- What is Psoriasis
- Statistics on Psoriasis
- Risk Factors for Psoriasis
- Progression of Psoriasis
- Symptoms of Psoriasis
- Clinical Examination of Psoriasis
- How is Psoriasis Diagnosed?
- Prognosis of Psoriasis
- How is Psoriasis Treated?
- Psoriasis References
What is Psoriasis
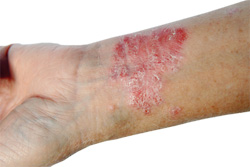
There are several different types of psoriasis – the most common, psoriasis vulgaris, accounts for 80–90% of all psoriasis cases. Psoriasis is associated with a range of other conditions, such as psoriatic arthritis, coronary artery disease and inflammatory bowel disease.
Psoriasis is a complex disease and much remains to be understood on how it develops. It is known that patches of psoriasis contain many abnormally activated immune cells within them. The most effective treatments for psoriasis are known to suppress immune cell activity. Research has established that certain inheritable genes predispose people to develop psoriasis.
 |
For more information about the subtypes of psoriasis and how they can be diagnosed, see Psoriasis Subtypes. |
Statistics on Psoriasis

Risk Factors for Psoriasis
Psoriasis probably occurs due to a combination of genetic and environmental factors. This includes stress, some types of infections and certain drugs (such as lithium and beta-blockers). Psoriasis is more common at higher than lower latitudes and is more common in Caucasians than other races.
Approximately 30% of people with psoriasis have an immediate family member who is also affected. Psoriasis vulgaris is more common in the immediate and extended family of individuals with the disease than in the general population. Children who have both parents and a sibling with psoriasis have an 83% chance of developing the disease.
Progression of Psoriasis
Relatively little is known regarding the progression of psoriasis, or factors that predict the severity of disease. As most cases of psoriasis commence during teenage years and early adulthood, the majority of individuals are affected for most of their lives. Psoriasis is called ‘early onset’ if it occurs before the age of 40.
It is thought that psoriasis will self-resolves in around a third of people. However, the disease can last for long periods, even up to 50 years. Of people with psoriasis vulgaris, 80% will have mild to moderate disease, while 20% have moderate to severe psoriasis (affecting more than 5% of the body surface area or affecting hands, feet, face, or genitals). If severe psoriasis is untreated, it tends to fluctuate in severity. Comparatively, mild to moderate psoriasis tends to wax and wane over time.
Psoriasis may take one of several forms and each has characteristic symptoms and potential severity. The types of psoriasis include psoriasis vulgaris, flexural/inverse psoriasis, guttate psoriasis, erythrodermic psoriasis, generalised pustular psoriasis, palmoplantar psoriasis, scalp psoriasis and nail psoriasis.
Psoriasis vulgaris (plaque psoriasis)
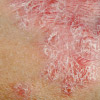
Psoriasis vulgaris (also known as chronic plaque psoriasis) is characterised by raised, rough plaques with surrounding normal skin. It is the most common form of psoriasis, affecting 80–90% of individuals. The plaques can be salmon-pink or red and are generally distributed symmetrically on the body. They are covered with white or silvery scales.
Flexural psoriasis (inverse psoriasis)
Flexural (inverse) psoriasis is a rare form of psoriasis that occurs in areas where two layers of skin come together, such as the groin, armpits, buttocks and below the breast. Flexural psoriasis appears as shiny red plaques that are not covered with scales, this is due to the moist areas in which they occur.
Guttate psoriasis
Guttate psoriasis generally affects children and young adults. Sufferers develop small salmon-pink, teardrop-shaped bumps (less than 1 cm in diameter) and are usually covered with a fine scale. This generally occurs on the trunk and upper arms and legs. It occurs approximately 2 to 3 weeks following a viral or bacterial upper airway infection, such as tonsillitis.
Erythrodermic psoriasis
Erythroderma is a rare, potentially life-threatening form of psoriasis. The skin becomes bright red and inflamed, with variable degrees of scale. Over 75% of the body surface is affected which can lead to fever, chills, fatigue, hypothermia, heart failure and infection.
