- What is Diabetes Mellitus Type 1 (insulin dependent, juvenile onset)?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- References
What is Diabetes Mellitus Type 1 (insulin dependent, juvenile onset)?
| Type 1 diabetes mellitus is a chronic metabolic syndrome defined by an inability to produce insulin, a hormone which lowers blood sugar. This leads to inappropriate hyperglycaemia (increased blood sugar levels) and deranged metabolism of carbohydrates, fats and proteins. Insulin is normally produced in the pancreas, a glandular organ involved in the production of digestive enzymes and hormones such as insulin and glucagon. These functions are carried out in the exocrine and endocrine (Islets of Langerhans) pancreas respectively. |
Statistics
Type 1 diabetes mellitus is predominantly a disease of the young, usually developing before 20 years of age. Overall, type I DM makes up approximately 15% of all cases of diabetes. It develops in approximately 1 in 600 children and is one of the most common chronic diseases in children. The incidence is relatively low for children under the age of 5, increases between 5 and 15, and then tapers off.
The incidence of diabetes (including type 1) appears to be rapidly rising in many parts of the world, including Australia. In addition, it may be occurring at an even younger age. Males and females tend to be equally affected.
In Australia there is estimated to be approximately one million diabetic patients, of which approximately 150,000 fit into the type 1 category. Australia has a very high rate of type 1 diabetes compared to the rest of the world. The incidence of diabetes in Australian Aboriginal people is even higher.
Risk Factors
Type I diabetes mellitus is a disease of disordered immune function involving destruction of the cells in the pancreas that secrete insulin (beta cells). The exact cause of the disease is unknown. It has been proposed that it arises from a genetically-linked autoimmune disease process. It is known that there is a strong family link.
The disease is thought to develop in five stages:
- Genetic predisposition
- Environmental trigger
- Active autoimmunity
- Progressive beta cell destruction
- Diabetes mellitus
For example, the environmental trigger may be a virus or chemical toxin that upsets the normal function of the immune system. This may lead to the body’s immune system attacking itself. The normal beta cells in the pancreas may be attacked and destroyed. When approximately 90% of the beta cells are destroyed, symptoms of diabetes mellitus begin to appear. The exact cause and sequence is not fully understood but investigation and research into the disease continues.
Genetic Predisposition
There is no single gene that “causes” type 1 diabetes. Instead, there are a large number of inherited factors that may increase an individual’s likelihood of developing diabetes. This is known as multifactorial inheritance. The genes implicated in the development of type 1 diabetes mellitus control the human leukocyte antigen (HLA) system. This system is involved in the complex process of identifying cells which are a normal part of the body, and distinguishing them from foreign cells, such as those of bacteria or viruses. In an autoimmune disease such as diabetes mellitus, this system makes a mistake in identifying the normal ‘self’ cells as ‘foreign’, and attacks the body.
Environmental Triggers
No single environmental trigger has been identified as causing diabetes mellitus, however both infectious agents and dietary factors are thought to be important. Various viruses have been implicated in the development of type I DM. They may act by initiating or modifying the autoimmune process. In particular, the rubella virus and coxsackie viruses have been closely studied. In particular, congenital rubella infection has shown direct relationships with the development of type 1 diabetes mellitus. This is presumably due to the virus (or antibodies against it) damaging the beta cells of the pancreas. Some research has looked at dietary factors that may be associated with type 1 diabetes. In particular, cow’s milk proteins (such as bovine serum albumin) which may have some similarities to pancreatic islet cell markers may be able to trigger the autoimmune process. Other chemicals including nitrosamines have been identified as causes of diabetes mellitus in animal models, but not in humans.
Progression
The development of type 1 diabetes mellitus can be said to pass through several ‘stages’. These include the pre-clinical stage, clinical presentation with symptoms, a period of relative remission (called the honeymoon period, characterised by improvement symptoms and even reduction in insulin dosage), and the chronic phase.
