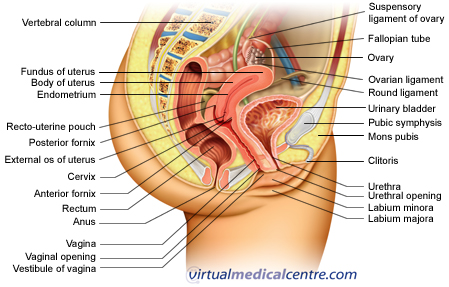
- What is Pelvic Inflammatory Disease (PID)?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- Pelvic Inflammatory Disease (PID) Prevention
- References
What is Pelvic Inflammatory Disease (PID)?

PID may be used to refer to a number of more specific conditions, including:
- Endometriosis (a condition in which tissues that normally grow in the womb grow outside the womb);
- Salpingitis (inflammation of the tubes in the womb);
- Parametritis (inflammation of the tissues which surround the womb);
- Oophoritis (inflammation of one of the ovaries);
- Tubo-ovarian abscess (pus in the fallopian tubes or ovaries); and
- Pelvic peritonitis (inflammation of the tissues surrounding the pelvis).
Statistics
PID usually produces general symptoms such as fever and vaginal discharge, which also occur with many other conditions or diseases (e.g. STIs, pregnancy). In some cases, a woman with PID will not have any symptoms and the inflammation will go away without medical treatment. As a result, up to two-thirds of women with PID do not even realise they have the condition.
The general, or sometimes lack, of symptoms in PID make it a challenging condition for doctors to diagnose. The exact number of women who experience PID each year is difficult to determine.Statistics probably underestimate the true number, although they clearly show that PID is a common condition.
10–15% of women experience PID at least once in their life, most commonly when they are aged 20–24. An estimated one million women are treated for PID in the United States each year, and some 75,000 suffer infertility because of damage to the uterus and fallopian tubes resulting from untreated PID.
In the United Kingdom, 1.7% of presentations to a doctor by women aged 16–46 years are for PID. Approximately 1 in 60 visits to general practitioners by women < 45 years of age are PID-related.
Information about the number of PID cases which doctors in Australia treat each year is limited, but evidence suggests that it is declining. For example, in NSW incidence rates fell from 165 cases per 100,000 women in 1992 to 64 cases per 100,000 women in 2001. This decline occurred despite an increase in the number of chlamydial infections, which are a common cause of PID. Doctors believe the decline is probably a reflection of earlier diagnosis and treatment of chlamydial infections, as early treatment can prevent complications such as PID.
Limited available evidence suggests that Aboriginal women have a greater risk of PID than non-Aboriginal women. Records from Royal Darwin Hospital show that Aboriginal women were seven times more likely to be admitted for PID than non-Aboriginal women.
Risk Factors
- Have been infected with C. trachomatis or N. gonorrhoeae, the bacteria that cause chlamydia and gonorrhoea. Chlamydia and/or gonorrhoea infection is the cause of 60–80% of PID cases in women aged under 25 years. PID may not develop for some time after these infections are transmitted. It may occur even if the woman never experienced symptoms of chlamydia or gonorrhoea, as these infections are often transmitted without causing obvious symptoms;
- Have previously experienced PID;
- Have previously had bacterial vaginosis (an infection caused by the excessive growth of bacteria which normally inhabit the vagina, including Gardnerella vaginalis). However, women who have had bacterial vaginosis are much less likely to get PID than those who have had chlamydia or gonorrhoea;
- Have experienced Mycoplasma genitalium infection in the past. It is a sexually transmitted organism that most commonly causes a condition called urethritis (inflammation of the urethra) in men. It also causes cervical infection in women;
- Are young: Adolescents are more likely to experience chlamydia or gonorrhoea infection than their older counterparts. Adolescent women who do become infected with chlamydia or gonorrhoea are more likely than older women to experience PID as a consequence of these infections.Evidence suggests that 15–19-year-olds have a five times greater risk of PID than their older counterparts. The increased incidence in young women is partly related to the immaturity of their reproductive organs. Because their reproductive tracts are not fully matured, teenagers are more susceptible to infection than older women;
- Have recently had an intrauterine contraceptive device (IUD) inserted or removed. IUD insertion or removal increases the risk of PID as it can result in spreading of bacteria which are normally found in the vagina but not in the uterus and the spreading of sexually transmitted organisms (if the woman has an untreated STI). As the IUD is inserted through the vagina into the uterus, bacteria sometimes also enter the uterus at the time of insertion. Doctors often prescribe antibiotics to women having an IUD inserted or removed, as this reduces the risk of the bacteria that enter the uterus multiplying and causing PID. Testing and treating existing STIs prior to insertion also greatly reduces the risk of an infection;
- Have recently terminated a pregnancy or given birth, which may similarly cause the spread of bacteria from the vagina to the uterus. Women are often tested (and if necessary treated) for bacterial vaginosis prior to surgical abortion because this reduces the risk of PID;