Generalised pustular psoriasis
Generalised pustular psoriasis is another rare, serious form of psoriasis. Sufferers develop fevers and chills and pustules form all over the body. Small pustules can form in acutely painful, inflamed skin all over the body. It is caused by infections, medications (such as corticosteroids) or pregnancy.
Palmoplantar psoriasis
In palmoplantar pustulosis, painful, itchy yellow-brown pustules form on the palms of the hands and soles of the feet. These pustules are typically 2–5 mm in diameter, yellow and evolve into a dusky-red, crusted, bumpy rash.
Scalp psoriasis
Scalp psoriasis is common in people with chronic plaque psoriasis, usually within the hairline but the entire scalp can be affected. Plaques are typically covered with thick white or silvery scales, however it does not cause hair loss.
Nail psoriasis
Around half of all people with psoriasis have fingernail changes associated with the disease, while 35% have toenail changes. The most common nail change is the formation of small pits within the nail. Other changes can include separation of the nail plate, dots of yellow-orange discolorations within the nail or breakdown of the entire nail.
 |
For more information about the subtypes of psoriasis and how their macroscopic features, see Psoriasis Subtypes. |
Symptoms of Psoriasis
People with psoriasis may find they are less productive, have altered moods (depression or anxiety) and experience difficulties with social interaction. It is important to tell your doctor about the severity of these symptoms, as this will help determine the intensity of treatment and allow for provision of adequate support.
People have different responses to treatments, so the effectiveness and side effects of previous treatments plays an important role in guiding current and future treatment options.
Clinical Examination of Psoriasis
The diagnosis of psoriasis is based on the appearance of the psoriasis-affected skin. Characteristic nail changes and classical distribution of plaques are also strongly suggestive of psoriasis. A doctor’s examination of a person with psoriasis aims to determine the severity of disease:
- Mild psoriasis is defined as affecting less than 10% of the body’s surface area;
- Moderate psoriasis affects more than 10%, or less than 10% in difficult areas; and
- Severe disease affects more than 20%.
Clinicians use a specific method to assess severity of psoriasis, called the Psoriasis Area and Severity Index (PASI). Moderate to severe disease is defined as a PASI score greater than 10. The PASI is also used to determine if individuals are responding to treatment over time.
The effect of psoriasis on a person’s quality of life needs to be considered when assessing the severity of disease. For example, mild psoriasis on the palms and soles may have a significant impact on day-to-day life and may require different medications. Doctors also examine psoriasis sufferers for evidence of an infection, which can cause other problems for people with psoriasis.
Some other conditions that can have a similar appearance to psoriasis are:
- Nummular eczema;
- Tinea;
- Cutaneous lupus;
- Pityriasis rosea (may resemble guttate psoriasis);
- Mycosis fungoides; and
- Intertrigo or candidiasis/thrush.
How is Psoriasis Diagnosed?
Special tests for psoriasis are generally not required. Diagnosing psoriasis and determining the severity of disease is based almost entirely on clinical examination. Occasionally, biopsies can be taken from a psoriasis plaque to confirm the diagnosis.
Prognosis of Psoriasis
Psoriasis is known to have a significant impact on quality of life that may result in profound affects on mental health and reduced participation in employment. There is an increased overall risk of death in individuals with severe psoriasis.
Psoriasis is associated with several diseases, including:
- Cardiovascular disease: There is an increased risk of cardiovascular disease in individuals with moderate or severe psoriasis. This is thought to be due to increased immune system activation due to psoriasis. Individuals with psoriasis are also frequently overweight and have higher rates of diabetes and high blood pressure. There does not appear to be an increased risk of cardiovascular disease in individuals who have only mild psoriasis;
- Metabolic syndrome: Metabolic syndrome is more common in individuals admitted to hospital with psoriasis than in hospitalised people who do not have psoriasis;
- Cancer: Skin cancer is more common in people with psoriasis. It is unclear whether the link between psoriasis and cancer is due to the treatment of psoriasis or the condition itself. There is a controversial link between lymphoma and psoriasis;
- Depression: Up to 60% of individuals with psoriasis may have depression and 5% reported active suicidal ideation; and
- Other diseases such as diabetes and Crohn’s disease.
