- What is Pulmonary oedema
- Statistics on Pulmonary oedema
- Risk Factors for Pulmonary oedema
- Progression of Pulmonary oedema
- Symptoms of Pulmonary oedema
- Clinical Examination of Pulmonary oedema
- How is Pulmonary oedema Diagnosed?
- Prognosis of Pulmonary oedema
- How is Pulmonary oedema Treated?
- Pulmonary oedema References
What is Pulmonary oedema
Pulmonary oedema is a disease of the lung.
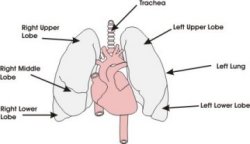
The lungs essentially provide the interface between air and blood. The lungs consist of a series of folded membranes (the alveoli), which are located at the ends of very fine branching air passages (bronchioles). Blood which arrives into the lungs from the pulmonary artery gets into smaller and smaller blood vessels until it ends up in the capillaries located within the walls of the alveoli, which is a very thin membrane. In this moist environment, oxygen diffuses from within the alveoli into the blood stream, while carbon dioxide moves out of the blood stream into the alveoli and is expelled out of the air passages.
Pulmonary oedema is the accumulation of fluid in the alveoli of the lungs. This fluid moves from blood vessels, across capillary and alveolar membranes, into the alveoli, causing symptoms such as shortness of breath. Which alveoli are affected depends on the cause and severity of pulmonary oedema: early pulmonary oedema due to heart failure affects the bases of the lungs, whereas severe adult respiratory distress syndrome involves oedema throughout the lung.
Statistics on Pulmonary oedema
Pulmonary oedema is a very common condition, mainly due left sided heart failure. With an ageing population and incresing numbers of patients surviving acute myocardial infarcts (heart attacks) there is a growing number of patients presenting with pulmonary oedema.
Heart failure is the most common cause of admission to hospital in the Medicare population in the United States, and almost a million patients (978,000) were admitted in the US with the diagnosis of pulmonary oedema in 1998. Other Western countries such as Australia and the UK have a similarly high incidence.
Risk Factors for Pulmonary oedema
Movement of fluid from blood vessels into air spaces occurs due to either:
- increased pressure in pulmonary veins – mostly due to
heart failure. - reduced protein in the blood – usually due to liver or kidney disease, or
- increased capillary permeability (leaky blood vessels) – see ARDS.
Progression of Pulmonary oedema
Congestive heart failure is the most common cause of pulmonary oedema. This causes blood to “back up” in the pulmonary veins. Initially fluid is pushed out of the vessels and into the surrounding tissue (interstitial oedema). Further increase in pressure causes fluid to move into the alveolar spaces, resulting in “alveolar oedema”. If this is present for a long time, further changes occur, impairing normal lung function, and predisposing to infection.
Pulmonary oedema due to other causes tends to be more short-lived, except for the cases that progress to adult respiratory distress syndrome.
How is Pulmonary oedema Diagnosed?
Chest x-ray: This is the most useful investigation in the diagnosis of pulmonary oedema. It can also suggest how severe the pulmonary oedema.
Prognosis of Pulmonary oedema
Admission to hospital for decompensated heart failure – or acute pulmonary oedema is associated with significan morbidity and mortality. A high proportion of patients are at risk of dying or a re-admission after one admission for pulmonary oedema.
The prognosis of course varies with severity. Causes other than heart failure have a differing prognosis.
How is Pulmonary oedema Treated?
Acute (emergency) treatment:
- The patient is placed in the sitting position, and
- High concentration oxygen administered via mask.
- CPAP is often helpful. Artificial ventilation is required in severe cases.
- Diuretic (frusemide) treatment is given intravenously, this is effective immediately through actions on the blood vessels, as well as in the longer term through the excretion of fluids.
- Morphine, together with an antiemetic (to prevent nausea/vomiting side effects of morphine) is given. Morphine helps to sedate the patient, and treats the oedema through dilatation of blood vessels outside the lung.
- GTN, which dilates veins, may be given. Hydralazine may be given in order to increase the output of the heart.
- Treatment of pulmonary oedema due to other causes, and long term treatment due to any cause, must address the underlying disease.
* Note that the above treatment focuses mainly on pulmonary oedema due to heart failure, as this is the most common cause of acute pulmonary oedema.
Pulmonary oedema References
[1] Felker GM. Adams KF Jr. Konstam MA. O’Connor CM. Gheorghiade M.The problem of decompensated heart failure: nomenclature, classification, and risk stratification. American Heart Journal. 145(2 Suppl):S18-25, 2003 Feb.
[2] Kumar P, Clark M. Clinical Medicine. Fourth Ed. WB Saunders, 1998. pp683-684
[3] Poole-Wilson PA. Xue SR. New therapies for the management of acute heart failure. Current Cardiology Reports. 5(3):229-36, 2003 May.
[4] Talley NJ, O’Connor S. Clinical examination. Third Ed. MacClennan & Petty, 1996. 65.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.