- Introduction
- Why do sexual feelings change after menopause?
- How many women have sexual complaints after menopause?
- When do sexual symptoms of menopause occur?
- How does sex feel after menopause?
- Assessing sexual function during and after menopause
- Improving sexual function during and after menopause
- Tips for having a great sex life after menopause
Introduction

As hormones influence the function of genital organs (e.g. vaginal lubrication) and also regulate libido, many of the symptoms which occur in the menopausal transition are related to sexual function. Menopause is also a time of significant psychosocial changes for women (e.g. changes to their maternal role resulting from children leaving home) and these changes may also influence a woman’s sexual function.
While menopausal changes and the symptoms which result from them are natural and experienced by all women to a greater or lesser degree, they may cause distress and reduce quality of life for many women. While many symptoms of menopause are temporary (e.g. hot flushes) changes to sexual function which occur at menopause are typically permanent.
 |
For more information about menopause, see Menopause.
|
Why do sexual feelings change after menopause?
Hormonal changes
Sexual feelings change in the peri-menopausal period and persist post-menopause due to hormonal changes. Prior to menopause, the ovaries produce the majority of oestrogen, progesterone and testosterone in a woman’s body. As ovarian hormone production ceases post-menopause, oestrogen, progesterone and testosterone levels decline.
Oestrogen (and to a lesser degree progesterone) largely regulate vaginal function (in particular blood flow to the vagina in response to physical stimulation and vaginal lubrication), while testosterone affects the functioning of the vulva. Reduced hormone levels in the menopausal period therefore affect the function of the vagina and vulva.
The vagina is a complex structure, consisting of several layers, a fibrous outer layer or rough skin cells, a middle muscular layer and smooth inner layer of skin cells known as the epithelium. The majority of the body’s cells which utilise and have their function regulated by oestrogen and progesterone are found in the vagina. The cells of the vulva comprise the majority of the body’s cells which utilise and are regulated by testosterone.
In the pre-menopausal period when levels of oestrogen and other hormones are high, the vagina is characterised by:
- Relatively high blood flow;
- A thicker epithelium, that is a thicker layer of smooth skin cells;
- Greater acidity; and
- Increased lubrication.
The changes to hormone production which occur at menopause, and particularly the rapid decline in oestrogen production, cause the skin and muscles cells of the vagina and vulva to deteriorate.
The physiology of the vagina changes and the vaginal walls, which are often only a few cell layers thick, become thinner. Their appearance and texture also changes. Post-menopause, the vaginal walls become pale, smoother and less elastic due to degeneration of the connective tissue components of the vagina (e.g. collagen, smooth muscle) which usually give them their elasticity. In addition the vagina typically becomes shorter and narrower as a result of hormonal changes which occur at menopause.
Vaginal lubrication
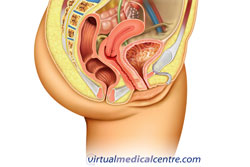
 |
More information on vaginal dryness. |
Vaginal blood flow also reduces as a result of the hormonal changes which occur at menopause. Reduced blood flow causes the vulva to be less sensitive to touch. It also further affects vaginal lubrication as in the absence of adequate vaginal blood flow during sexual activity, the amount of lubricant which passes out of the vaginal membrane to lubricate the vaginal walls also decreases. This further increases the likelihood of vaginal dryness and trauma.
Acidity of the vaginal environment
The vaginal environment becomes less acidic in the post-menopausal period as a result of physical changes (e.g. changes to the shape and texture of the vagina) and reduced glycogen production which occurs as a result of hormonal changes. This in turn reduces concentrations of lactic acid producing lactobacilli, microorganisms which colonise the vaginal tract pre-menopause and maintain an acidic vaginal environment. The acidity of the vaginal tract in the pre-menopausal period provides considerable protection against infection. With increasing alkalinity the vagina becomes more susceptible to infection, as microorganisms which could previously not survive in the acidic vaginal environment can more easily colonise the vaginal tract.
