- What is Emphysema
- Statistics on Emphysema
- Risk Factors for Emphysema
- Progression of Emphysema
- Symptoms of Emphysema
- Clinical Examination of Emphysema
- How is Emphysema Diagnosed?
- Prognosis of Emphysema
- How is Emphysema Treated?
- Emphysema References
What is Emphysema
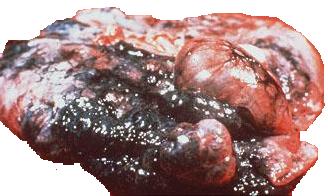
Emphysema is a chronic disease affecting the lungs. People have two lungs as demonstrated in the diagram below. The lungs receive air that travels from the nose and mouth, through the trachea (windpipe) and to the smaller airways. The lungs consist of a series of folded membranes (the alveoli) which are located at the ends of very fine branching air passages (bronchioles). The alveoli are responsible for the absorption of oxygen and removal of carbon dioxide from the body. Emphysema involves abnormal permanent enlargement of the tiniest airspaces of the lungs, the alveoli and respiratory bronchioles. There is also destruction of the walls of these airspaces. Emphysema usually occurs with chronic bronchitis as part of the disease complex known as Chronic Obstructive Pulmonary Disease (COPD). There is significant overlap between chronic bronchitis and emphysema. Below is a postmortem lung specimen of a chronic emphysema sufferer.
Statistics on Emphysema
Emphysema, along with chronic bronchitis (together known as COPD) is a major cause of disability, hospital admissions, and mortality. More than half a million Australians are estimated to suffer from moderate to severe disease, and COPD ranks fourth among the common causes of death in Australian men, and sixth in women. The global prevalence is quoted at 7.5% of which 1.8% have emphysema alone. COPD occurs in 18% of male and 14% of female smokers and in 7% and 6% respectively in people who have never smoked. Emphysema has a strong relationship with cigarette smoking and smokers tend to have more severe disease.
Risk Factors for Emphysema
- Cigarette smoke is by far the most important factor in the development of emphysema and COPD. Those who smoke 30 cigarettes per day are 20 times more likely to die from COPD than non-smokers.
- About 2% of cases of emphysema are due to hereditary deficiency of the alpha-1 antitrypsin gene. This gene abnormality occurs in about 1 in 5000 people, but does not always cause disease. Alpha-1 antitrypsin is an important enzyme in the lung that prevents destruction of the alveoli walls.
Progression of Emphysema

Nearly all sufferers of emphysema are smokers or have smoked in the past. In susceptible smokers, cigarette smoking results in a steady decline in lung function. Smoking cessation, even late in the course of the disease may result in mild improvement in lung function, and more importantly it will slow the rate of decline in lung function. Emphysema usually presents in about the fifth decade although you may recall some breathing troubles prior to this time. If you have a deficiency in the alpha-1 antitrypsin gene your disease may present even earlier. In general emphysema gradually causes a decline in function and you may notice you become less capable of performing normal activities. Impairment increases as the disease progresses, but it may go unrecognised until later. In advanced stages of disease patients can become short of breath even at rest which is particularly disabling for patients. Emphysema sufferers also have a lower expected life expectancy than the general population.
Possible complications of emphysema include:
- Secondary polycythaemia (abnormally high amount of red blood cells causing sluggish blood flow and an increased risk of clotting).
- Right heart failure.
- Pneumothorax (escape of air from the lung into the pleural cavity).
- Respiratory failure– Often caused by acute infections of the lungs.
Symptoms of Emphysema
Most patients with emphysema have smoked at least 20 cigarettes per day for 20 or more years before the symptoms develop. A small proportion of patients will have a family history of emphysema (from alpha-1 antitrypsin deficiency) and may also have symptoms of cirrhosis or chronic liver disease. The most common symptoms of emphysema include shortness of breath and cough. You may also notice that you cough up mucus or sputum if you have concurrent chronic bronchitis. Wheezing may occur in some patients, particularly during exertion and exacerbations. Symptoms of emphysema usually present in the fifth decade of life when there has already been a significant decline in lung function. Sometimes emphysema can present acutely with a respiratory illness or sudden onset of shortness of breath. As the disease progresses you may notice increasing shortness of breath. In advanced disease, severe breathlessness may occur with mild exercise such as dressing. You may also have shorter intervals between exacerbations. When you present to your doctor, the will ask several questions in order to gauge the severity of your disease.
