- What is Ectopic Pregnancy?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- References
What is Ectopic Pregnancy?
Ectopic pregnancy (sometimes referred to as extrauterine pregnancy) refers to a pregnancy which grows outside of the uterus (where pregnancy usually occurs). It occurs when a fertilised egg fails to implant in the endometrial tissues of the uterine cavity and instead leaves the uterus and implants at another site. The most common sites for such pregnancies are the:
|
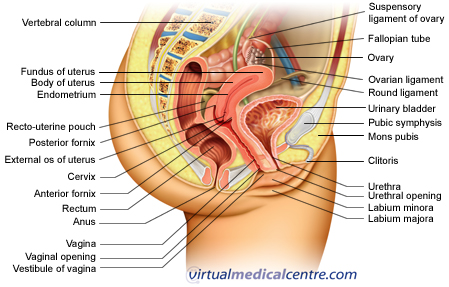
Left untreated, ectopic pregnancy is a life threatening condition. It is the leading cause of death in the first trimester of pregnancy and the fourth leading cause of all maternal deaths in the United Kingdom. Ectopic pregnancy is also a leading cause of early pregnancy death in Australia. In the 2003-05 period, there were two women who died directly as a result of pregnancy in the first trimester and one of these deaths was caused by an ectopic pregnancy.
Statistics
Women of childbearing age are at risk of ectopic pregnancy and is estimated that 2% of all pregnancies are ectopic. While incidence is now stable or declining in many developing countries, it increased markedly 1970-1990 and remains well above 1970s levels today. For example in England ectopic pregnancies occurred at a rate of 3.45 per 1000 live births in 1966. In 1996 the rate had increased to 15.5 per 1000 live births.
In Australia the incidence of ectopic pregnancy decreased slightly in the 1990s, from a rate of 17.4 per 1000 births in 1990 to 16.2 per 1000 in 1998.
Increasing incidence is in part due to improvements in the way ectopic pregnancy is diagnosed (e.g. ultrasound, which is the usual way to diagnose ectopic pregnancy today, was much less accessible several decades ago). Other factors thought to play a role in the changing incidence of ectopic pregnancy include changes in smoking patterns in women and increased incidence of pelvic inflammatory disease (PID) and chlamydia trachomatis, a sexually transmitted infection (STI).
Risk Factors

- Smoking: A French study reported that cigarette smoking accounted for 35% of the risk associated with ectopic pregnancy. The more a woman smokes, the more likely she is to develop an ectopic pregnancy. Women who smoke more than 20 cigarettes per day are almost four times more likely to experience an ectopic pregnancy than those who have never smoked. Women who smoke less than 10 cigarettes per day are less than 2 times more likely to develop ectopic pregnancy than those who never smoked;
- Previous ectopic pregnancy: Women who have had one ectopic pregnancy in the past are about seven times more likely to develop an ectopic pregnancy in the future than women who have never had an ectopic pregnancy. Women who have had two or more ectopic pregnancies in the past are over 70 times more likely to develop an ectopic pregnancy in the future;
- Previous miscarriage: The risk of ectopic pregnancy increases with the number of miscarriages a woman has previously experienced. Women who have experienced 1-2 miscarriages in the past are 1.2 times more likely to develop an ectopic pregnancy than women who have never miscarried. Three or more miscarriages in the past increases the risk of developing an ectopic pregnancy to three times that of women who have never had a miscarriage;
- Previous medically induced abortion: Women who have medically terminated a pregnancy are 2.8 times more likely to experience ectopic pregnancy than those who had never induced abortion. There is no increased risk associated with a history of induced surgical abortion;
- History of pelvic inflammatory disease: Pelvic inflammatory disease (PID) often leads to scarring and deformation of the pelvic cavity, which is thought to increase risk for ectopic pregnancy. A French study reported the risk of ectopic in women with a history of PID to be 3.4 times higher than in women who had never experienced PID;
- History of sexually transmitted infection (particularly chlamydia and gonorrhoea): Women with a history of STI are more likely to develop an ectopic pregnancy and a history of multiple STIs may increase the risk even further. STIs are associated with pelvic infection, post inflammatory scarring and distortion of normal reproductive anatomy which appear to cause the increased risk of ectopic pregnancy;
- Many lifetime sexual partners
- Age: The risk of ectopic pregnancy increases with age. Women who are more than 40 years of age are 2.9 times more likely to develop an ectopic pregnancy if they become pregnant, than women who are 25-29 years;
- History of infertility: Women who have been infertile in the past are more likely to develop an ectopic pregnancy than those who have not been infertile. The risk of developing an ectopic pregnancy increases with the number of years of infertility. Women who have been infertile for two or more years are 2.7 times more likely, women who have been infertile for 1-2 years are 2.6 times more likely, and those who have been infertile for less than one year 2.1 times more likely to develop an ectopic pregnancy than women who have never been infertile;
- History of using assisted reproduction techniques: Ectopic pregnancies account for some 4% of all pregnancies in women who have used assisted reproductive techniques, compared to estimated 2% of pregnancies in total;
History of, or current, intrauterine contraceptive device use: Women who have previously used an intrauterine device are 1.3 times more likely to develop an ectopic pregnancy than those who have not. When a woman who is using an intrauterine device becomes pregnant (a rare event), there is a high chance the pregnancy is ectopic;
- History of tubal surgery: Women who have undergone surgery involving the fallopian tubes are 4 times more likely to have an ectopic pregnancy than those who have not had tubal surgery;
- Sterilisation: Pregnancy in general is uncommon following sterilisation, however when it does occur, pregnancy is usually ectopic. Women sterilised using the bipolar coagulation technique had the highest rate of ectopic pregnancy following sterilisation (17.3 events per 1000 sterilisations), while women sterilised by postpartum partial salpingectomy, had the lowest rate of ectopic pregnancy (1.5 per 1000). Women under 30 years of age at the time of sterilisation had a higher risk of ectopic pregnancy than those who were aged 30 or more when sterilised.