How is Psoriasis Treated?
Treatment considerations

The management of psoriasis is tailored to suit each individual. The extent and location of the psoriasis, as well as other illnesses, quality of life, triggering factors and ability to use different treatments can affect the selection of medications.
As a chronic condition that can affect your quality of life, your doctor will provide you with education on aspects of the illness, such as:
- Exacerbating factors, including stress, other medications, excessive alcohol and tobacco use;
- Maintaining skin hydration; and
- A long-term approach to treatment, including likely prognosis, cost/benefit of treatments, future life events (e.g. pregnancy) and the possible effect of psoriasis on quality-of-life.
Topical therapy
Topical therapies (treatments applied to the surface of the area they are intended to treat) can be applied directly to psoriasis as creams or ointments and are generally safe. They are the best approach in treating psoriasis over smaller areas and they can also reduce the need for, or dose of, other medications.
Topical corticosteroids
Topical corticosteroids suppress immune system activity. They are the first choice for plaque, scalp or intertriginous psoriasis and are available in varying strengths. Lower strength steroids are reserved for the face, thin-skinned areas and on children. They are often used in combination with other topical therapies, phototherapy or oral medications.
Topical corticosteroids do have some side effects, such as acne, skin infections or dermatitis. They can also exacerbate other underlying skin conditions if used for long periods of time. More serious side effects are very rare. If individuals are using strong doses, very frequent application and/or over a large surface area, side effects are more likely.
Vitamin D analogues
The vitamin D analogues (substances that are similar in structure to vitamin D) include calcipotriene, calcipotriol (e.g. Daivonex, Daivobet) and calcitriol. They slow down the overgrowth of skin tissue characteristic of psoriasis. These drugs take longer to work than topical corticosteroids but tend to be effective for longer periods. The use of corticosteroids with vitamin D analogue therapy is more effective than using either treatment alone. Skin irritation is the most common side effect, affecting up to 35% of people.
Tazarotene
Tazarotene (e.g. Zorac) is a topical retinoid that decreases skin overgrowth and inflammation. Tazarotene is often used in combination with topical corticosteroids. Skin irritation and heightened sensitivity to sunlight are possible side effects.
Dithranol
Dithranol (also known as anthralin) was a common treatment for psoriasis, but it is used less commonly as it can stain skin and clothing. Dithranol is an effective treatment that can be used in combination with phototherapy, topical corticosteroids or calcipotriol.
Calcineurin inhibitors
Calcineurin inhibitors such as tacrolimus (e.g. Prograf, Tacrolimus Sandoz) and pimecrolimus (e.g. Elidel) stop the production of inflammatory chemicals that cause psoriasis to evolve. They are generally only used for facial or intertriginous psoriasis. They can, however, cause burning and itching, but this generally reduces with ongoing use.
Salicylic acid

Emollients
Emollients increase skin hydration and are used in combination with other psoriasis treatments. They can reduce the mount of scale and decrease itchiness of psoriasis and they have minimal side effects.
Coal tar
Coal tar has been used as a treatment for psoriasis for many decades. It is available as solutions, shampoos and ointments. It can also be used as combination with phototherapy. However, individuals using coal tar often complain of skin irritation, skin infections, staining of clothing and an unpleasant smell.
Phototherapy
Phototherapy is a commonly used treatment for psoriasis, where the skin is exposed to ultraviolet (UV) light to inhibit skin overgrowth. Phototherapy is effective in younger people with thin psoriasis and in individuals who say sunlight improves their symptoms. Phototherapy uses narrow band UV-B light as it is more effective than other types. Moderate psoriasis is generally cleared after 6 weeks of phototherapy three times a week. This can give 3 to 6 months of symptom relief.
