retrieval purposes. It is a relatively simple technique, which the patient can perform without the assistance of a health professional.
Masturbation provides a complete semen sample, which is important for both semen analysis testing and assisted reproduction, because the first quantity of seminal fluid expelled during ejaculation is typically of the best quality.
Results will therefore be inaccurate or outcomes less than optimal, if this portion of the ejaculate is not captured. Masturbation is also the preferred technique for sperm retrieval because it provides a semen sample that is uncontaminated (e.g. by vaginal fluids).
So that a man can induce ejaculation through masturbation in comfort and privacy, most infertility clinics provide a private room in which the man, and if necessary his partner, can perform masturbation. The man will be provided with a sterile container, labelled with identifying information, in which the ejaculate can be stored. He will be instructed to check the identifying information to ensure it is his, then to ejaculate into the container and ensure all the ejaculate, and particularly the first portion, is captured. The semen specimen should then be handed immediately to the treating clinicians, who will record the date and time of ejaculation and store the semen sample at room temperature if it is to be used immediately, or cryopreserve it for future use.
For men who find it difficult to achieve orgasm and ejaculate in the clinic environment, some clinics allow the male partner to complete sperm retrieval at home. There are no significant differences in pregnancy rates following intrauterine insemination when sperm is retrieved at home or in a clinic, as long as the sperm sample reaches the clinic quickly (i.e. one hour). When sperm retrieval is performed at home, the man will be provided with a sterile container, labelled with the couple’s identifying information, in which to collect his ejaculate. The time and date of collection should be recorded on the jar, immediately following ejaculation. The patient will be instructed to seal the container and ensure it is kept at room temperature until it reaches the clinic. Because sperm performs better when it is fresh, it is important that the sample reaches the clinic within one hour of ejaculation. For patients who are geographically remote from infertility clinics or do not have reliable forms of transport to reach the clinic, home retrieval is therefore not an option.
Ejaculation – sexual intercourse

Vibration or electro stimulation
For men who do not produce ejaculate, vibration or electro stimulation techniques are often effective in inducing ejaculation. They are relatively simple techniques which do not require anaesthetic, however they do require the assistance of a health professional and special medical equipment. The vibro-stimulation technique involves holding a special vibrating instrument to a man’s penis. The aim is to induce an ejaculation by stimulating ejaculatory reflexes. The electro stimulation technique involves inserting a electro-stimulation probe into the man’s rectum. Electrical impulses are then sent through the probe to stimulate sensitive nerves in this region, which can induce an erection and ejaculation.
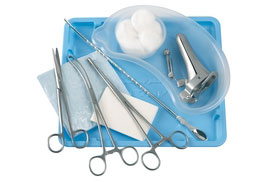
- Microsurgical epididymal sperm aspiration (MESA): a surgical technique in which a small incision (1-1.5cm) is made in the scrotum, to enable a special microscope to be inserted to view the epididymis. A needle is then inserted into a suitable area of the scrotum and sperm are aspirated into the needle. The procedure is usually performed under local anaesthetic;
- Percutaneous epididymal sperm extraction (PESE): a minimally invasive surgical technique in which a fine needle is inserted through the skin of the scrotum into the epididymis, and sperm are sucked into the needle. This is the simplest surgical sperm retrieval procedure and is performed under local anaesthetic, however does not always result in a sufficient quantity of sperm being retrieved;
- Fine needle aspiration (FNA): a minimally invasive surgical technique in which a fine needle is inserted directly into the testicle, and aspirated in the hope of retrieving sperm cells. It is a simple technique however generally results in only a few sperm being retrieved, meaning that sperm cannot be cryopreserved for future use;
- Testicular sperm extraction (TESE)- Open Testicular Biopsy: is a highly invasive, open surgical procedure performed under general anaesthetic. The scrotum and testes are cut open, before testicular tissues are cut away and examined for sperm, which, if present can be extracted.
There is currently insufficient evidence to determine which of the sperm retrieval techniques have the best outcomes in terms of pregnancy rates or patient satisfaction.