The following factor haa a protective effect in relation to ectopic pregnancy:
- History of oral contraceptive use: Women who have used oral contraceptives in the past are less likely to develop an ectopic pregnancy than those who have never used oral contraceptives.
Progression
Following fertilisation of the egg, the embryo of an ectopic pregnancy implants outside the uterus and grows. In some cases the pregnancy will naturally resolve (i.e. the woman will have a miscarriage and the embryo will be expelled from the body) however when spontaneous abortion (i.e. miscarriage) does not occur, the embryo will continue to grow. If left untreated the embryo can grow too large to be accommodated by the surrounding organs. In this case the embryo can cause a rupture and considerably damage the reproductive organs. In very serious cases, ectopic pregnancy also poses a threat to the pregnant woman’s life.
Symptoms
Women with an ectopic pregnancy will appear pregnant (i.e. when a pregnancy test is conducted on a woman with ectopic pregnancy, the result will be positive). The most common symptoms of ectopic pregnancy are lower abdominal pain (reported by over 90% of women with ectopic pregnancy) and abnormal menstrual bleeding (reported by over 80% of women). If left untreated, the consequences of ectopic pregnancy include damage to the reproductive organs, reduced fertility and in the most severe cases, death.
Clinical Examination
How is it Diagnosed
If a pregnancy test, questioning and physical examination of the pelvis indicate the possibility of ectopic pregnancy, further tests need to be conducted, in most cases a transvaginal ultrasound. Depending on the equipment and specialists available, this may require the patient be referred to a hospital or specialist.
A transvaginal ultrasound is an ultrasound test which focuses on the vaginal area. When assessing a normal pregnancy occurring in the uterus, transabdominal ultrasound is used. The ultrasound test enables a health specialist to look inside the woman and see whether there are any abnormalities (e.g. a growing mass in the fallopian tubes) which may be the embryo of an ectopic pregnancy.
Ultrasound is often used in conjunction with measurements of the level of a hormone called human chorionic gonadotrophin. It is the same hormone measured in a standard urine pregnancy test and can increase the accuracy of diagnosis using ultrasound.
In rare cases, either when an ectopic pregnancy cannot be identified using ultrasound, or when a woman with suspected ectopic pregnancy presents in a critical state (e.g. collapsed with suspected rupture of the ectopic pregnancy) laparoscopy may be performed to diagnose the ectopic pregnancy. However in most case laparoscopy is used only in the treatment of ectopic pregnancy.
Prognosis

Treatment

When treatment is agreed upon, there are a range of treatment options. Surgery has traditionally been the only method of treating ectopic pregnancy and remains the most common form of treatment. However medical treatment (i.e. the prescription and administration of medication to induce termination of the ectopic pregnancy) and expectant monitoring of the ectopic pregnancy (i.e. waiting to see if spontaneous abortion occurs) are becoming increasingly popular. Choice of treatment will depend on the gestation of the ectopic pregnancy, health of the pregnant woman, her personal wishes and availability of ultrasonographic and laparoscopic equipment and expertise.
Expectant monitoring
Expectant monitoring is appropriate for managing select cases of ectopic pregnancy. If this is the preferred method of treatment, a health practitioner will probably measure the pregnant woman’s human chorionic gonadotrophin concentrations to assess whether expectant management is appropriate. Where human chorionic gonadotrophin levels are relatively low, expectant management is successful in treating 88% of cases. However where expectant management fails, medical and surgical treatment is necessary.
Medical treatment
Methotrexate can also be injected straight into the ectopic gestational sac, however this technique requires laparoscopy and has a higher failure rate than intra muscular injection.
Surgical treatment
Surgery can be conservative or radical depending on the length of gestation at diagnosis, presence or absence of rupture and health of the pregnant woman. Common surgical treatments are:
- Salpingostomy: is a conservative surgical treatment for ectopic pregnancy which involves the removal of the embryoalone.