Indirect effects of hormonal changes on sexual function
Reduced oestrogen levels may also affect a woman’s sexual response indirectly. In the post-menopausal period, many women experience vasomotor symptoms (e.g. hot flushes) which may cause insomnia, irritability and reduced skin sensitivity. These in turn, may affect a woman’s sexual desire.

A woman’s libido and sexual response are highly contextual and heavily influenced by psychosocial factors, that is, factors relating to the psychological health and social context. As a result, many women with biologically and physiologically normal genital systems experience sexual dysfunction. Such sexual dysfunctions may become more prevalent at menopause, because of the significant psychological and social changes which also occur in a woman’s life at this time. For example, a menopausal woman’s ageing partner may experience sexual dysfunction which can significantly affect the woman’s sexual function, or the woman may be coping with upheavals such as changes to her maternal role because of her children leaving home.
A woman’s satisfaction with her sexual relationship and her psychological wellbeing also have an important influence on her sexual desire in the menopausal period. One large study found that having positive feelings for their partner and good psychological health were more important predictors for a woman having a good libido in the post-menopausal period than hormone levels. A study of 438 Australian women also reported that psychosocial factors (including previous sexual function, partner change and satisfaction with sexual partner) had a more important influence on sexual response than oestrogen levels (although oestrogen levels were correlated with sexual function).
Other non-hormonal factors which may influence sexual function include:
- Emotional wellbeing, including the presence or absence of psychological disorders such as depression and anxiety;
- Emotional satisfaction with the relationship;
- Satisfaction with previous sexual encounters;
- Fatigue;
- Medication use, in particular use of antidepressant medications;
- Thyroid disorder;
- Hyperprolactinaemia (elevated blood prolactin levels).
How many women have sexual complaints after menopause?

Urogenital symptoms, including increased frequency or urgency of urination and pain when urinating may also be reported and indirectly affect women’s sexual function. Women are 2-3 times more likely than men to experience reduced libido as they age.
When do sexual symptoms of menopause occur?
The timing of menopause-associated sexual dysfunctions in relation to menopause varies between women. Typically, women experience symptoms in the pre- and peri-menopausal periods and for about five years after their final menstrual bleeding. In some women symptoms persist beyond five years, and sexual and urogenital symptoms are particularly likely to persist (compared to other symptoms such as vasomotor symptoms). Sometimes the sexual symptoms of menopause persist permanently.
How does sex feel after menopause?
Most women experience changes in the way sex feels around the time of menopause. Changes to sexual feeling reported by menopausal women commonly include:
- Vaginal dryness;
- Dyspareunia (pain during sex);
- Vulvo-vaginal itching; and/or
- Vulvo-vaginal irritation.
Women may also experience a reduction in the size of their breasts and decreased nipple sensation.
Urogenital symptoms may make sex uncomfortable or painful or reduce a woman’s libido. While many women experience reduced libido following menopause, it is important to note that some feel sexier and freer about their sexual interactions.
It is also important to note that many women who do experience changed sexual feelings do not feel these changes affect the quality of their sex life, and many women continue to enjoy sex after menopause despite it feeling different. It is also important for menopausal women to be cognisant that sexual feelings change differently for each woman. While the majority report reduced sexual desire, a considerable proportion also report increasing desire post-menopause. For example, in one qualitative study, a quarter of participants reported that their libido increased after menopause.
Women may also experience changes in the way particular aspects of sex feel, for example the intensity with which they experience orgasm. However, the direction of change varies between women, with some women experiencing more intense and others less intense orgasms. It is important to note that in many cases these changed sexual feelings are not perceived by women as related to the hormonal and physiological changes of menopause. Rather women are more likely to perceive these changes occur as a result of changing sexual partners or techniques (e.g. masturbation rather than intercourse).
In around one third of couples, changes to the male partner’s sexual function (e.g. the woman’s partner may begin to experience erectile dysfunction as he ages) is the cause of female sexual dysfunction post-menopause.
