- What is Pressure Ulcers
- Statistics on Pressure Ulcers
- Risk Factors for Pressure Ulcers
- Progression of Pressure Ulcers
- Symptoms of Pressure Ulcers
- Clinical Examination of Pressure Ulcers
- How is Pressure Ulcers Diagnosed?
- Prognosis of Pressure Ulcers
- How is Pressure Ulcers Treated?
- Pressure Ulcers References
What is Pressure Ulcers
Pressure ulcers occur when an area of skin breaks down when you stay in one position for too long, most commonly involving bony areas such as around the heels, hips, elbows and back. People who are exposed to developing pressure ulcers include: those who are in a wheelchair or are bedridden (eg after surgery or injury), the elderly and if you are unconscious and stay in a particular position for a long period of time. The constant pressure produced against the skin reduces the blood supply to that area, and the affected tissue dies.
Common sites for pressure ulcer development include:
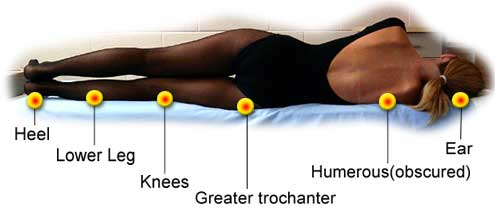
Lateral position
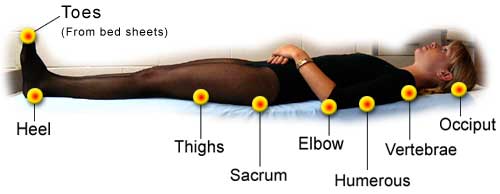
Supine position
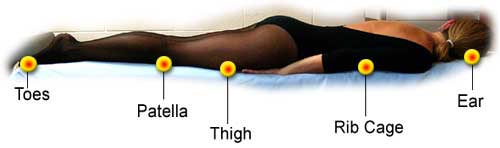
Prone position
Many factors are important in contributing to the formation of pressure ulcers, including:
- pressure
- friction
- shearing forces
- moisture
Pressure
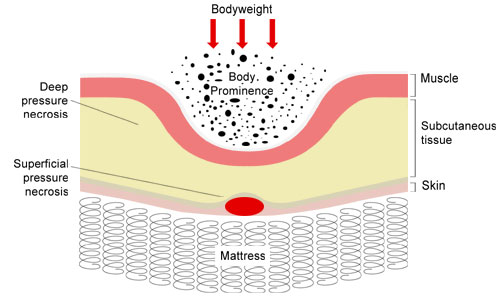
Pressure is one of the most important external factors that contributes to the development of pressure ulcers. When tissue becomes caught between two hard surfaces, cells are deprived of oxygen and nutrients and waste products build up within the cells. If the pressure is relieved to the tissues the blood supply is returned to the area, thus oxygen and nutrients are returned to the cells and waste products are removed. If this pressure is not relieved, death of tissues will occur resulting in destruction of the tissues.Pressure ulcers usually start as areas of red skin that can deteriorate to form blisters and deeper sores. To demonstrate the effects on pressure on healthy skin, we asked our medical model to lay on her side on the floor for five minutes. The images below show the reddened areas of skin over her upper arm and thigh.
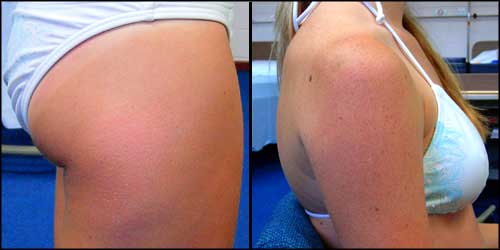
You may be able to note the affected area more easily on the thigh than on the arm (probably because the arm is more pigmented from sun exposure than the thigh). Here are the same two pictures, with the reddened areas highlighted:
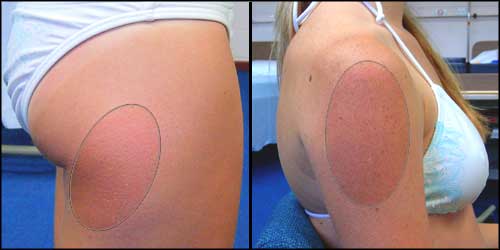
Friction
This occurs when two surfaces rub together. An example of friction is when we move up and down in bed, with our skin rubbing against the sheets. Friction may remove the superficial skin layers, making the skin more prone to breakdown.
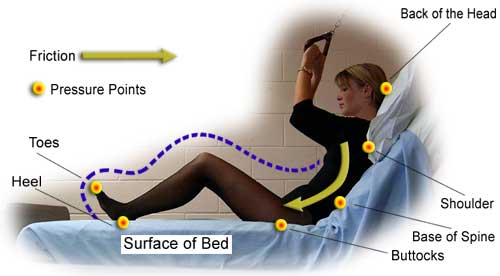
Shearing
A shearing injury occurs when there are two forces pulling in different directions.