Phototherapy can have side effects. This includes skin redness, itchiness, burning and stinging of the skin. The skin can also age prematurely. However, there is no evidence of increased risk of skin cancer. Using new lasers, phototherapy can now be targeted specifically on psoriasis-affected areas, while leaving unaffected skin untreated.
PUVA photochemotherapy

Common side effects of PUVA treatment include skin redness, itchiness, pigmentation of the skin and nausea and vomiting. With long-term PUVA therapy, most individuals will have skin aging and there is an increased risk of cataracts.
Systemic therapy
Systemic therapies are medications that are taken orally and circulate around the entire body. These drugs are used in individuals with psoriasis that is not controlled by topical agents or phototherapy, but they carry a higher risk of side effects.
Cyclosporin
Cyclosporin inhibits the activity of immune cells. It is used in palmoplantar pustulosis, erythrodermic and nail psoriasis. It is a safe treatment to use in women who are trying to fall pregnant. Cyclosporin works quickly and can stop the symptoms of psoriasis for long periods. The major side effects are high blood pressure and kidney toxicity. Cyclosporin can only be used for 1 to 2 years. Cyclosporin may also be a good treatment option for people with hepatitis C infection.
Methotrexate
Methotrexate is the most used treatment for moderate to severe psoriasis. Methotrexate is generally well tolerated and can be used long-term. However, it is not safe to be used during pregnancy or for women who are trying to fall pregnant. Men taking methotrexate should avoid conceiving while taking the drug. Men should also take folic acid supplements while on methotrexate. Because methotrexate is associated with liver disease, extra consideration should be given to cases where alcohol use disorder is present.
Acitretin
Acitretin (e.g. Neotigason, Acitretin Actavis) is a medication that inhibits immune dysfunction causing psoriasis. It takes 3 to 6 months to reach maximum effect. It can be combined with other topical treatments (corticosteroids or vitamin D analogues). Individuals may experience side effects such as conjunctivitis, hair loss, skin dryness, nail fragility, high cholesterol and osteoporosis.
Biologic agents

These medications are:
- TNF-alpha antagonists – etanercept (e.g. Enbrel), adalimumab (e.g. Humira) and infliximab (e.g. Remicade);
- T cell modulators – alefacept and efalizumab (neither is currently available in Australia);
- IL-12/IL-23 inhibitors – ustekinumab (e.g. Stelara).
TNF alpha antagonists
These drugs bind and inactivate the inflammatory chemicals that cause psoriasis to progress. They are given intravenously; however, 24% of people experience a reaction at the injection site. Over 20% of individuals experience side effects during the injection, such as chills, headache, flushing and dyspnoea.
T cell modulators
Alefacept and efalizumab target immune cells critical to the development of psoriasis. However, neither is available in Australia. These drugs are generally less effective than other biological agents and require careful monitoring of white cell counts. The main side effects are fatigue and joint pain, which occurs in approximately 20% of people treated with alefacept.
IL-12/IL-23 inhibitors
Ustekinumab is a drug that binds and inactivates two chemicals (IL-12 and IL-23) that stimulate the development of moderate to severe psoriasis. Ustekinumab has very few side effects and injection site reactions are uncommon. It is currently available in Australia.