There is clearly diversity in the changes women experience following menopause and many factors other than hormonal changes influence sexual feelings. Nevertheless, there is also considerable evidence that hormonal factors do influence the feeling of sex post-menopause.
Assessing sexual function during and after menopause

The assessment of post-menopausal sexual dysfunction is undertaken from a bio-psycho-social perspective, that is, recognising that biological, psychological and social factors all influence women’s sexuality. This usually means that the woman’s partner (if she has one) is involved in the assessment and treatment process, as factors relating to the partner (e.g. the interpersonal relationship, his sexual function) heavily influence the sexual functioning of the female partner.
When a menopausal woman reports sexual symptoms to a doctor, the doctor will typically begin investigating the symptoms by taking a detailed sexual and medical history. That involves asking lots of questions about the woman’s health and sexuality, now and in the past. The doctor will typically enquire about:
- The woman’s current sexual function and whether or not she has experienced sexual dysfunction or problems in the past;
- Her partner’s sexual function and whether there are any issues which may affect the her sexual function (e.g. partner experience of erectile dysfunction);
- Relationship history including any stressors or issues in the relationship (e.g. lack of trust) which may affect sexual function;
- Investigation of psychosocial factors (e.g. religious beliefs, life upheavals) which may influence sexual function;
- Medical history including previous sexual conditions (e.g. sexually transmitted infections) or dysfunctions and current medication use;
- Blood tests, including assessment of testosterone levels may be conducted in some cases;
- History of psychological complaints including depression as these are commonly associated with sexual problems in women.
When asking these questions the doctor will consider whether the symptoms of sexual dysfunction are related to the hormonal changes of menopause, or whether there are other factors causing or contributing to the woman’s sexual symptoms. As interpersonal and relationship factors exert a significant influence on sexual function, ideally both partners are interviewed, separately and as a couple.
A physical examination may also be conducted, particularly if the woman’s sexual complaints include painful sexual intercourse or arousal difficulties.
Improving sexual function during and after menopause

Non-hormonal vaginal lubricants
In many cases non-hormonal vaginal moisturisers (e.g. water based lubricants) are sufficient to relieve symptoms, in particular vaginal dryness. These products are usually recommended to relieve symptoms before other treatments, which involve greater side effects are trialled. Water-based lubricants are usually recommended as they are more effective than oil-based lubricants such as petroleum jelly.
Sexual dysfunctions can cause distress and other psychological problems including mood changes, depression and anxiety. Existing psychological problems (e.g. depression) may also contribute to difficulties with sexual function. It is therefore often useful to involve women’s partners in the treatment of post-menopausal sexual dysfunction, and it is recommended that both partners be interviewed alone and as a couple in the assessment of these problems.
Couples with interpersonal issues in their relationship may benefit from consulting a specialist for assessment and treatment (e.g. couples therapy or sex therapy). It may also be important to assess the male partner’s sexual function, as male sexual dysfunction often undermines the female partner’s functioning.
Psychological interventions may also assist menopausal women to cope with other stressors in their life which influence the severity of menopause symptoms, such as stress in the workplace, or dealing with children leaving home.
It may also be important for the couple to learn new sexual techniques. Learning and normalising the use of non-penetrative sexual techniques can be important for women experiencing pain during intercourse, as pain typically worsens when women persist with intercourse when experiencing pain. In other cases, couples may benefit from increasing foreplay before vaginal penetration is attempted, and it may be important to learn sexual techniques which involve greater vulval and clitoral stimulation.
Sexual permissiveness training may also be important, to teach the couple to be happy about their sexuality. As ageing individuals are not typically perceived as sexual in many societies, couples may feel guilty about sex as they age, or not be aware that they can still have a fulfilling sex life.
 |
For more information, see Sex Therapy. |
While herbal (often termed natural) therapies are more commonly applied to the treatment of hot flushes, they may also be used to treat menopause-related sexual dysfunction. However, there is currently insufficient evidence to determine whether or not these remedies are an effective treatment. Their use is not currently recommended for the treatment of sexual symptoms of menopause.
