- What is Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- Statistics on Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- Risk Factors for Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- Progression of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- Symptoms of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- Clinical Examination of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- How is Bladder Cancer (Squamous Cell Carcinoma of the Bladder) Diagnosed?
- Prognosis of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
- How is Bladder Cancer (Squamous Cell Carcinoma of the Bladder) Treated?
- Bladder Cancer (Squamous Cell Carcinoma of the Bladder) References
What is Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
Squamous Cell Carcinoma of the Bladder is a rarer type of bladder cancer. The majority of bladder cancers are transitional cell carcinomas that arise in the urinary tract epithelium and can also occur in parts of the kidney, ureter and urethra (tubes carrying urine from the kidney and urinary bladder respectively). The bladder functions as a waste storage system for urine. Urine is produced by the kidneys as they filter the blood. The urine then travels down the ureters into the bladder. The bladder expands and once it reaches a certain maximum volume, the urge to pass urine increases until urine is passed. The bladder is made up of an elastic type tissue which contains a layer of muscle. The bladder is lined with epithelium called transitional cells which are tall, thin cells that protect the underlying bladder from the urine contained therein. Because the bladder is lined with transitional epithelium, the usual type of cancer affecting the bladder is transitional cell carcinoma. However, in response to chronic irritation the epithelial lining of the bladder can gradually change to squamous (similar to the skin). With further exposure to irritative or carcinogenic agents – bladder cancer can develop.
Statistics on Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
Bladder cancer on the whole is the most common malignancy affecting the urinary system. The majority of cases are transitional cell carcinomas affecting the tall epithelial cells lining the bladder. Squamous cell carcinoma accounts for only 3 to 7% of bladder cancers in Western countries, but in certain countries where parasites are very common (especially schistosomiasis) it is found much more frequently. The parasites cause chronic irritation of the bladder causing the cells to change their shape to try to protect the bladder. Over time the cells can change to become neoplastic or cancerous. In these countries up to 70% of bladder cancers are the squamous type. The incidence of bladder cancer increases with age and 80% of patients are found to be between 50 and 80 years. Men: bladder cancer is much more common in men and is the fourth most common cancer. In Australia approximately 554 men die from bladder cancer each year. However, squamous cell carcinoma accounts for only a small percentage. Women: Bladder cancer is the tenth most common cancer in women. Approximately 250 Australian women die from bladder cancer each year. However, squamous cell carcinoma accounts for only a small percentage.
Risk Factors for Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
bladder cancer is almost exclusively found in bladders exposed to chronic irritation and infection. It is primarily a bladder disease of developing countries and is twice as common in white people compared to blacks. In African countries, Schistosoma haematobium is a parasitic infection of the bladder transmitted by freshwater snails and is acquired when people bathe in slow-moving freshwater rivers and lakes. The eggs of the parasite cause chronic inflammation of the bladder and ureters – and more frequently leads to obstructive kidney disease, but can also cause bladder cancer. In the United States chronic inflammation of the bladder is more often due to long-term indwelling urinary catheters or other instrumentation, and bladder stones.
Progression of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
Bladder cancer initially spreads to involve larger areas of the mucosa of the bladder, with deeper invasion later. Finally metastatic spread to other organs via the blood stream and lymphatics can occur. At the time of discovery most bladder tumours are deeply invasive.
Symptoms of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
Bladder tumours classically present with painless haematuria (blood in the urine). They can also present with symptoms simulating urinary tract infections such as frequency, dysuria, urgency. Blood in the urine does not always indicate bladder cancer, and cystitis (inflammation of the bladder) is a much commoner cause. However, all patients should be assumed to have cancer (and be appropriately investigated) until proven otherwise. Pain can also result from local nerve involvement. If a ureter is obstructed patients can also develop pyelonephritis (inflammation of the kidney and its pelvis with fever and flank pain) or hydronephrosis (obstruction and dilation of the upper urinary tract).
Clinical Examination of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
With bladder cancer there is normally little to find on examination, unless the bladder tumour is widespread. Your doctor will carefully examine your abdomen, pelvis and urinary tract. Haematuria (blood in the urine) may be obvious on urinary examination, or microscopic haematuria (only visible under the microscope) on urinalysis may be the only sign in 2% of incidents. Visit our information on Anatomy and Physiology of the Renal System.