Important sources of shearing injury are:
- dragging or sliding a patient across the bed
- raising the head of the bed more than 30 degrees.
Statistics on Pressure Ulcers
The majority of pressure ulcers occur in patients in hospital. Around seventy percent occur in the first two weeks of hospitalization and seventy percent of these are seen in patients admitted for problems with the bones (orthopedics). About twenty – thirty percent of pressure ulcers occur in the community.
Risk Factors for Pressure Ulcers
There are many factors that can put you at a higher risk for developing pressure ulcers. These include:
- Being unable to move certain parts of your body properly.
- Paraplegia
- Severe physical disease
- Arthritis
- Surgery and post operative states
- Intensive care
- Plaster casts
- Decreased sensation (feeling in the limbs)
- Neurological disease
- Diabetes
- Coma
- Disease of the vessels: these diseases prevent areas of the body from receiving proper blood flow.
- Atherosclerosis
- Diabetes
- Vasculitis
- scleroderma
- Inadequate nutrition
- Anaemia(low levels of red blood cells)
- Hypoalbuminaemia (low levels of albumin, a protein produced by the liver).
- Vitamin C / Zinc deficiency
Progression of Pressure Ulcers
For pressure ulcers to develop, there must be both forces applied to the skin from the outside, plus predisposing factors that you may have, interacting to produce tissue damage. Factors from the outside environment that can lead to development of pressure ulcers include: increased pressure, rubbing (friction), shearing forces and prolonged areas of wetness. These are described in the introductory section. Factors that you may have contributing to development of ulcers include: inability to move properly, poor nutritional status, poor blood supply to various body areas, incontinence (inability to retain urine or faeces), and diseases affecting the neurological system.
Symptoms of Pressure Ulcers
When you visit the doctor, he or she may ask the following questions, as they see necessary.
- Have you been immobile for long periods of time?
- Are you unable to move certain parts of the body / are there any physical disabilities?
- Are there any problems with your nervous system?
- Can you tell me more about the ulcer – when did it first start, how long has it been there, are there any other ulcers on the body, have you received any treatment for it?
- Who do you live with at home? Do you have enough support? What is your bed like?
- Are there any other symptoms you are experiencing – fevers, sweats, loss of appetite, loss of weight, weakness in any parts of the body?
Clinical Examination of Pressure Ulcers
When your doctor examines you, he or she may look for the following features.
- Where specifically is the ulcer located on the body?
- Are there any signs of infection – redness, foul smell, discharge?
- How deep does the ulcer extend into the tissues?
- They may also look at the base of the ulcer to see if there are any changes occurring such as formation of healing cells and tissues.
How is Pressure Ulcers Diagnosed?
The doctor may decide to do some of the following tests, to help determine the reason for your pressure ulcers.
- If there are signs of infection, a wound swab may be performed.
- If you may have diabetes, a blood glucose level can be obtained.
- If you may have anaemia, blood can be taken to determine the level of red blood cells in the bloodstream.
- If the doctor suspects zinc or vitamin C deficiency, he or she may test you for these levels.
Prognosis of Pressure Ulcers
The outcome of patients with pressure ulcers largely depends upon the extent of their disease and the staging of ulcers present. Pressure ulcers may be associated with both medical and psychosocial (emotional and social) complications. The medical complications are potentially life threatening and can include infection, which may lead to bacteria entering the bloodstream. Psychological complications you may experience include feeling depressed and having decreased self esteem, due to the presence of pressure ulcers.
How is Pressure Ulcers Treated?
Prevention of pressure ulcers is better than cure. However, once a pressure ulcer is identified, the following steps can be taken:
- Relieve the pressure on that area. Use soft pillows, cushions, and other supports to reduce the pressure.
- Pressure relieving mattresses and beds should be used.
- Depending on the stage of the ulcer, your doctor will give you further treatment and care instructions. This can involve instructions on how to clean and care for the ulcers.
- The ulcer may need to be covered with a special dressing to prevent complications such as infection.
- You should try and improve nutrition and other underlying problems that may affect the healing process.
- Any further trauma or friction should be avoided.
Pressure Ulcers References
- Glass R, Lynm C, Zeller J. Pressure Ulcers. JAMA. 2006;296:1020
- Kumar P, Clark M. Clinical Medicine United Kingdom: WB Saunders; 2002.
- Margolis D, Knauss J, Bilker W, Baumgarten M. Medical conditions as risk factors for pressure ulcers in an outpatient setting. Age and Ageing 2003; 32: 259-264
- Resnick N, Dosa D. Harrisons Principles of Internal Medicine; Management of Common Geriatric Conditions. USA: The McGraw-Hill Companies; 2006
- Wilhelmi B, Neumister M. Pressure Ulcers, Surgical Treatment and Principles. E-medicine [serial online].2006 [cited 20th July 2006].
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







