Abscesses are localised collections of pus contained within a cavity. Pus itself is a mixture of bacteria (bugs), dead cells and proteins secreted by neutrophils (a type of immune cell that fights infection). Abscesses can occur at various sites within the abdominal cavity when infection or inflammation occurs. Abscesses are part of the body’s immune response to trap nasty bacteria within a cavity so they cannot spread to the rest of the body. The most common type of abscesses in the abdomen are intra-peritoneal abscesses. This means they are contained within the space between the two layers of peritoneum and the abscesses lie within the space between the organs and abdominal wall. These abscesses often occur due to bowel perforations where the contents of the bowel (including the normal bacteria) leak into the abdominal cavity. Leakage can also occur following bowel surgery if the two ends of bowel are insufficiently reconnected. Abscesses can also occur actually in the organs or muscles.
Abscess Definition
An abscess is a localised collection of pus contained within a cavity. Pus is a mixture of dead and dying inflammatory cells called neutrophils, combined with special protein fluids secreted by cells to try and kill of bugs. Abscesses contain dead tissue in the centre and are surrounded by a fibrous capsule or case. This capsule ensures that the infection cannot spread to other parts of the body. However, it can be difficult to treat abscesses because antibiotics also have trouble crossing this fibrous layer. Abscesses can occur virtually anywhere within the body but only those occurring within the abdomen are discussed in this article. These often contain a mixture of bacteria which means they can be harder to treat. The most common organism involved is the bacteria called Bacteroides fragilis which makes up a small percentage of the normal bowel flora. Intra-abdominal abscesses often develop secondary to peritonitis an infection of the serous membranes lining the abdominal organs and walls.
The different types of abscesses are listed below:
Sub-phrenic abscess
This is a collection of pus below the diaphragm (the muscular organ separating the abdominal cavity from the chest cavity). It is often caused by rupture of the gallbladder that causes fluid to build up under the diaphragm. Abscesses at this location are close to the lungs so can cause basal lung infections. In addition, shoulder tip pain is a common feature of these abscesses. The image below shows two large abscesses (arrows) situated below the right side of the diaphragm. (CT image shows a cross-section through the abdomen, looking from below). The abscesses have well-defined margins of connective tissue with semi-dense pus in the cavity. These abscesses are most likely secondary to gall bladder perforation.
Intra-peritoneal abscess
This is an abscess within the peritoneal cavity due to an infection of free fluid, bile or blood. Often these abscesses are the result of bowel perforation or a complication of bowel surgery. Spillage of feacal material from an inflamed appendix frequently causes this type of abscess.
Visceral abscess
Abscesses are also found on the surface or within gastrointestinal organs. Liver abscesses are the most common and account for approximately half of all visceral abscesses. These may cause pain in the right upper part of the abdomen. Pancreatic abscesses occur as a late complication of acute pancreatitis. Pancreatitis causes severe central abdominal pain that spreads to the back. Early recognition and treatment of this disorder will prevent abscesses forming. Abscesses of the spleen are rare but can occur if this organ is damaged or if there is an infection in the blood. Patients with immune disorders or the sickle cell trait are at greater risk. Abscesses in or near the kidneys are quite rare but can occur due to the spread of infection up the urinary tract from a urinary tract infection. The CT image below demonstrates a large abscess within the liver.
Pelvic abscess
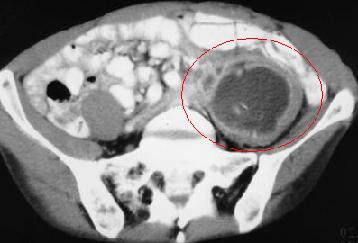
Pelvic abscesses car occur secondary to the same conditions that cause intra-peritoneal abscesses if the pus and fluid tracks downwards into the pelvis. In addition, gynaecologicalinfections can cause pelvic abscesses. The image below shows CT findings of a pelvic abscess causes by appendicitis. Pelvic abscesses can cause symptoms of frequent urination, diarrhoea or tenesmus (a sensation of incomplete bowel emptying). If symptoms are mild, pelvic abscesses do not require treatment as they often self resolve on their own by draining out the rectum.
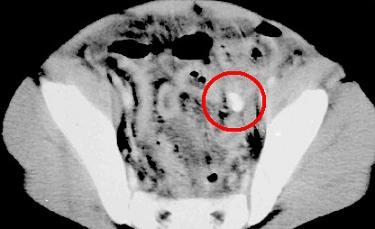
Psoas abscess
The psoas muscle is a large muscle running alongside the spine which crosses the pelvis. It helps bend the hip so your doctor may do tests to see if hip flexion is painful to make this diagnosis. Clinical signs of back pain or pain during flexion of the hip can help doctors make the diagnosis early by triggering them to perform imaging such as CT (as displayed below) or MRI. Abscesses occur in the psoas muscle when infections spread in the blood or from local organs of the abdomen or pelvis. In addition, infections in the bones of the spine (osteomyelitis) can cause psoas abscesses.