Semen analysis (sperm count testing)
The results are compared to reference values published by the World Health Organisation. Semen analysis testing investigates a number of characteristics of the seminal fluid and the sperm it contains including:
- Volume of ejaculate: the quantity of seminal fluid which is released on ejaculation is measured;
- Sperm concentration and number: the concentration of sperm in ejaculate is determined by counting the number of sperm in each field of view of the microscope. The concentration of sperm per ml of ejaculate can then be calculated;
- Sperm motility: the ability of sperm to move is a prerequisite for natural conception and many assisted reproductive technology procedures also depend on the ability of the sperm to move and bind to an egg. The semen sample is therefore examined to determine what proportion of sperm is motile and to what extent they move. Sperm can be classified as rapidly progressive (i.e. moving quickly), slowly progressive (i.e. moving slowly), non progressive (moving very slowly) or immotile (not moving at all);
- Sperm morphology: the shape of sperm is an important predictor of a sperm’s capacity to fertilise an egg and is thus an important part of semen analysis testing. The shape of the head, tail and mid-piece of up to 200 sperm will be examined and their details recorded so that the proportion of morphologically normal sperm in the ejaculate can be calculated;
- pH: a pH test is performed to assess the acidity of seminal fluid;
- White blood cells: the concentration of white blood cells in the seminal fluid is assessed, to determine whether or not there are any infections in the man’s genital tract;
- Liquification time: immediately after ejaculation, seminal fluid is a thick mucus-like substance in which sperm are suspended. Normal seminal fluid will change to watery liquid within 15-60 minutes of ejaculation;
- Vitality: assesses the proportion of sperm in the suspension which are alive;
- Sperm antibodies: are produced by the body’s immune system and reduce the life span and impair the motility of sperm. Sperm are generally protected from these antibodies whilst in the testicles, however in men who have previously experienced testicular surgery or trauma, sperm antibodies may be found in the seminal fluid. In other cases the presence of sperm antibodies is unexplained.
How is an abnormal semen analysis result determined?
Analysis of the total quality and quantity of sperm in an infertile man is conducted as it allows clinicians to gain insight regarding the factors which are likely underpinning the couple’s infertility problems, but not because it enables clinicians to predict the likelihood of natural conception occurring at some point in the future.
When the results of the semen analysis fall within the parameters outlined by WHO (, the man’s sperm production is considered normal. When one or more of the test values fall outside the WHO criteria, a repeat semen analysis test is usually conducted (ideally 3 months after the first test) to confirm the result. Semen quality can vary considerably over time, due to the health, lifestyle and environmental conditions of the man whose semen is being analysed. Around 10% of men who return abnormal results in their first semen analysis test will actually have normal results when they are tested again.
|
World Health Organisation Reference Values for Semen Analysis Testing3 |
|
| Volume | > 2 mL |
| Sperm concentration | > 20 million/mL |
| Sperm number | > 40 million per ejaculate |
| Sperm motility | > 50% progressive or > 25% rapidly progressive |
| Morphology (strict criteria) | > 15% normal forms |
| White blood cells | < 1 million/mL |
| Immunobead or mixed antiglobulin reaction test* | < 10% coated |
| Vitality | ≥ 75% living |
| pH | ≥ 7.2 |
| Liquification time | < 60 minutes |
* for antisperm antibodies
Based on the results of semen analysis testing, a man will be given a sperm classification, using the following standard terminology:
- Normozoospermia: (i.e. normal sperm) is the classification for men whose semen parameters fall within the WHO reference values (i.e. >20 million sperm/ml of semen and no morphological or genetic defects in the sperm);
- Oligozoospermia: refers to seminal fluid in which the concentration of sperm is lower than the WHO reference values. 5-20 million sperm/ml of seminal fluid indicates mild-moderate oligozoospermia, while a concentration <5 million indicates severe oligozoospermia. Oligozoospermia may result from environmental conditions (e.g. exposure to pesticides, excessive testicular heat), recent illness, use of some recreational and prescription drugs, genital infections or testicular abnormalities (e.g. cryptorchidism);
- Asthenozoospermia: refers to a man who produces a greater proportion of sperm which are immotile or have reduced motility, compared to the WHO reference values;
- Teratozoospermia: is characterised by the production of a large proportion of sperm which have morphologically abnormal forms (e.g. sperm with abnormal shape which cannot bind to and penetrate an egg for fertilisation). According to the WHO criteria a man with <15% morphologically normal forms is classified teratozoospermia;
- Oligoasthenoteratozoospermia: is a condition in which all sperm variables are subnormal when compared to the WHO reference values;
- Azoospermia: is a condition in which semen is present but contains no sperm;
- Aspermia (anejaculation):is an uncommon condition in which ejaculation fails or seminal fluid is not expelled from the man’s body upon ejaculation;
- Leucocytospermia: refers to a concentration of white blood cells in semen higher than the WHO reference values;
- Necrozoospermia: refers to semen in which all sperm are non-viable or non-motile.