Red clover isoflavones (oestrogens which occur naturally in plants) have been used to treat sexual symptoms. It has shown a positive effect on vaginal tissue. However, further research regarding their effectiveness in relieving vaginal dryness or libido is warranted.
Lycopodium clavatum (also known as Wolf’s foot) is a homeopathic remedy used to treat sexual symptoms of menopause. There is little evidence available on its efficacy.
There are numerous hormonal therapies which are highly effective in relieving sexual symptoms in menopausal and post-menopausal women. However, it is important to note that hormonal therapies are associated with adverse side effects and cannot be used by a substantial proportion of women due to side effects and health risks.
In addition it is important to be cognisant that many sexual dysfunctions result from complex interactions between biological, psychological and social factors. In the presence of psychological and social inhibitors of sexual function, biological therapies such as hormone replacement therapy, may be ineffective.
Oestrogen therapy is the standard second line treatment for sexual symptoms of menopause, that is, it is the treatment which is most likely to be instituted if a woman finds vaginal lubricants (first line treatment) are ineffective in relieving her symptoms. Oestrogen therapy is effective in relieving sexual symptoms in 80-90% of women. It can be delivered locally to the vagina (e.g. via oestrogen-containing vaginal lubricants which are absorbed locally and only affect the vaginal cells) or as low dose systemic therapy (e.g. as oestrogen-containing tablets, the oestrogen from which is distributed through and affects the entire body or has a systemic effect). As local modes of administration provide oestrogen only to the vagina and not the entire body, they are associated with fewer side effects.
The most appropriate type of oestrogen therapy depends on the causes of sexual dysfunction. For example, an oestrogen-releasing ring is more effective than an oestrogen releasing tablet in reducing vaginal rash, but less effective for relieving vaginal dryness, compared to an oestrogen containing tablet. It is important that women discuss their symptoms openly and honestly with their doctor so they can determine which treatment is most appropriate.
Local therapies include oestrogen-containing creams which are applied to the vagina and oestrogen-releasing tablets and rings which are inserted into the vagina. In women who experience only vaginal symptoms and do not experience other symptoms of menopause (e.g. hot flushes) local oestrogen-therapy is preferred over systemic therapy, as it raises systemic oestrogen levels very little, and therefore is associated with fewer side effects.
Local oestrogen therapies are suitable for most women, but those with hormone-dependent cancers should consult their oncologist before treatment is instituted. All local oestrogen therapies have demonstrated similar efficacy, so the most appropriate product is selected based on the woman’s preference and availability. Therapy usually continues as long as symptoms persist.
While local therapy can effectively relieve vaginal symptoms of menopause, it is not an effective treatment for vasomotor symptoms and is not associated with a reduced risk of osteoporosis as is systemic therapy. Thus systemic therapy may be recommended for menopausal women who also experience vasomotor symptoms.
Systemic treatment is indicated for women with sexual and other (e.g. vasomotor) symptoms of menopause, but it is not indicated for the treatment of vaginal symptoms alone. It is contraindicated in a substantial proportion of women (e.g. those with a history of hormone dependent cancer) because it carries a number of health risks, including an increased risk of cancer.
When oestrogen therapy is systemic it is typically administered in conjunction with progesterone to reduce potential adverse oestrogenic side effects, in particular the increased risk of endometrial cancer associated with sole-oestrogen therapy. Progesterone is typically not necessary for women receiving local oestrogen therapy, although it may be considered for women using frequent or high doses of local-oestrogen products.
Progesterone therapy has not been tested as a treatment for sexual dysfunction associated with menopause. However, evidence from one study suggests that progesterone may inhibit sexual desire.
Testosterone may also be administered in conjunction with oestrogen. Limited available data suggests that combined testosterone-oestrogen therapy is more effective in reducing menopause-related sexual dysfunction than oestrogen therapy alone.