Anorectal abscess
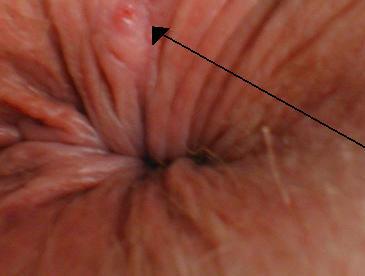
The anus and rectum (which form the back passage) are other common sites of abscess formation worth separate mention. Anorectal abscesses are more common in men and often develop from anorectal fistulas or sexually transmitted infections. They present as painful, tender swellings and are easily accessible for surgical treatment. The image below shows a magnified view of a perianal abscess on the skin
surrounding the anal opening. This should be picked up by your doctor on careful examination of the anus and rectum.
Causes of abscesses
As previously mentioned, abdominal abscesses are caused by various infectious organisms within the abdomen. They develop as the body’s immune system attempts to treat the infection and prevent it from spreading. Intra-abdominal infection (peritonitis) quite commonly is the source of an abscess but infections can also seed from organs or via the bloodstream.
Some common causes of abdominal abscesses are listed below:
- Bowel perforation- often due to an underlying disease process or weakness. This includes peptic ulcer perforation. Diverticular disease, colonic tumours and inflammatory bowel disease can also predispose to infection and ruptures.
- Ruptured appendix or gallbladder due to inflammation or infection within these organs. Infection of virtually any abdominal or pelvic organ may lead to local abscess formation.
- Abdominal trauma or injury.
- Bowel surgery- Faecal contamination of operation sites or leakage of bowel contents post-operatively due to poor re-anastomosis (connection of segments) often lead to abscess formation.
Signs and symptoms
The clinical presentation of abdominal abscesses is highly variable. If you have an abscess it is likely you will have constant abdominal pain and a spiking fever. You will have cycles of feeling hot and cold which is an important sign doctors look for to diagnose this condition. Blood tests will show that you have lots of white blood cells which increase to try to fight the infection. You may also have changes in bowel function such as diarrhoea or obstruction. If your abscess is deep within an organ, the classic signs may not be present. It can also be difficult for doctors to diagnose abscesses instead of other disorders such as pancreatitis. Your doctor will feel your abdomen to detect any areas of tenderness or masses. Generally the site of pain corresponds well with the location of the abscess. If you have an associated peritonitis your abdomen will be markedly tender and may stiffen up like a board. Your doctor may also like to perform a rectal examination. For this they insert a gloved finger gently into the back passage to see if they can feel any hot and tender masses. You will also be examined in general to make sure you are not too sick or dehydrated. If you develop an abscess following an operation it can be very hard to diagnose because the pain killers and antibiotics you would be taking can mask some of the symptoms. Doctors must have a high index of suspicion for this disorder to make sure it doesnt get missed. Sometimes the doctor will need to perform investigations to confirm the site and size of an abdominal abscess. These may include:
- Abdominal ultrasound– Reasonably reliable and safe test.
- CT– A very accurate test that will find most abscesses.
- Radioisotope scanning using white blood cells labelled with special radioactive substances that localise in the abscess. These are however very time consuming so will only be used if other investigations are negative but it is still thought there is an abscess.
- Plain abdominal x-rays have little diagnostic value and often highlight the need for further investigation.
Management
The underlying principal for management of abscesses involves incision and drainage, which is cutting them open to allow the pus to drain. In many cases this can be performed as a procedure through the skin. Ultrasounds or CT scans can be used by the treating doctor to guide the needle into the right spot. Occasionally the abdomen will need to be cut open (laparotomy) to allow the abscess to be drained. Some types of abscesses in the pelvis, below the diaphragm or associated with diverticuli may resolve on there own without any surgical treatment. In general, if surgery is performed it is expected that your symptoms will resolve within three days. Failure to do so may indicate incomplete drainage or alternative sources of infection. In addition to surgery you are likely to receive antibiotic therapy that covers a broad range of bugs. Once the abscess is drained the pus can be examined under a microscope and cultured so the specific bug(s) involved can be identified. At this stage your doctor may need to change your antibiotics to make sure they will kill the bug involved. In most cases your symptoms will improve rapidly and you will have no long term consequences from the abscess.
References
- Burkitt, Quick. Essential Surgery. 3rd Edition.Churchill Livingstone. 2002.
- Cotran R, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- Kasper D, Zalenzik D. ‘Intra-abdominal Infections and Abscesses’ in Kasper et al. Harrison’s Principle of Internal Medicine, 16th Edition (Chpater 112). McGraw-Hill, 2006.
- Kumar, Clark. Clinical Medicine. 5th Edition. Saunders. 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. 2004.
- Saber A, LaRaja R. Abdominal abscess. eMedicine. Web MD, 2006. Available at URL: http://www.emedicine.com/med/topic2702.htm.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







