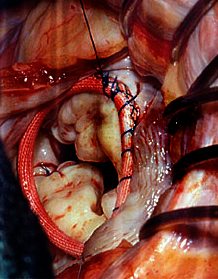
- What is Mitral Regurgitation (MR)
- Statistics on Mitral Regurgitation (MR)
- Risk Factors for Mitral Regurgitation (MR)
- Progression of Mitral Regurgitation (MR)
- Symptoms of Mitral Regurgitation (MR)
- Clinical Examination of Mitral Regurgitation (MR)
- How is Mitral Regurgitation (MR) Diagnosed?
- Prognosis of Mitral Regurgitation (MR)
- How is Mitral Regurgitation (MR) Treated?
- Mitral Regurgitation (MR) References
What is Mitral Regurgitation (MR)
Acute mitral regurgitation is a disorder in which the heart’s mitral valve (between the left aftrium and left ventricle) does not close properly, causing blood to leak (back-flow) into the left atrium (upper heart chamber) when the left ventricle (lower heart chamber) contracts.
Statistics on Mitral Regurgitation (MR)
Mitral valve prolapse which can cause regurgitation is the most common form of valvular heart disease and occurs in 3-8% of the population. 50% of cases of mitral regurgitation are due to rheumatic heart disease. The current rate of rheumatic fever in the developed world is 0.01%, although this is higher in the Middle and Far East, South America and Indigenous Aboriginal populations of Australia.
Risk Factors for Mitral Regurgitation (MR)
The main causes of MR are mitral valve prolapse in which one of the leaflets of the mitral valve bulges up into the left atrium during systole, and acute rheumatic fever.
However any disease process which causes dilatation of the left ventricle can also induce regurgitation:
- Aortic valvular disease (especially aortic regurgitation).
- Dilated cardiomyopathy.
- Ischaemic heart disease and myocardial infarction.
Other disease which can produce MR by mechanisms other than dilatation of the left ventricle include:
- Infective endocarditis (destruction of the valve leaflets).
- Hypertrophic cardiomyopathy (disorganization of ventricular contraction).
- Connective tissue disorders (eg. SLE).
- Degenerative valve changes.
- Rupture of the chordae tendineae (causing acute MR).
Obviously, factors which predispose to these diseases will also predispose to MR. Usual risk factors for ischaemic heart disease (age, hypertension, smoking, diabetes mellitus and hyperlipidaemia) will also increase the risk of developing MR.
Progression of Mitral Regurgitation (MR)
The disease follows two distinct natural histories depending on whether it is acute or chronic.
Chronic regurgitation back into the left atrium causes the atrium to dilate to accommodate the extra blood. The ventricle also dilates to increase volume of blood pumped out and maintain the cardiac output (compensatory changes).
Eventually, heart failure, arrhythmias and pulmonary oedema occur. Late in the disease right heart failure may also occur, secondary to left heart failure and pulmonary hypertension.
How is Mitral Regurgitation (MR) Diagnosed?
Chest x-ray shows left atrial and left ventricular enlargement and may show valve calcification and evidence of pulmonary oedema.
ECG may show abnormalities in keeping with the heart enlarging, as well as atrial fibrillation if present.
Prognosis of Mitral Regurgitation (MR)
MR follows a chronic course of compensation and decompensation, the end result of which is heart failure which has a very poor prognosis. However, the natural history of the disease often does not reach this point due to potential surgical interventions. Mortality is MR is also attributable to complications such as embolic (clots forming in the heart and travelling to other organs) events and infective endocarditis. Some studies have shown an 80% 5 year survival rate for MR patients.
How is Mitral Regurgitation (MR) Treated?
Early in the natural history, management is conservative with monitoring via regular echocardiogram studies. Prophylaxis against infective endocarditis is given and any related problems (eg. atrial fibrillation) are treated.
Progression of the disease is an indication for early surgical intervention, either by mitral valve repair, or mitral valve replacement. Late disease in patients who are not suitable for surgery requires standard heart failure management with ACE inhibitors, diuretics and beta-blockers and possibly anticoagulation.
Mitral Regurgitation (MR) References
- Hurst’s The Heart 8th Edition, McGRAW-HILL 1994.
- Kumar and Clark Clinical Medicine 4th Edition, W.B SAUNDERS 1998.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.