- Have recently had gynaecological surgery, which can also cause of the spread of bacteria from the vagina to the uterus, as it often involves inserting instruments into the vagina or uterus;
- Have a greater number of sexual partners. The more sexual partners a woman has, the greater her risk of being exposed to infections which cause PID. Women are also at greater risk if their sexual partner has sex with other partners without using a condom. Women who have more than one partner or a partner who has not been tested for STIs should use condoms as they greatly reduce the risk of contracting an infection during sex;
- Douche: Douching increases the risk of PID because it disturbs the bacteria which normally inhabit the vagina and keep it healthy. Douching can also make it easier for vaginal bacteria to enter the uterus;
- Are of low socioeconomic status;
- Smoke, because smoking impairs the immune system and means that it cannot fight against an infection of the uterus as efficiently as it would otherwise do;
- Have sex during menstruation or just afterwards, as the cervix (entrance to the uterus) is not protected by a plug at this time like it is at other times. As a result it is easier for the bacteria which can cause PID to enter the uterus during menstruation;
- Have genetic factors which may influence the risk of PID.
The use of barrier methods of contraception (e.g. condoms or diaphragms), levonorgestrel contraceptive implants and oral contraceptives are associated with a decreased risk of PID. Hormonal contraceptive use is also associated with a less severe presentation of PID. Less severe PID is less likely to cause infertility, but it is more difficult for a doctor to diagnose.
Progression

- Microorganisms which normally inhabit the vagina. These bacteria usually grow in small concentrations and protect the health of the vagina by preventing infection with other bacteria. However, when they grow abundantly and become too concentrated they can cause infections. Bacteria which normally inhabit the vagina but can cause PID if they grow excessively include:
- Gardnerella vaginalis;
- Haemophilus influenzae;
- Streptococcus agalactiae.
- Cytomegalovirus;
- Mycoplasma hominis;
- Ureaplasma urealyticum (a bacteria which normally inhabits the vagina in small numbers);
- Mycoplasma genitalium (a sexually transmitted organism which causes the majority of male cases of urethritis);
- Escherichia coli (a bacteria commonly found in faeces, which may be more common in individuals who engage in anal sex);
- Peptostreptococcus species (a species of bacteria which normally inhabits the vagina in small numbers);
- Prevotella bivia and other Prevotella species (a species of bacteria which normally inhabits the vagina in small numbers).
In some cases, infections are polymicrobial, meaning that they involve more that one type of microbe. Usually the main bacteria causing the infection is either C. trachomatis or N. gonorrhoeae. Bacteria normally found in the vagina in low concentrations are most likely to be the secondary cause of infection.
Symptoms
PID may not cause symptoms. While, symptoms usually do occur, they are general and also commonly occur with other health conditions including STIs and pregnancy. Doctors therefore usually look for two or more symptoms which might indicate PID. They include:
- Tenderness or the cervix;
- Tenderness of the ovaries;
- Tenderness of the uterus;
- A mass in one or both ovaries;
- Lower abdominal pain or tenderness;
- Abnormal vaginal discharge which is sometimes pus-like;
- Abnormal cervical discharge;
- Abnormal bleeding, including bleeding after sex or between normal menstrual bleeding;
- Increased temperature (oral temperature > 38.3oC);
- Increased pulse rate;
- Vulvovaginal pain;
- Pain during sexual intercourse;
- A diagnosed STI (in which case the doctor will also need to test you for other STIs);
- History of surgery or instrumentation to the uterus (e.g. abortion or IUD insertion).
These symptoms are more likely to indicate PID if they started just after the woman returned to or commenced sexual activity.
Because the symptoms of PID are similar to those of other health conditions, doctors must ensure that the symptoms are not caused by another condition. Other conditions which may have similar symptoms to PID include:
- Ectopic pregnancy: A pregnancy which grows outside the uterus. It is very dangerous to the pregnant woman and the growing foetus cannot develop properly. Women with an ectopic pregnancy need to undergo an abortion. If a doctor suspects ectopic pregnancy might be causing the symptoms, a pregnancy test will be performed;
- Acute appendicitis;
- Endometriosis: A condition in which uterine tissues grow outside the uterus;
- Irritable bowel syndrome: A condition in which bowel movements are difficult to control;
- Other conditions which affect the bowel. These commonly co-occur with PID;
- Other gastrointestinal disorders;
- Ovarian cyst complications, for example when a cyst ruptures or tears;
- Urinary tract infection; or
- Pain of unknown origin.
