- What is Marfan’s Syndrome
- Statistics on Marfan’s Syndrome
- Risk Factors for Marfan’s Syndrome
- Progression of Marfan’s Syndrome
- Symptoms of Marfan’s Syndrome
- Clinical Examination of Marfan’s Syndrome
- How is Marfan’s Syndrome Diagnosed?
- Prognosis of Marfan’s Syndrome
- How is Marfan’s Syndrome Treated?
- Marfan’s Syndrome References
What is Marfan’s Syndrome
Marfan’s syndrome is an inherited disorder of connective tissues within the body. It affects the skeleton, joints, eyes and cardiovascular structures. The skin and lungs are also frequently involved. The clinical expression of the disorder is largely variable and some patients may have marked abnormalities in one system (e.g. cardiovascular) with only minor changes in others (e.g. minimal skeletal changes). Two of the major systems must be involved to avoid over-diagnosis of the condition.
Abraham Lincoln was thought to have Marfan’s syndrome as he possessed many of the physical characteristics of Marfan’s. Patients with Marfan’s syndrome are usually tall, thin, with long arms, legs and fingers, and often scoliosis (curvature of the spine) and pectus deformity (abnormality of the chest wall).
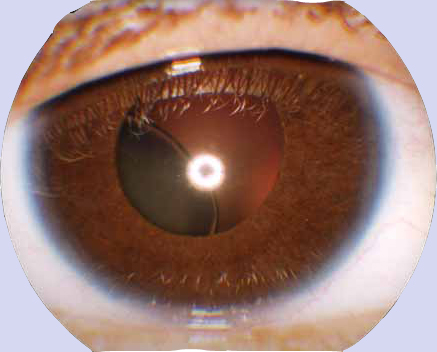
The image below is indicative of Lens subluxation associated with Marfan’s Syndrome.
Statistics on Marfan’s Syndrome
Marfan’s syndrome is one of the most common autosomal dominant inherited disorders of connective tissue. It is thought to affect approximately 1 in 5000 people worldwide, most of who get the disorder passed on from their family. However, around 25% of individuals have no family history and develop the disorder from random mutations in the particular genes. These latter cases are more severely affected.
Risk Factors for Marfan’s Syndrome
Marfan’s syndrome arises from a mutation in a gene that codes for a protein called fibrillin, which forms the structural components of connective tissue in the aorta, joint ligaments and in the eye. Abnormal fibrillin in reduced integrity of these structures.
Progression of Marfan’s Syndrome
As fore mentioned, Marfan’s syndrome develops due to an inherited or random mutation in the gene coding for fibrillin which is important in maintaining the structure of connective tissues within the body. When this is abnormal there are progressive changes in some of the tissues such as gradual dilation of the aorta (the major blood vessel leaving the heart to supply the rest of the body). Approximately 80% of patients will develop aortic complications. The lens of the eye, ligaments and airways also gradually lose their integrity.
Patients may be diagnosed with Marfan’s at birth, during childhood or later in life. The more severe cases are usually diagnosed early. Many patients present with features such as tall stature and an arm span that exceeds height. However, lens dislocation, aortic dilatation or skeletal manifestations (such as pectus deformities or scoliosis) may also be the first presentation. Many of the manifestations of the disease change with age so diagnosis can be difficult in children. Marfan’s syndrome causes a host of physical abnormalities but is not thought to affect inteligence.
Patients with Marfan’s are at increased risk of early cardiovascular death from aortic aneurysms (dilations) and dissection (splitting of the wall). Family history of these complications, male sex and extreme physical characteristics are associated with higher cardiovascular risks. If you suffer this disorder you will be advised to make several lifestyle changes to reduce your risk.
Symptoms of Marfan’s Syndrome
If you are suspected to suffer from Marfan’s syndrome, your doctor will take a detailed history of your presenting symptoms to determine whether the appropriate organ systems are involved. Of extreme importance is whether any of your family members have been diagnosed with this disorder or have had cardiovascular problems at a young age. Any results you have from any genetic testing provide very useful information to your doctor.
If you suffer Marfan’s syndrome you may have noticed the following features:
- Delayed gross and motor development due to laxity of ligaments.
- You may have been diagnosed with a murmur previously.
- Abnormal heart rhythms.
- Sudden onset of thoracic (chest) pain due to aortic dissection.
- Lower back pain- Possibly with burning, numbness or weakness in the legs due to an abnormality of a membrane lining the spinal canal. This can also cause headaches and other neurologic deficits.
- Joint pain in adults.
- Shortness of breath, palpitations and substernal pain in severe pectus excavatum (deformity of the chest wall).
- Visual problems or loss of vision due to lens dislocation or retinal detachment.
Clinical Examination of Marfan’s Syndrome
The diagnosis of Marfan’s is largely clinical and relies on your doctor carefully examining your cardiovascular system, eyes, lung, skin and skeletal system. The latter two examinations may be done by a clinical geneticist who has a speciality in that field.