Tibolone is a synthetically produced hormone with oestrogenic, progesterogenic and androgenic properties. It has been demonstrated effective in reducing some symptoms of menopause. Trials have shown this drug effective in reducing vaginal dryness, although results regarding its effect on libido are somewhat conflicting. One small trial found that women treated with tibolone experienced a greater number of sexual fantasies compared to women who did not receive tibolone, while other trials have reported no improvement in libido following tibolone therapy. Women considering this therapy should be aware that tibolone increases the risk of recurrence in patients who have been treated for breast cancer.
Tips for having a great sex life after menopause
Having a great sex life is possible after menopause. There are many techniques and strategies which help women optimise their sex life after menopause.
 |
For more information, sees Tips for a Great Sex Life after Menopause
. |
More information
 |
For more information on menopause, including symptoms and management of menopause, as well as some useful animations and videos, see Menopause. |
 |
For more information on psychology and psychotherapy, including different types of therapy, see Psychology and Psychotherapy. |
References
- Burbos N, Morris E. Menopausal symptoms. BMJ Clin Evid. 2010; 2: 804.
- Hinchliff S, Gott M, Ingleton C. Sex, menopause and social context: A qualitative study with heterosexual women. J Health Psychol. 2010;15(5):724-33. [Abstract]
- North American Menopause Society. Estrogen and progestogen use in postmenopausal women: 2010 position statement of The North American Menopause Society. Menopause. 2010;17(2):242-55. [Abstract]
- Bélisle S, Blake J, Basson R, et al. Canadian consensus conference on menopause, 2006 update. J Obstet Gynaecol Can. 2006;28(2 Suppl 1):S7-S94. [Abstract | Full text]
- Menopause: What is it? BMJ patient leaflet [online]. London, UK: BMJ Group; 6 July 2010 [cited 25 July 2010]. Available from: URL link
- Decks AA, McCabe MP. Sexual function and the menopausal woman: The importance of age and partner’s sexual function. J Sex Res. 2001;38(3):219-25. [Abstract]
- Grady D. Clinical practice. Management of menopausal symptoms. N Engl J Med. 2006; 355(22):2338-47. [Full text]
- Menopause support: Fixes for a stalled sex life [online]. Mayfield Heights, OH: North American Menopause Society; 4 March 2010 [cited 26 July 2010]. Available from: URL link
- Cobin RH, Futterweit W, Ginzburg SB, et al. American Association of Clinical Endocrinologists medical guidelines for clinical practice for the diagnosis and treatment of menopause. Endocr Pract. 2006;12(3):315-37. [Full text]
- Phillips NA. Female sexual dysfunction: Evaluation and treatment. Am Fam Physician. 2000;62(1):127-36, 141-2. [Abstract]
- AgePage: Menopause [online]. Gaithersburg, MD: National Institute on Aging; April 2008. [cited 13 July 2010]. Available from: URL link
- Leventhal JL. Management of libido problems in menopause. Presented at: Cojoint Annual Meeting of the American Society for Reproductive Medicine and the Canadian Fertility and Andrology Society 32nd Annual Postgraduate Program. Toronto, Canada; 25-26 September 1999. Available from: URL link
- Bartlik B, Goldstein MZ. Maintaining sexual health after menopause. Psychiatr Serv. 2000;51(6):751-3. [Full text]
- Managing menopause: Emotional wellbeing [online]. Clayton, VIC: Jean Hailes Foundation for Women’s Health; 26 October 2009 [cited 13 July 2010]. Available from: URL link
- Abernethy K, Hillard A, Holloway D, et al. Complementary approaches to menopausal symptoms: RCN guidance for nurses, midwives and health visitors. London, UK: Royal College of Nursing; 2 October 2007 [cited 25 July 2010]. Available from: URL link
- Basson R, Berman J, Burnett A, et al. Report of the international consensus development conference on female sexual dysfunction: Definitions and classifications. J Urol. 2000;163(3):888-93. [Abstract]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