 |
For more information about the treatment of psoriasis, see Psoriasis Treatment. |
Psoriasis References
- GriffithsCE, Barker JN. Pathogenesis and clinical features of psoriasis. Lancet. 2007; 370(9583): 263-71. [Abstract]
- Pathirana D, Ormerod AD, Saiag P, et al. European S3-guidelines on the systemic treatment of psoriasis vulgaris. J Eur Acad Dermatol Venereol. 2009; 23 Suppl 2:1-70. [Abstract | Full text]
- Rapp SR, Feldman SR, Exum ML, et al. Psoriasis causes as much disability as other major medical diseases. J Am Acad Dermatol. 1999;41(3 Pt 1): 401-7. [Abstract]
- Gaspari AA. Innate and adaptive immunity and the pathophysiology of psoriasis. J Am Acad Dermatol. 2006; 54(3 Suppl 2): S67-80. [Abstract]
- Cumberbatch M, Singh M, Dearman RJ, et al. Impaired Langerhans cell migration in psoriasis. J Exp Med. 2006; 203(4): 953-60. [Abstract | Full text]
- Allen MH, Ameen H, Veal C, et al. The major psoriasis susceptibility locus PSORS1 is not a risk factor for late-onset psoriasis. J Invest Dermatol. 2005; 124(1): 103-6. [Abstract | Full text]
- Swanbeck G, Inerot A, Martinsson T, et al. Genetic counselling in psoriasis: empirical data on psoriasis among first-degree relatives of 3095 psoriatic probands. Br J Dermatol. 1997; 137(6): 939-42. [Abstract]
- Huerta C, Rivero E, Rodríguez LA.Incidence and risk factors for psoriasis in the general population. Arch Dermatol. 2007; 143(12): 1559-65. [Abstract]
- GriffithsCEM, CampRDR, Barker JNWN. Psoriasis. In: Burns T, Breathnach S, CoxNH, Griffiths C (eds). Rook’s Textbook of Dermatology (7th edition). Oxford: Blackwell Science; 2005: 35.1-35.69. [Publisher]
- Mason AR, Mason J, Cork M, et al. Topical treatments for chronic plaque psoriasis. Cochrane Database Syst Rev. 2009; 2: CD005028. [Abstract | Full Text]
- Medansky RS, CuffieCA, Tanner DJ. Mometasone furoate 0.1%-salicylic acid 5% ointment twice daily versus fluocinonide 0.05% ointment twice daily in the management of patients with psoriasis. Clin Ther. 1997; 19(4): 701-9. [Abstract]
- Koo J, CuffieCA, Tanner DJ, et al. Mometasone furoate 0.1%-salicylic acid 5% ointment versus mometasone furoate 0.1% ointment in the treatment of moderate-to-severe psoriasis: a multicenter study. Clin Ther. 1998; 20(2): 283-91. [Abstract]
- Menter A, Gottlieb A, Feldman SR, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: Section 1. Overview of psoriasis and guidelines of care for the treatment of psoriasis with biologics. J Am Acad Dermatol. 2008; 58(5): 826-50. [Abstract]
- Australian Medicines Handbook. Dermatological drugs[online]. AMH 2012 [cited 20th June 2012]. Available from: URL link
- Christensen TE, Callis KP, Papenfuss J, et al. Observations of psoriasis in the absence of therapeutic intervention identifies two unappreciated morphologic variants, thin-plaque and thick-plaque psoriasis, and their associated phenotypes. J Invest Dermatol. 2006; 126(11): 2397-403. [Abstract | Full text]
- Lebwohl M. Psoriasis. Lancet. 2003; 361(9364): 1197-204. [Abstract]
- Farber EM, Nall ML. The natural history of psoriasis in 5,600 patients. Dermatologica. 1974; 148(1): 1-18. [Abstract]
- Wang G, Chunying L, Tianwen G et al. Clinical analysis of 48 cases of inverse psoriasis: a hospital based study. European Journal of Dermatology. 2005; 15: 176-178. [Abstract | Full Text]
- Chalmers R, O’Sullivan T, Owen C. A systematic review of treatments for guttate psoriasis. Br J Dermatology. 2001; 145: 891-894. [Abstract]
- Rosenbach M, Hsu S, Korman N, et al. Treatment of erythrodermic psoriasis: From the medical board of the National Psoriasis Foundation. J Am Acad Dermatol. 2010; 62: 655-662. [Abstract]