- Salpingectomy:is a radical surgical treatment for ectopic pregnancy which involves the removal of the embryo and the tube in which is occurs. It is recommended in cases where the fallopian tube is extensively diseased or damaged and risk of ectopic pregnancy recurring is high.
Either type of surgery can be performed via laparoscopy or laparotomy. Laparoscopic surgery is less costly and is associated with shorter hospital stays and recovery times but there is a higher rate of recurring problems in the long term following laparoscopic surgery.
Treatment for the psychological side effects
Ectopic pregnancy can be distressing and often results in feelings of grief, loss and depression. Patients may require counseling and/or support group participation to help them cope with the psychological difficulties of ectopic pregnancy.
References
- Lee, J.W. Sohn, K.M. Jung, H.S. “Retroperitonal Ectopic Pregnancy [Case Report]” in Am J Roentgen 2005; 184:1600-1601.
- Drife J, Lewis G. eds. Why mothers die. Triennial report 2000-2002. Confidential enquiries into maternal deaths. UK: RCOG, 2004, available from: www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsStatistics/DH_4009520
- Sullivan, E. Hall, B. King, J. 2008, Maternal Deaths in Australia 2003-2005. Australian Institute of Health and Welfare, available from: http://www.npsu.unsw.edu.au
- Conduous, G. “Ectopic Pregnancy: Risk factors and diagnosis” in Aust Fam Phys, 2006, 35(11):8547.
- Rajkhowa M. Glass M.R. Rutherford A.J. et al, “Trends in the incidence of ectopic pregnancy in England and Wales from 1966 to 1996” in BJOG, 2000, 107(3):369-74
- Boufous, S. Quartararo, M. Moshin, M. Parker, J. “Trends in the incidence of ectopic pregnancy 1990-1998″in Aust NZ J Obstet Gynaecol, 2001, 41(4):436-8.
- Bouyer. J. Coste, J. Shojaei, T. “Risk factors for Ectopic Pregnancy: A Comprehensive Analysis Based on a Large Case-Control, Population-based study in France” in Am J Epi, 2003, 157(3):185-194.
- Chen, M.Y. Fairly, C.K. Donovan, B. “Discordance between trends in Chlamydia notifications and hospital admission rates for Chlamydia related diseases in New South Wales, Australia, Sex Transm Inf, 2005, 81, 318-22.
- Egger, M. Low, N. Davey-Smith,G. et al, “Screening for Chlamydial Infections and the risk of ectopic pregnancy in Sweden: ecological analysis” in BMJ, 1998, 316:1776-1780.
- Virk, J. Zhang, J. Olsen, J. “Medical Abortion and the risk of subsequent adverse pregnancy outcomes” in NEMJ, 2007, 357:648-53.
- Rolle, C.J. Wai, C.Y. Bawdon, R. “Unilateral Twin Ectopic Pregnancy in a Patient with a history of Multiple Sexually Transmitted Infections” in Infect Dis Obstet Gynecol. 2006; 2006: 10306.
- Strandell, A. Thorborn, J. Hamberger, L. “Risk Factors for Ectopic Pregnancy in Assisted Reproduction” Fertil Steril, 1999, 71(2):282-286.
- Peterson, H.B. Xia, Z. Hughes, J. “The risk of ectopic pregnancy following tubal sterilisation” in NEJM, 1997, 336:762-7.
- Tay, J. Moore, J. Walker, J. “Ectopic Pregnancy [Clinical Review]” in BMJ, 2000, 320, 916-19.
- Ludwig, M. “Heterotopic pregnancy in a spontaneous cycle: do not forget about it!” in Eur J Obstet Gynaecol Reprod Biol, 2003, 87(1):91-93.
- Ankum, W.M. “Diagnosing Suspected Ectopic Pregnancy [Editorial]” in BMJ, 2000, 321:1235-36.
- Kaczor, C. “Moral Absolutism and Ectopic Pregnancy” in J Med Philos. 2001, 26(1):61-74.
- Hajenius PJ, Mol F, Mol BWJ, Bossuyt PMM, Ankum WM, van der Veen F. Interventions for tubal ectopic pregnancy. Cochrane Database of Syst Rev, 2007, Issue 1. Art. No.: CD000324
- Barnhart KT. Ectopic pregnancy. New England Journal of Medicine 2009; 361: 379-87.
- Ectopic pregnancy – United States, 1990-1992. MMWR Morb Mortal Wkly Rep 1995; 44: 46-8.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.

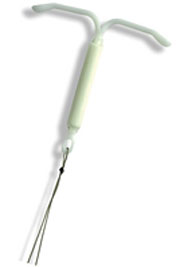 History of, or current, intrauterine contraceptive device use: Women who have previously used an
History of, or current, intrauterine contraceptive device use: Women who have previously used an 