How is Bladder Cancer (Squamous Cell Carcinoma of the Bladder) Diagnosed?
Bladder cancer investigations tend to involve basic blood tests such as FBP (full blood picture) which may reveal anaemia due to chronic blood loss. A mid-stream urine sample (MSU) may reveal red blood cells or malignant cells. Imaging of the urinary tract will be preformed such as Ultrasound and intravenous pylogram followed by CT and/or MRI. These rule out pathology in other parts of the urinary tract and can be used to visualise the urothelium. Cytoscopy (visualisation of the bladder with a camera) and biopsy are important investigations to obtain a tissue daignosis.
Prognosis of Bladder Cancer (Squamous Cell Carcinoma of the Bladder)
Bladder cancer generally has poorer prognosis than transitional cell carcinoma. The reason for this is probably that most bladder tumours are discovered late. The bladder cancer prognosis hence depends on the stage of the bladder tumour at the time of bladder cancer diagnosis. Women tend to have a poorer bladder cancer prognosis than men.
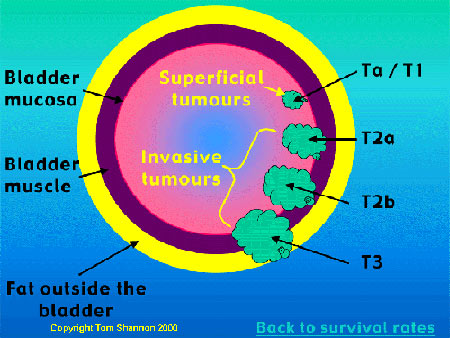
Image courtesy of Mr. Tom Shannon (MBBS, FRACS). Click here to visit Mr. Shannon’s external site, Hollywood Urology.
How is Bladder Cancer (Squamous Cell Carcinoma of the Bladder) Treated?
Bladder cancer treatment options depend on the stage of the cancer. Surgical resection of part of the bladder, or the whole bladder (radical cystectomy) may be performed with curative intent in early bladder cancer. Radical cystectomy is a major procedure and is usually reserved for cases where more conservative approaches are not likely to succeed and a cure is possible. A conduit or reservoir (using ileum- the final segment of the small intestines) can then be fashioned, which connects the ureters to the ileum or the urethra, or the anterior abdominal wall for the drainage of urine. A uretero-ileal conduit is the more widely used. In males radical cystectomy also involves removal of the bladder, prostate, seminal vesicles, and proximal urethra, and often causes impotence (erectile dysfunction) post-surgery unless the nerves responsible for erectile function are preserved. In females radical cystectomy includes removal of the bladder, urethra, uterus, fallopian tubes, ovaries, anterior vaginal wall, and surrounding fascia. Local (intravesical) or systemic chemotherapy and/or radiotherapy can also be used for bladder cancer treatment. Chemotherapy protocols include:
- MVAC- a combination of 4 drugs: Methotrexate (IV days 1,15,22), Vinblastine (IV days 1,15,22), Doxorubicin (IV day 2) and Cisplatin (IV over 2 hours day 2). Cycle is repeated every 28 days.
- For bladder cancer patients unlikely to tolerate MVAC because of renal function, age or performance status: Cisplatin (day 1) and Gemcitabine (days 1+8) are used.
- Concomitant chemotherapy/radiotherapy: with Cisplatin (5days) and Normal Saline hydration for the first and fourth weeks of radical radiation.
Bladder Cancer (Squamous Cell Carcinoma of the Bladder) References
- AIHW, Cancer Survival in Australia 2001. Australian Institute of Health and Welfare and Australasian Association of Cancer Registries 2001, Canberra, AIHW cat. no. CAN 13.
- Bochner B, Epidemiology and etiology of bladder cancer, UpToDate, 2005.
- Braunwald, Fauci, Kasper, Hauser, Longo, Jameson. Harrison’s Principles of Internal Medicine. 15th Edition. McGraw-Hill. 2001.
- Cotran RS, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- Kumar, Clark. Clinical Medicine. 5th Edition. Saunders. 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. 2004.
- Steinberg G, Kim H, Bladder cancer, eMedicine, Web MD, 2005. Available [online] at URL: http://www.emedicine.com/med/topic2344.htm.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