Pre-Clinical Phase
Pre-clinical diabetes refers to the time during which destruction of pancreatic insulin-producing cells is occurring, but symptoms have not yet developed. This period may last for months to years. Normally, 80-90% of the pancreatic beta cells must be destroyed before any symptoms of diabetes develops. During this time, blood tests can identify some immunological markers of pancreatic cell destruction. However, there is currently no known treatment to prevent progression of pre-clinical diabetes to true diabetes mellitus.
Clinical Presentation
The classic presenting symptoms of type 1 diabetes mellitus are discussed below. For some children, the first symptoms of diabetes mellitus are those of diabetic ketoacidosis. This is a serious and life-threatening condition, requiring immediate treatment. Ketoacidosis occurs due to a severe disturbance in the body’s metabolism. Without insulin, glucose cannot be taken up into cells. Instead fats are broken down for energy which can have acid by-products.
Honeymoon Stage
After a diagnosis of diabetes mellitus has been made, and treatment with insulin therapy has begun, a so-called ‘honeymoon stage’ may develop. This stage is characterised by a reduction in insulin requirements which may last from weeks to months. Some patients may require no insulin at all. This stage is always transient (short-lasting) and is due to production of insulin by the remaining surviving pancreatic beta cells. Eventually, these cells will be destroyed by the on-going auto-immune process, and the patient will be dependent on exogenous (artificial) insulin.
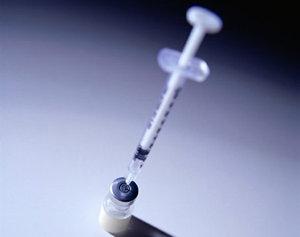
Chronic Phase
Patients with type 1 diabetes require life-long treatment with exogenous (artificial) insulin to regulate their blood sugar levels. This insulin may be given through the use of a hypodermic needle (seen right), or other methods such as the use of an insulin pump. Over time, many patients suffer chronic complications: vascular, neurological and organ-specific (such as kidney and eye disease). The frequency and severity of these complications is related to duration that the patient has suffered the disease for, and by how well their blood sugar levels have been controlled. If blood sugar levels, blood pressure and lipids are tightly controlled, many complications of diabetes may be prevented. Some patients may develop the major emergency complication of diabetes, known as ketoacidosis (extremely high blood glucose levels accompanied with extremely low insulin levels), which has a mortality rate of 5-10%.
Symptoms
The symptoms of type 1 diabetes mellitus usually develop rapidly and may include:
- Polyuria: increased frequency of urination, and particularly urination at night (nocturia).
- Polydipsia: increased thirst.
- Polyphagia: increased hunger.
- Fatigue or lethargy.
- Weight loss.
- Recurrent infections: for example, urinary tract infection or skin infection.
- Symptoms of ketoacidosis: drowsiness, rapid breathing, dehydration, abdominal pain, nausea and vomiting, decreased consciousness or coma.
Clinical Examination
Your doctor will carefully examine you at each visit for diabetes. In particular they will examine your cardiovascular system, eyes and neurological systems to detect any complications present. In the acute phase you may appear wasted and dehydrated. You may have difficulty breathing and have a sweet smell to your breath. In the later stages, your doctor will check your pulse, listen to your heart, measure your blood pressure (often lying and standing) and examine your limbs to detect any loss of sensation or ulcers.
How is it Diagnosed
- Blood glucose levels: persistently elevated blood sugar levels are diagnostic of diabetes mellitus. A specific test called a glucose tolerance test (GTT) may be performed. For this you need to be fasted and will be given a sugary drink. Your glucose level will then be measured at one and two hours after the doseto determine how welll your body copes with glucose.
- Urine: glycosuria (sugar in the urine) and ketonuria (ketones, a fat breakdown product) may be increased in diabetes mellitus.
- Urea and electrolytes: changes in these values may reflect possible dehydration.
Where difficulty with diagnosis is present, other investigations may include:
- Pancreatic islet cell autoantibody marker measurements: presence of islet cell autoantibodies is suggestive of type 1 DM.