Clinical Examination of Emphysema

Your doctor will perform a detailed examination of your respiratory system. This will include undressing your top, inspecting your chest, measuring your chest expansion and listening to your breath sounds. Important signs your doctor will be looking for include:
- Tachypnoea (rapid breathing).
- Prolonged expiratory phase of respiration
- Use of accessory muscles of respiration- Other muscles in your neck and between your ribs may contract as they try to help with the work of breathing.
- Reduced chest expansion.
- Hyperinflation- Your chest may become barrel-shaped due to air trapping. The anterior to posterior (front to back) distance becomes larger and the lungs may become so big they overlap the heart and push down the liver.
- Wheeze (a musical type sound heard through the stethoscope) is rarely present.
- Signs of heart failure such as peripheral oedema (swelling) may be present in advanced disease.
- Evidence of smoking such as odour or nicotine staining of the fingernails or teeth.
Classically, the patient with significant emphysema is barrel chested, short of breath, and sits forward in a hunched-over position, breathing through pursed lips to try to prevent air trapping. Rarely will you be cyanosed (blue discolouration of the skin). This typical appearance is described as “pink puffers” as opposed to the classic “blue bloater” appearance seen in chronic bronchitis.
How is Emphysema Diagnosed?
Your doctor may perform number of tests to confirm the diagnosis of emphysema and determine the severity. Tests performed may include:
- Blood tests- Specifically looking at the concentration of red blood cells. Haemoglobin levels and the concentration of red blood cells may be increased due to the chronic lack of oxygen in the body (an attempt at compensation). This process is called secondary polycythaemia.
-
Chest x-ray– This helps to show hyper-expansion of the lungs. The lung fields may look enlarged and empty and may flatten out the diaphragm. The doctor may also see bullae (dilated airspaces) from severe emphysema at the outside of the lungs. In many cases however the chest x-ray may be normal.
- ECG or Echocardiogram– These tests can detect signs of right heart failure (a complication of emphysema and COPD).
- Pulmonary/Lung Function tests– Spirometry is the best test to detect airflow limitation and obstruction. Unlike asthma, the airflow limitation in chronic obstructive pulmonary diseases is largely irreversible.
- Blood gases- These may also be normal but in the later stages of disease you may have low oxygen and high carbon dioxide levels.
- High resolution CT– This is probably the best test for detecting emphysema and bullae (big dilated air spaces).
Prognosis of Emphysema
The prognosis of emphysema depends on several factors. One of the most important factors determining your outcome is whether you continue to smoke. Cessation of smoking improves symptoms and prognosis even in patients with severe disease. Your initial lung function and subsequent reductions is also important. This is usually measured by lung function tests (particularly FEV1). In general a lower FEV1 is associated with reduced survival. Patients with deficiency of alpha-1 antitrypsin may have rapid declines in lung function which is made worse by smoking. The presence of complications such as heart failure, respiratory failure, and exacerbations also determine your overall outcome and mortality. In most patients with emphysema, airflow limitation is progressive, eventually leading to significant disability and reduced survival. Treatment of emphysema is difficult with only approximately one quarter of patients benefiting from the usual medical treatments. In addition, these medications can cause significant side effects.
How is Emphysema Treated?
The goal of treatment for emphysema is mainly to improve your quality of life by controlling symptoms and preventing exacerbations of disease (sudden onset of symptoms and decline in function). Your doctor can help explain your condition to you and it is best if you try to become actively involved in you management. An overview of possible treatments that may be used for your emphysema as outlined below:

Quitting smoking Stopping smoking is the most important treatment for emphysema. Quitting smoking, will slow down the rate of progression of disease, improve your symptoms and prolong your survival, irregardless of the underlying severity of disease. Your doctor will provide you with education and advice on the importance of quitting smoking. They can also prescribe a drug called bupropion (Zyban) and nicotine replacement therapy (as patches, gum, lozenges etc) to reduce your cravings. It is also beneficial for you to be involved in counseling and other supportive measures. Your doctor will organise a smoking cessation program with you. This will involve choosing a quit date, education and support measures.