Treatment options for sub-optimal sperm production

- Normozoospermia: if a man’s semen analysis results are normal, female factors may underpin the couple’s infertility (in which case the best treatment option will be determined based on the female infertility factors) or the cause of infertility may be unidentifiable. In cases of unexplained infertility, intrauterine insemination is often instituted as first line treatment, however recent evidence from a large randomised controlled trial demonstrates that intrauterine insemination (with or without ovarian stimulation) is no more effective than expectant management (waiting and seeing) in terms of achieving conception;
- Oligozoospermia: when sperm concentration is low, a man may still be able to conceive naturally, however the chances of conception are reduced. If natural conception fails, intrauterine insemination is indicated as first line treatment, following which in vitro fertilisation or intracytoplasmic sperm injection may be instituted if conception is still not achieved;
- Asthenozoospermia: men with largely immotile sperm have a very poor chance of conceiving naturally or through intrauterine insemination or in vitro fertilisation, as all of these techniques are dependent on the ability of sperm to move to and penetrate an oocyte. Intracytoplasmic sperm injection, an in vitro fertilisation procedure in which a single sperm is injected directly into the nucleus of a mature oocyte (i.e. is injected through the egg’s zona pellucida), is the usual treatment in cases where sperm are largely immotile. The likelihood of a successful intracytoplasmic sperm injection outcome are however reduced when the injected sperm is immotile;
- Teratozoospermia: abnormally shaped sperm are typically unable to bind to and/or penetrate the egg’s zona pellucida and often also have impaired motility. Thus men with this condition have little chance of conceiving naturally, through intrauterine insemination or in vitro fertilisation. Treatment with intracytoplasmic sperm injection is therefore indicated in these men;
- Oligoasthenoteratozoospermia: in cases of men with more than one sub-optimal semen parameter, conception can usually be achieved through intracytoplasmic sperm injection;
- Azoospermia: is treatable with gonadotrophin injections (in cases of hypothalamic pituitary dysfunction) or surgery to restore tubal patency (in cases of epidydimal or vas deferens blockage). Where these treatments fail, the retrieval of sperm using surgical methods may enable successful intrauterine insemination, in vitro fertilisation or intracytoplasmic sperm injection;4
- Aspermia: while there is no effective treatment which can restore ejaculation in anejaculatory men, surgical sperm retrieval techniques can be used to obtain sperm from the testicles or epidydimus so that intracytoplasmic sperm injection can be performed;
- Leucocytospermia: as increased concentrations of white blood cells typically indicate genital tract infection, a course of antibiotics will usually treat the infection and cause the white blood cell count to decrease to within normal parameters;
- Necrozoospermia: when semen analysis reveals the ejaculate contains no sperm, or only dead sperm, surgical techniques may enable viable sperm to be retrieved either from the testicles or the epididymis, for intracytoplasmic sperm injection;
- Presence of sperm antibodies: there is no effective treatment for infertility stemming from the production of antisperm antibodies.
Sperm preparation for assisted reproduction techniques

Sperm preparation is a procedure in which the most viable sperm in an ejaculate (i.e. the most morphologically normal and motile) are separated from non-viable and dead sperm, white blood cells and bacteria in the suspension. This is because these components of the suspension are thought to impair the fertilisation process. Following separation, the motile sperm are re-suspended to form a solution with a high concentration of sperm.