Clinical Examination

The doctor will also ask about your general health and recent sexual activity, for example when you last had sex, how often you have it, how many sexual partners you have and whether or not you have recently found a new sexual partner. It is important to be honest about your sex life. What you tell the doctor is confidential and will be used to help diagnose what is causing your symptoms.
How is it Diagnosed
If a doctor suspects PID based on the findings of a pelvic examination and the answers to questioning you about your symptoms and sexual activity, further tests might be conducted to increase the certainty of the diagnosis. Tests may also be used to determine whether or not conditions other than PID (e.g. ectopic pregnancy) might be causing the symptoms.
The most common investigations are:
- Microscopy: Examining a smear of vaginal or endocervical (the endometrium which lines the uterus and the cervix which blocks entrance to it) secretions under a microscope. Under a microscope it is possible to check for the presence or absence of:
- Leukocytes: Components of blood that fight against infection. They are commonly found in high concentrations in the vaginal secretions of women who have PID but are also found in the vaginal secretions of women with other STIs so do not give a clear indication on their own;
- Pus cells which indicate pus in the vagina or on the cervix. Pus occurs commonly in cases of PID and other infection. Therefore if no pus is found in the secretions, then PID is unlikely (< 5% chance). However, the presence of pus does not necessarily indicate PID. It may also indicate another infection;
- Bacteria which may be the cause of PID.
- Bacterial culture of vaginal secretions: Culturing or growing vaginal secretions so that any bacteria contained in it can be identified;
- Nucleic acid testing (NAAT) of vaginal secretions or urine: Can detect C. trachomatis or N. gonorrhoeae. which are a common causes of PID;
Other tests may also be conducted if the doctor remains unsure whether or not PID is causing the woman’s symptoms.
Laparoscopy
Laparoscopy is a technique used to view internal body cavities. It involves inserting a small camera into the body. However, laparoscopy misses 15–30% of PID and is not generally used for diagnosing the condition. It is more likely to be used to rule out other possible causes of the symptoms.
Endometrial biopsy
Endometrial biopsy involves removing a tiny piece of the endometrium (the lining of the uterus) for viewing under a microscope. It may be used if a doctor suspects the woman has endometriosis and not PID.
Transvaginal ultrasound
Transvaginal ultrasound may be used when a doctor suspects a woman has appendicitis. It also enables the doctor to see whether or not the fallopian tubes are inflamed and whether or not there are abscesses on the ovaries or fallopian tubes.
Computed tomography or magnetic resonance imaging
CT or MRI are only rarely used in the diagnosis of PID.
Additional laboratory tests
Other laboratory tests which might be conducted include:
- Blood test: To assess for signs of infection;
- STI screening: With a positive result for HIV, hepatitis B or syphilis supporting a diagnosis of PID;
- Pregnancy testing: With a positive test indicating ectopic pregnancy and not PID as the cause of symptoms.
Prognosis

Amongst women who develop symptoms and visit a doctor for treatment with antibiotics, symptoms resolve in 88–100% of cases. However, in some cases, serious complications can occur following PID. The risk of complications is higher when treatment is delayed. One study found that a three-day delay in treatment was associated with a more than two-fold increased risk of impaired fertility.
When PID is not treated, around 50% of women become infertile. The risk is higher in women who have experienced multiple episodes of PID. PID is also associated with an increased risk of:
- Ectopic pregnancy, experienced by about 9% of women with a history of PID;
- Dysmenorrhoea (period pain); and
- Chronic pelvic pain, the risk of which increases with increasing episodes of PID. After a single PID episode, 12% of women experience chronic pelvic pain, increasing to 30% amongst women who have experienced two episodes of PID, and 67% amongst those who have had PID three or more times in the past.
Treatment

Prescribing before PID is diagnosed definitively means that treatment is commenced earlier. However, doctors are still able to conduct tests which may diagnose other conditions that are causing the symptoms (e.g. ectopic pregnancy).
The types of antibiotics prescribed will depend on a number of factors, including:
- The suspected cause of PID, in particular whether or not it is caused by STI. STIs respond to different types of antibiotics than infections caused by bacteria which normally inhabit the vagina.
- The severity of the illness and symptoms;
- Characteristics of the woman, including allergies and pregnancy/breastfeeding status.
Antibiotics should begin to make you feel better within 72 hours. If you are not starting to feel better by then, you will need to go back to the doctor for further tests.