- Glycosylated haemoglobin (HbA1c): this is an indirect measure of long-term blood sugar levels. It is usually expressed as a percentage (eg. 7%). It is used for monitoring of glycaemic (blood sugar) control.
Prognosis
Patients who suffer from diabetes have a lifelong struggle to attain and maintain blood glucose levels as close to the normal range as possible. With appropriate blood sugar control, the risk of both microvascular (small blood vessel) and neuropathic (nerve) complications is decreased markedly. Additionally, if hypertension (high blood pressure) and hyperlipidemia (high cholesterol) are treated promptly and aggressively, the risk of cardiovascular complications should decrease as well.
Treatment
Due to the dangers of diabetic ketoacidosis and high blood glucose levels, the initial management of type 1 diabetes mellitus may require hospitalisation to get blood sugar levels under control.
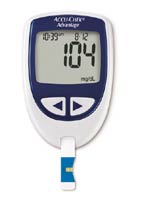
Longer-term, the goals of treatment are to prolong life, reduce symptoms, and prevent diabetes-related complications such as blindness, kidney failure, and amputation of limbs. These goals are accomplished through education, insulin use, meal planning and weight control, exercise, foot care, and careful self-testing of blood glucose levels. Self-testing of blood glucose is accomplished through regular use of a blood glucose monitor (pictured, right). This machine can quickly and easily measure the level of blood glucose based by analysing the level from a small drop of blood that is usually obtained from the tip of a finger. You will also require regular tests for glycated haemoglobin (HbA1c). This measures your overall control over several months.
Insulin
Replacement of insulin is essential in the treatment of type 1 diabetes mellitus. Numerous insulin types are available, and are chosen based on the patient’s lifestyle and blood glucose levels. Insulin is given as a subcutaneous (under the skin) injection several times throughout the day to attempt to stabilise blood glucose levels.
Education
Education about diabetes is essential, and is usually conducted by a diabetes educator in conjunction with a multidisciplinary diabetes management team. Important areas to cover include diet, exercise, blood glucose monitoring, medication regimes, and alterations in diabetes management with illness.
Other
Diabetes management involves controlling a whole lot of other risk factors:
- Reducing your blood pressure – The usual target is less than 130/80mmHg. This may be achieved by medications and dietary salt restrictions.
- Lowering cholesterol – Eating lots of oily fish can also help.
- Weight control – This is best achieved through diet and exercise. If you are very overweight you may also need special meal replacement programs, drugs or bariatric surgery to help you lose weight.
- Monitoring for complications – As well as seeing your diabetic educator you may need follow up with a podiatrist (foot doctor), ophthalmologist (eye doctor), renal physician and cardiologist to monitor and treat any complications from your disease.
References
- Braunwald, Fauci, Kasper, Hauser, Longo, Jameson. Harrison’s Principles of Internal Medicine. 16th Edition. McGraw-Hill. 2005.
- Bryant W, Greenfield J, Chisholm D, Campbell L. Diabetes guidelines: easier to preach than to practise? A retrospective audit of outpatient management of type 1 and type 2 diabetes mellitus, MJA 2006; 185 (6): 305-309.
- Cotran, Kumar, Collins 6th edition. Robbins Pathologic Basis of Disease. WB Saunders Company. 1999.
- Devendra D, Liu E, Eisenbarth G. Type 1 diabetes: recent developments, , BMJ 2004; 328: 750-754.
- Hurst JW (Editor-in-chief). Medicine for the practicing physician. 4th edition Appleton and Lange 1996.
- Hussain A, Vincent M. ‘Diabetes Mellitus, Type 1,’ eMedicine, 2005. Available [online] at URL: http://www.emedicine.com/med/topic546.htm
- Kumar P, Clark M. Clinical Medicine. WB Saunders 2002 Pg 427-430.
- Longmore M, Wilkinson I, Torok E. Oxford Handbook of Clinical Medicine. Oxford University Press. 2001.
- Murtagh J. General Practice. 3rd edition. McGraw-Hill. 2003.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.