- What is breast conserving surgery?
- Who can have breast conserving surgery?
- What are the risks of breast conserving surgery?
- Breast conserving surgery or mastectomy?
- Advantages and disadvantages of breast conserving surgery
What is breast conserving surgery?

Breast conserving surgery is an alternative treatment to mastectomy (removal of the entire breast). Breast conserving surgery may be associated with better cosmetic outcomes than mastectomy, as only a small mass of breast tissue is removed. Women who undergo breast conserving surgery usually also require axillary dissection (removal of the lymph nodes in the armpit) and radiotherapy to the affected breast after surgery. These help reduce the risk of recurrence of the tumour.
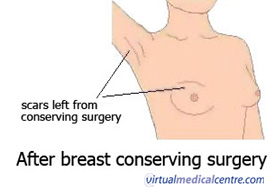
The pictures below show the incisions (cuts) that are made during breast conserving surgery and what the scars might look like after surgery. The exact position of the scar on the breast will depend on the location of the lump to be removed.
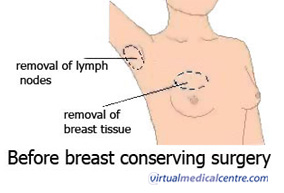
Axillary dissection refers to the removal of the lymph nodes in the armpit (axilla) on the same side as the affected breast. This is done because axillary lymph nodes are one of the commonest first sites for breast cancer to spread to. By removing some of the axillary lymph nodes during surgery, it is possible to find out whether the cancer has spread to these nodes. This may help plan future treatment such as chemotherapy or radiotherapy. Axillary dissection can also help by removing nodes the cancer has already spread to, reducing the likelihood that cancer will grow in the axilla.
Axillary dissection is important, but is associated with some side effects. These may include:
- Bruising under the arm, particularly in the days and weeks immediately after surgery;
- A feeling of numbness or tingling in the arm, shoulder or chest;
- Stiffness of the shoulder, which may be temporary or may remain;
- Lymphoedema: Swelling in the arm, hand or chest which develops months or years after surgery because the normal drainage function of the lymph nodes has been impaired. This cannot be cured, but some treatments are available to reduce the swelling.
For some women with very small breast cancers, axillary dissection is not considered necessary. In other women who are considered at high risk of axillary recurrence (growth of cancer in the lymph nodes of the axilla), radiotherapy to the armpit may be recommended in addition to surgery.
Who can have breast conserving surgery?

Breast conserving surgery may not be possible if:
- The tumour is multifocal, i.e. there is more than one tumour ‘mass’ in the breast;
- The tumour involves multiple quadrants (areas) of the breast;
- There is extensive intraductal disease;
- The tumour involves the nipple-areola complex (the cosmetic outcome is usually poor in these cases);
Because patients who undergo CLE must usually have radiotherapy after surgery, breast conserving surgery may also not be appropriate for women who:
- Have a history of connective tissue disease involving the skin (such as scleroderma). This is because people with connective tissue disease can suffer severe side effects from radiotherapy;
- Have a history of previous moderate- or high-dose radiotherapy to the chest wall; or
- Have no access to radiotherapy facilities.
What are the risks of breast conserving surgery?
Breast conserving surgery is a surgical procedure requiring a general anaesthetic. Patients will usually stay in hospital between one day and one week.
Some side effects include:
- Swelling or bruising around the operation sites is common;
- A fluid collection known as a ‘seroma’ may develop in or around the surgical scars. This is not dangerous but may require draining;
- Infection, either in the scar in the breast or in the axilla (armpit) is possible;
- Bleeding in either scar is also rarely seen.
The risks of axillary dissection are described above.
Breast conserving surgery or mastectomy?

- Over a 10-year period, there is no difference in the rate of survival for women who undergo mastectomy versus those who undergo breast conserving surgery with radiotherapy.
- The rate of distant metastasis (spread of cancer beyond the breast and lymph nodes) is also no different between the two groups.
There is a slightly higher rate of local recurrence (re-appearance of cancer in the affected breast) for women who undergo complete local excision, compared to those who have a mastectomy. However, as shown above, this does not make any difference to survival.
Overall, breast conserving surgery with radiotherapy is considered equally as effective as mastectomy.
Advantages and disadvantages of breast conserving surgery
The most obvious advantage of breast conserving surgery is a better cosmetic outcome. Though the surgery does leave a scar, and the shape of the breast will be different, women who have breast conserving surgery are usually happier about their bodies and have a better self-image than women who have a mastectomy. Sexuality may be less affected. In addition, women who undergo breast conserving surgery do not need to undergo breast reconstruction surgery or have external breast prostheses fitted.
The disadvantage of choosing breast conserving surgery is the need for radiotherapy after surgery. Radiotherapy is essential after breast conserving surgery as it reduces the risk that the cancer will return, and improves survival. However, it can be a lengthy process – most women have radiotherapy once per day, five days a week, for five or six weeks – and there are some side effects. There is also a risk that breast conserving surgery will not be able to remove the whole tumour. Women who have had a complete local excision (CLE) where the surgical margins are not clear may need further surgery, including the possibility of mastectomy.
More information
 |
For information on breast cancer, types of breast cancer and its investigations and treatments, as well as some useful videos, see Breast Cancer. |
References
- Braunwald, Fauci, Kasper, Hauser, Longo, Jameson. Harrison’s Principles of Internal Medicine. 16th Edition. McGraw-Hill. 2001
- National Breast Cancer Centre. 2001. ‘Clinical practice guidelines for the management of early breast cancer: Second edition’. National Breast Cancer Centre, Camperdown, NSW. [online] Available from: http://www.nhmrc.gov.au/publications/synopses/cp74syn.htm
- National Breast Cancer Centre. 2003. ‘A guide for women with early breast cancer.’ National Breast Cancer Centre, Camperdown, NSW. [online] Available from: http://www.nbcc.org.au/resources/documents/EBC_earlyguide.pdf
- National Comprehensive Cancer Network (NCCN) 2007. ‘Clinical Practice Guidelines in Oncology: Breast Cancer’. [online] Available from: http://www.nccn.org/professionals/physician_gls/default.asp.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.