Skeletal abnormalities are usually the most obvious feature of Marfan’s. Individuals are typically exceptionally tall, with long arms and legs, and elongated tapering fingers and toes. The ligaments in hand and foot joints are lax, and individuals may appear to be double jointed due to the increased joint mobility. A number of spinal abnormalities may be present, including kyphosis (increased outwards curvature of the spine) or scoliosis (sideways curvature of the spine). There maybe also be abnormalities of the chest wall, which may be depressed inwards (pectus excavatum) or outwards (pectus carinatum).
Eye changes may also be present. Most common is dislocation of the lens in both eyes (ectopia lentis). This is very uncommon, and if present should raise the suspicion of Marfan’s.
The most serious manifestation of Marfan’s are heart complications. Dilatation of the aorta (widening and structural weakening of the aorta) may occur, increasing the risk of an aortic dissection – a rupture through the aorta causing massive haemorrhage. This the cause of death in 30-45% of individuals with Marfan’s. The heart valves may also be affected. Deficient connective tissue support results in floppy valves, which may predispose to heart failure. An abnormal heart rhythm may be present.
Other features include striae, or stretch marks, hernias (part of the intestine protruding through a weakened part of the abdominal wall), and lung complications.
How is Marfan’s Syndrome Diagnosed?
A number of tests are usually performed to diagnose Marfan’s syndrome:
- Molecular and genetic studies of the fibrillin gene.
- Chest x-ray which can show lung, spine or heart abnormalities. X-rays of the spine are also important in the diagnosis of scoliosis.
- Echocardiography (heart scan) to examine the heart structures.
- MRI scan if aortic rupture is suspected or to examine for dural ectasia (damage to one of the membranes lining of the spinal cord).
- Electrocardiogram (ECG) to examine heart activity, as 40% of patients have abnormal heart rhythms.
- Blood pressure.
- Eye examination to check for lens dislocation and retinal tears.
Prognosis of Marfan’s Syndrome
The prognosis of Marfan’s largely depends on the severity of the complications previously mentioned and the degree of progressive aortic dilation which can lead to death at a young age. However, the life expectancy for patients with Marfan’s has improved over time, presumably due to improved detection and intervention, including surgical procedures and the use of beta-blockers. The average lifespan is now approximately 70 years.
How is Marfan’s Syndrome Treated?
Education in the form of genetic couselling is particularly important for families with Marfan’s as there is a 50% chance of one affected parent passing the disease on to their child. If you or a family member are diagnosed with Marfan’s syndrome you will likely be referred to a genetic counsellor or clinical geneticist for information regarding your disorder and screening programs. All close family members may be offered testing for the gene involved and be screened on a yearly basis for the development of clinical features. I
Patients with Marfan’s are advised to avoid strenous activities and contact sports due to risk of cardiac complications. Highly competitive sports por those involving isometric work such as weightlifting, climbing steep inclines, gymnastics, and pull-ups should be avoided due to risks of increased blood pressure and sudden death. Nonstrenuous activities and sports (such as golf, walking, fishing) are recommended. It may also be necessary to change your job to a more sedentary one as you may find yourself easily fatigued or the visual and painful skeletal changes may limit your work.
Some patients may require cardiac surgery which can prolong and improve quality of life. Surgery may be performed on the aorta either under emergency or preventative circumstances. Surgery may also be helpful for improving chest wall deformities, severe scoliosis and repairing detached retinas. An orthopaedic surgeon and ophthalmologist will be involved in your long-term care.
Patients with Marfan’s are usually given medications (long-term) to help lower the risk of cardiac complications. The main class of drugs used are called beta-blockers which reduce the dilation of the aortic root. Long term monitoring of cardiac complications is also required, including blood pressure checks and regular echocardiography. Your cardiologist will determine the frequency of these visits that is suitable for you depending on the severity of your condition. However, patients are usually followed up every six months to one year.
Marfan’s Syndrome References
- Chen H. Marfan Syndrome. eMedicine. Web MD 2006. Available [online] at URL: http://www.emedicine.com/ped/topic1372.htm
- Cotran R, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- Kumar, Clark. Clinical Medicine. 5th Edition. Saunders. 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. 2004.
- Murtagh J. General Practice, 3rd Ed. McGraw-Hill, Australia, 2003.
- Summers K, West J, Peterson M, Stark D, McGill J, West M. Challenges in the diagnosis of Marfan syndrome. MJA 2006; 184 (12): 627-631.
- The Cardiac Society of Australia and New Zealand. Guidelines for the Diagnosis and Management of Marfan’s Syndrome. 2005. Available [online] at URL: http://www.csanz.edu.au/guidelines/practice/Marfans_Diagnosis_and_Management_2005.pdf
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