- Iizuka H, Takahashi H, Ishida-Yamamoto. Pathophysiology of generalised pustular psoriasis. Archives of Dermatological Research. 2003; 295: S55-S59. [Abstract]
- Wolff K, Johnson R. Fitzpatrick’s Colour Atlas and Synopsis of Clinical Dermatology (6th edition). New York: McGraw Hill Medical; 2009. [Publisher]
- Sullivan J, Preda V. Treatments for severe psoriasis. Aust Prescr. 2009; 32: 14-8. [Full text]
- Martin BA, Chalmers RJG, Telfer NR. How great is the risk of further psoriasis following a single episode of a guttate psoriasis? Arch Dermatol. 1996; 132(6): 717-8. [Abstract]
- Finlay AY, Coles EC. The effect of severe psoriasis on the quality of life of 369 patients. Br J Dermatol. 1995; 132(2): 236-44. [Abstract]
- Richards HL, Fortune DG, GriffithsCE. Adherence to treatment in patients with psoriasis. J Eur Acad Dermatol Venereol. 2006; 20(4): 370-9. [Abstract]
- Fortune DG, Richards HL, Kirby B, et al. Psychological distress impairs clearance of psoriasis in patients treated with photochemotherapy. Arch Dermatol. 2003; 139(6): 752-6. [Full text]
- Menter A, Griffiths C. Current and future management of psoriasis. Lancet. 2007; 370(9583): 272-84. [Abstract]
- Naldi L. Scoring and monitoring the severity of psoriasis. What is the preferred method? What is the ideal method? Is PASI passé? Facts and controversies. Clin Dermatol. 2010; 28(1): 67-72. [Abstract]
- Horn EJ, Fox KM, Patel V, et al. Association of patient-reported psoriasis severity with income and employment. J Am Acad Dermatol. 2007; 57(6): 963-71. [Abstract]
- Finlay AY, Kelly SE. Psoriasis: An index of disability. Clin Exp Dermatol. 1987; 12(1): 8-11. [Abstract]
- Gelfand JM, TroxelAB, Lewis JD, et al. The risk of mortality in patients with psoriasis: Results from a population-based study. Arch Dermatol. 2007; 143(12): 1493-9. [Abstract]
- Mallbris L, Akre O, Granath F, et al. Increased risk for cardiovascular mortality in psoriasis inpatients but not in outpatients. Eur J Epidemiol. 2004; 19(3): 225-30. [Abstract]
- Neimann AL, Shin DB, Wang X, et al. Prevalence of cardiovascular risk factors in patients with psoriasis. J Am Acad Dermatol. 2006 Nov; 55(5): 829-35. [Abstract]
- Gelfand JM, Neimann AL, Shin DB, et al. Risk of myocardial infarction in patients with psoriasis. JAMA. 2006; 296(14): 1735-41. [Abstract | Full text]
- Sommer DM, Jenisch S, Suchan M, et al. Increased prevalence of the metabolic syndrome in patients with moderate to severe psoriasis. Arch Dermatol Res. 2006; 298(7): 321-8. [Abstract]
- Gelfand JM, Shin DB, Neimann AL, et al. The risk of lymphoma in patients with psoriasis. J Invest Dermatol. 2006; 126(10): 2194-201. [Abstract | Full text]
- Margolis D, Bilker W, Hennessy S, et al. The risk of malignancy associated with psoriasis. Arch Dermatol. 2001; 137(6): 778-83. [Abstract | Full text]
- Stern RS, Lunder EJ. Risk of squamous cell carcinoma and methoxsalen (psoralen) and UV-A radiation (PUVA): A metaanalysis. Arch Dermatol. 1998; 134(12): 1582-5. [Abstract | Full text]
- Kimball AB, Gordon KB, Fakharzadeh S, et al. Long-term efficacy of ustekinumab in patients with moderate-to-severe psoriasis: results from the PHOENIX 1 trial through up to 3 years. Br J Dermatol. 2012; 166(4): 861-72. [Abstract]
- Esposito M, Saraceno R, Giunta A, et al. An Italian study on psoriasis and depression. Dermatology. 2006; 212(2): 123-7. [Abstract]
- Gupta MA, Gupta AK. Depression and suicidal ideation in dermatology patients with acne, alopecia areata, atopic dermatitis and psoriasis. Br J Dermatol. 1998; 139(5): 846-50. [Abstract]