Referral to a specialist
You may be referred to a specialist if the doctor suspects complications, including:
- An abscess in the fallopian tubes or ovaries;
- Rupture of a mass in the ovaries;
- Adnexal torsion (torsion affecting one or both ovaries); or
- Perihepatitis meaning the pelvic infection is affecting the liver and causing it to be inflamed.
You may also be referred to a specialist for assessment if:
- You are pregnant;
- You have severe symptoms;
- The doctor remains uncertain whether PID or another condition is causing the symptoms, after doing tests. Some of the other conditions which have similar symptoms to PID (e.g. ectopic pregnancy) can be very dangerous to the woman’s life so it is important that the doctor is certain that such conditions are not causing the symptoms;
- You do not improve after taking antibiotics for 48 hours;
- You have trouble taking the antibiotic prescribed;
- Your immune system is compromised, for example because of medication use or AIDS.
Admission to hospital
Some women with PID are admitted to hospital so that they can be given antibiotics through an intravenous drip. This might occur if:
- You have severe PID symptoms, including:
- Symptoms that fail to improve after 2–3 days of antibiotic therapy;
- Severe nausea and vomiting or high fever;
- Unable to swallow antibiotics;
- You have a tubo-ovarian abscess;
- A surgical emergency cannot be excluded (e.g. if there is a possibility that the symptoms are caused by appendicitis or ectopic pregnancy);
- You are pregnant;
- You are HIV positive;
- You have difficulty taking your medicine as prescribed by the doctor.
Medicines

Usually several types of antibiotics are prescribed and the woman must take antibiotics for two weeks. Antibiotics that may be prescribed when STIs are the suspected cause include:
- Azithromycin;
- Doxycycline;
- Metronidazole;
- Ceftriaxone (when gonorrhoea is suspected or the symptoms are severe);
- Cefotaxime (when symptoms are severe);
- Cefoxitin (when symptoms are severe);
- Roxithromycin (when symptoms are severe);
When non-STI causes are suspected, antibiotics that may be prescribed include:
- Doxycycline;
- Metronidazole;
- Amoxycillin;
- Clindamycin (when symptoms are severe);
- Gentamicin (when symptoms are severe);
- Cefotetan (when symptoms are severe);
- Cefoxitin (when symptoms are severe).
If you are pregnant or breastfeeding, some of the medicines listed above are not safe. Instead you may be prescribed one or more of the following antibiotics:
- Amoxycillin plus clavulanate;
- Roxithromycin;
- Metronidazole;
- Amoxicillin.
You will probably need to take more than one antibiotic to treat PID. Usually you will need to take them every day for two weeks. Most antibiotics are prescribed as tablets which you swallow at the correct times, however if the symptoms are severe, you may be admitted to hospital so that the antibiotics can be administered intravenously. Always follow the doctor’s instructions carefully, ensuring you take the right amount at the right time/s of day until your complete the entire course.
The doctor may also provide painkillers to help relieve symptoms like lower abdominal pain. Medicine to prevent Candida infection (thrush) may be given to women who have a history of thrush while using antibiotics.
Treating sexual partners
If sexually transmitted organisms are suspected to have caused PID, it is very important that your sexual partners are also diagnosed and treated. They may also have the STI and if they do, they can pass it to you or their other sexual partners. Ideally, all the people you have had sex with in the six months preceding the onset of symptoms should be contacted. Health professionals can help if you are not able to contact sexual partners yourself.
It is very important that you do not have unprotected sex until both you and your sexual partner have finished taking all the medicine prescribed.
Surgery
Surgical treatment may be considered in severe cases with pelvic abscess (small pussy deposits caused by damaged tissues in the pelvis).
Women using an IUD for contraception
If you are using an IUD for contraception, the doctor may need to remove the IUD so that the treatment works properly. However, removing the IUD means you may become pregnant if you have had sex in the past seven days. The doctor may recommend you take an emergency contraceptive if your IUD is removed.
Women who are HIV positive
If you are HIV positive and are taking AIDS medication, the medication may interact with the medicines that treat PID. It is very important to let your doctor know that you are HIV positive and which medicines you are taking so that they can prescribe antibiotics that do not interact with your existing medication.
Information the doctor can provide
It is important that you understand how PID is treated and the complications that can arise from PID (e.g. infertility). Your doctor is a good source of information, so be sure to ask any questions you have about the disease when you are being treated.
The doctor may also explain to you:
- How the treatment works and the side effects it might cause;
- The importance of treating your sexual partners;
- How to avoid PID in the future. The best way is to use condoms everytime you have sex, or to only have sex with a partner you know does not have an STI.
Ask your doctor for written information about PID so you can refer to it once you get home.