There are a range of techniques which can be used to prepare sperm and the technique used will depend upon the assisted reproductive technique procedure and the quality of the semen sample. The procedures use different techniques, however are similar in that they all aim to separate viable from non-viable sperm.
The most common semen preparation techniques are:
- Discontinuous density gradient: is a technique in which all sperm in the seminal fluid are separated by centrifugation (i.e. spinning);
- Swim up: is a technique in which the most motile sperm are selected from the ejaculate. Fresh semen is covered with a medium and placed in a cylinder which is laid at a 45oC angle. Motile sperm in the ejaculate will then swim up to the top of the tube, leaving immotile sperm and debris in the lower part of the cylinder.
For more information
 |
For more information on sperm health and male fertility, see Sperm Health. |
 |
For more information on infertility, including investigations and treatments, as well as some useful animations, see Infertility. |
References
- McLachlan RI, de Kretser DM. Male infertility: The case for continued research. Med J Aust. 2001;174(3):116-7.
- Hirsch A. Male subfertility. BMJ. 2003;327(7416):669-72.
- Rowe PJ, Comhaire FH, Hargreave TB, Mahmoud AMA. WHO manual for the Standardized Investigation, Diagnosis and Management of the Infertile Male (4th edition). Cambridge: Cambridge University Press; 1999.
- National Collaborating Centre for Women’s and Children’s Health. Clinical guideline: Fertility: Assessment and treatment for people with fertility problems [online]. Royal College of Obstetricians and Gynaecologists. 1 February 2004 [cited 30 December 2008]. Available from URL: http://www.rcog.org.uk/womens-health/clinical-guidance/fertility-assessment-and-treatment-people-fertility-problems
- Bhattacharya S, Harrild K, Mollison J, Wordsworth S, Tay C, Harrold A, et al. Clomifene citrate or unstimulated intrauterine insemination compared with expectant management for unexplained infertility: Pragmatic randomised controlled trial. BMJ. 2008;337:a716.
- Malter HE, Cohen J. Intracytoplasmic sperm injection: Technical aspects. In: Vayena E, Rowe PJ, Griffin PD (eds). Current Practices and Controversies in Assisted Reproduction [online]. Geneva: World Health Organisation; 2002 [cited 30 December 2008]. pp. 126-33. Available from URL: http://whqlibdoc.who.int/hq/2002/9241590300.pdf
- Gerris J. Methods of semen collection not based on masturbation or surgical sperm retrieval. Hum Reprod Update. 1999;5(3):211-5.
- Song GJ, Herko R, Lewis V. Location of semen collection and time interval from collection to use for intrauterine insemination. Fertil Steril. 2007;88(6):1689-91.
- Shafik A. The mechanism of ejaculation: The glans-vasal and urethromuscular reflexes. Arch Androl. 1998;41(2):71-8.
- Howards SS, Jones EV, Wind TC, Edlich RF. Functional electrical stimulation for ejaculation. J Long Term Eff Med Implants. 2002;12(3):201-9.
- Ezeh UI, Moore HD, Cooke ID. A prospective study of multiple needle biopsies versus a single open biopsy for testicular sperm extraction in men with non-obstructive azoospermia. Hum Reprod. 1998;13(11):3075-80.
- Khalifa Y, Grudzinskas JG. Minimally invasive surgery for male subfertility. BMJ. 1996;312(7022):5-6.
- Craft I, Tsirigotis M. Simplified recovery, preparation and cryopreservation of testicular spermatozoa. Hum Reprod. 1995;10(7):1623-6.
- Van Peperstraten A, Proctor ML, Johnson NP, Philipson G. Techniques for surgical retrieval of sperm prior to intra-cytoplasmic sperm injection (ICSI) for azoospermia. Cochrane Database Syst Rev. 2008;(2):CD002807.
- Boomsma CM, Heineman MJ, Cohlen BJ, Farquhar C. Semen preparation techniques for intrauterine insemination. Cochrane Database Syst Rev. 2007;(4):CD004507.
- Counsel M, Bellinge R, Burton P. Vitality of oligozoospermic semen samples is improved by both swim-up and density gradient centrifugation before cryopreservation. J Assist Reprod Genet. 2004;21(5):137-42.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