- Henseler T, Christophers E. Disease concomitance in psoriasis. J Am Acad Dermatol. 1995; 32(6): 982-6. [Abstract]
- Dediol I, Buljan M, Buljan D, et al. Associations of psoriasis and alcoholism: psychodermatological issues. Psychiatria Danube. 2009; 21(1): 9-13. [Abstract | Full Text]
- Menter A, Korman A, Elmets C, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 3: Guidelines of care for the management of psoriasis with topical therapies. Academy of Dermatology. 2009; 60: 643-659. [Abstract]
- McGill A, Frank A, Emmett N, et al. The anti-psoriatic drug anthralin accumulates in keratinocyte mitochondria, dissipates mitochondrial membrane potential, and induces apoptosis through a pathway dependent on respiratory competent mitochondria. FASEB J. 2005; 19(8): 1012-4. [Full text]
- Therapeutic Guidelines. Psoriasis. Revised February 2009. Available from: URL link
- Swinkels OQ, Prins M, Kucharekova M, et al. Combining lesional short-contact dithranol therapy of psoriasis with a potent topical corticosteroid. Br J Dermatol. 2002; 146(4): 621-6. [Abstract]
- Monastirli A, Georgiou S, Pasmatzi E, et al. Calcipotriol plus short-contact dithranol: A novel topical combination therapy for chronic plaque psoriasis. Skin Pharmacol Appl Skin Physiol. 2002; 15(4): 246-51. [Abstract]
- Green L. An overview and update on psoriasis. Nursing Standard. 2011 (25): 47-55. [Abstract]
- Menter A, Korman A, Elmets C, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 5: Guidelines of care for the management of psoriasis with phototherapy and photochemotherapy. J Am Acad Dermatol. 2010; 62: 114-135. [Abstract]
- Herrier R. Advances in the treatment of moderate to severe plaque psoriasis. Am J Health-Syst Pharm. 2011; 68: 795-806. [Abstract]
- Lapolla W, Yentzner B, Bagel J, et al. A review of phototherapy protocols for psoriasis treatment. J Am Acad Dermatol. 2011; 64: 936-949. [Abstract]
- Menter A, Korman A, Elmets C, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 6: Guidelines of care for the treatment of psoriasis and psoriatic arthritis: case-based presentations and evidence based conclusions. J Am Acad Dermatol. 2011; 65: 137-174. [Abstract]
- Paul C, Gallini A, Maza A, et al. Evidence-based recommendations on conventional systemic treatments in psoriasis: systematic review and expert opinion of a panel of dermatologists. J Euro Acad Dermatol Venereol. 2011; 25: 2-11. [Abstract]
- Maza A, Montaudie H, Sbidian E, et al. Oral cyclosporin in psoriasis: a systematic review on treatment modalities, risk of kidney toxicity and evidence for use in non-plaque psoriasis. J Euro Acad Dermatol Venereol. 2011; 25: 19-27. [Abstract]
- Montaudie H, Sbidian E, Paul C, et al. Methotrexate in psoriasis: a systematic review of treatment modalities, incidence, risk factors and monitoring of liver toxicity. J Euro Acad Dermatol Venereol. 2011; 25: 12-18. [Abstract]
- Garcia-Valladares, Cuchacovich R, Espinoza L. Comparative assessment of biologics in treatment of psoriasis: drug design and clinical effectiveness of ustekinumab. Drug Des Develop Therapy. 2011; 5: 41-49. [Abstract | Full Text]
- Weger W. Current status and new developments in the treatment of psoriasis and psoriatic arthritis with biological agents. Br J Pharmaco. 2010; 160: 810-820. [Abstract | Full Text]
- Foulkes AC, Grindlay DJC, Griffiths CEM, et al. What’s new in psoriasis? An analysis of guidelines and systematic reviews published in 2009-10. Clin Experimental Dermatol. 2011; 36: 585-9. [Abstract | Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