Follow-up care
The doctor will probably ask you to come back for a checkup once you have completed the medicine. It is very important to go for a checkup, even if you feel well. If your medicines do not start to make you feel better within 48 hours, you must also return to your doctor.
More Information
 |
For more information on different types of sexually transmitted infections, prevention of STIs, treatments and effects on fertility, see Sexually Transmitted Infections (STIs). |
Pelvic Inflammatory Disease (PID) Prevention
Prevention and early treatment of STIs are the key preventative measure women can take to avoid PID. STIs can be prevented in the following ways:
- Abstinence from sexual intercourse;
- Having sexual intercourse within a mutually monogamous relationship, after both partners have been tested for STIs; or
- Using condoms consistently, every time you have sex.
 |
For more information, see Protecting against Sexually Transmitted Infections. |
If a woman contracts an STI, early treatment greatly reduces the risk of PID developing. As many STIs and particularly chlamydia may be asymptomatic, it is important to get screened for chlamydia if you have had unprotected sex. In Australia, doctors will screen for chlamydia if you ask them to. They may also recommend you screen for chlamydia if you have any of the following characteristics:
- You have been diagnosed with another STI;
- Your partner has been diagnosed with urethritis or another STI;
- You have a pap smear and the results indicate pelvic inflammation;
- You are < 25 years of age (as chlamydia is more common in young women);
- You have recent changed sexual partners;
- You do not consistently use condoms;
- You have an unplanned pregnancy;
- Your cervix is unusually positioned within your genital tract;
- You experience bleeding between menstrual bleeding;
- You experience deep period pain;
- You have a vaginal discharge;
- You experience pain when urinating.
In you are diagnosed with chlamydia, it is important that all your recent sexual partners are also checked for infection. The doctor can help you trace sexual partners if this will be difficult for you.
It is also important to avoid having sex until both you and your partner have been treated. You have been treated when you have finished taking all the medicines that the doctor prescribed for you.
You should also avoid having sex if you or your partner has any unusual genital symptoms such as itchy genitals or a discharge. Go to the doctor to have the symptoms checked as soon as possible. Do not have sex until you have been checked and (if necessary) treated.
References
- Pelvic inflammatory disease: Green-top guideline 32 [online]. London, UK: Royal College of Obstetricians and Gynaecologists; 17 November 2008 [cited 7 February 2010]. Available from: URL link
- Pelvic inflammatory disease: ACOG education pamphlet [online]. Washington, DC: American Congress of Obstetricians and Gynecologists; April 2010 [cited 31 January 2011]. Available from: URL link
- Ross J. Pelvic inflammatory disease. BMJ Clin Evid. 2008;322(7287):658. [Abstract]
- Skinner SR, Hickey M. Current priorities for adolescent sexual and reproductive health in Australia. Med J Aust. 2003;179(3):158-61. [Abstract | Full text]
- National management guidelines for sexually transmissible infections [online]. Melbourne, VIC: Sexual Health Society of Victory; 2008 [cited 21 January 2011]. Available from: URL link
- Dayan L. Pelvic inflammatory disease. Aust Fam Physician. 2006;35(11):858-92. [Full text]
- 2010 STD treatment guidelines [online]. Atlanta, GA: Centres for Disease Control and Prevention; December 2010 [cited 31 January 2011]. Available from: URL link
- Pelvic inflammatory disease (PID): Fact sheet [online]. Atlanta, GA: Centres for Disease Control and Prevention; 2010 [cited 20 November 2010]. Available from: URL link
- Pelvic inflammatory disease: Canadian guidelines on sexually transmitted infections [online]. Ottawa, ON: Public Health Agency of Canada; October 2007 [cited 31 January 2011]. Available from: URL link
- Parekh V, Devine B. How to treat: Pelvic inflammatory disease. Austr Doc. 2006;June:27-32. [Full text]
- Ross J, Phillippe J, Nilas L. European guideline for the management of pelvic inflammatory disease. Int J STD AIDS. 2007;18(10):662-6. [Abstract | Full text]
- Antibiotic treatment for pelvic inflammatory disease [online]. Perth, WA: King Edward Memorial Hospital, Women and Newborn Health Service; October 2007 [cited 1 March 2011]. Available from: URL link
- Ross J. United Kingdom national guideline for the management of pelvic inflammatory disease [online]. London: British Association for Sexual Health and HIV; 14 February 2005 [cited 2 March 2011]. Available from: URL link
- Kong FYS, Guy RJ, Hocking JS, et al. Australian general practitioner chlamydia testing rates among young people. Med J Aust. 2011;194(5):249-52. [Abstract]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.