Drug therapy Drugs are used in emphysema to suppress symptoms and for treatment of acute exacerbations. Bronchodilators (such as Ventolin, Seretide and Atrovent given as puffers or nebulisers) can help improve your lung function. However these improvements are usually much less than with other diseases such as asthma. Your doctor may also use steroids to control your symptoms. Usually you will be given a trial of oral steroids to see if you respond before using long-term inhaled steroids. Antibiotics are taken for short-term exacerbations of disease. Your doctor may also prescribe agents to reduce the thickness of your sputum (called mucolytics, for example acetylcysteine). Studies have shown these agents may reduce the frequency of exacerbations. If you have alpha-1-antitrypsin deficiency you may also be treated with weekly or monthly injections of this specially synthesised agent. This may prevent further decline in lung function but it cannot reverse the damage that has already occurred. In addition, it not yet known for sure whether this treatment alters the course of disease.
Pulmonary rehabilitation Chest physiotherapy has been shown to help remove secretions in the airways. Various techniques are available such as steam inhalation, which assist sputum removal and improve your breathing. Your doctor will also enter you into exercise or pulmonary rehabilitation programs which have been shown to increase exercise tolerance, relieve symptoms and improve your quality of life.
Oxygen therapy If you have severe airflow limitation you may require home oxygen therapy, sometimes for up to 19 hours per day. Oxygen can be administered via nasal prongs (small plastic tubes into your nose) or via a mask. This treatment has been shown to prolong life in patients with severe emphysema and COPD who have stopped smoking. The best benefit from oxygen treatment is obtained if you have quit smoking. Furthermore, oxygen is flammable so smoking is in fact dangerous during this treatment
Other treatments
- Vaccinations- It is important that you have your yearly influenza vaccination, and pneumococcal vaccine. This will help reduce effective exacerbations from these agents.
- Diuretics– If you have right heart failure complications, you may be treated with tablets to remove the excess fluid.
- Acute exacerbations- Acute attacks should be treated with bronchodilators, supplemental oxygen, antibiotics and glucocorticoids.
- Depression– As emphysema and COPD can cause significant disabilities it is not uncommon for patients to become depressed. Counselling and antidepressant medications may help you overcome this.
- Weight control- It is important that you maintain a healthy weight and nutrition. In advanced disease you may notice marked weight loss. You should have a high fat content and nutritious diet to prevent muscle wasting. Alternatively if you are markedly overweight or obese you should try to reduce your weight to a healthy range with diet an exercise, in order to reduce demands on your lung function.
Emphysema References
- Cotran R, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- Hutchinson D. Pulmonary emphysema, BMJ 1994; 309: 1244-45.
- Kumar, Clark. Clinical Medicine, 5th Edition, Saunders, 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine, 6th Edition, Oxford University Press, 2004.
- McKenzie D, Frith P, Burdon J, Town G. The COPDX Plan: Australian and New Zealand Guidelines for the management of Chronic Obstructive Pulmonary Disease 2003, MJA 2003; 178: S1-S40. Available from: [URL Link]
- Reilly J, Silverman E, Shapiro S. ‘Chronic Obstructive Pulmonary Disease,’ in Kasper et al. Harrison’s Principle of Internal Medicine, 16th Edition (Chapter 242), McGraw-Hill, 2006.
- Sharma S. Emphysema, eMedicine, Web MD, 2006. Available from: [URL Link]
- Talley NJ, O’Connor S. Clinical examination- A Systematic Guide to Physical Diagnosis, 4th Edition. MacClennan & Petty, Sydney 2001.
- Venuta F, Bognolo G. Surgery for emphysema, BMJ 2006; 332: 375-376.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







