- What is Placenta Praevia?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- References
What is Placenta Praevia?
Placenta praevia occurs when the placenta is situated wholly or in part into the lower segment of the uterus and is located close to the opening of the cervix. Clinically this is important as it can give rise to bleeding either during pregnancy, during labour or following delivery.
Statistics
Placenta praevia complicates approximately 1 in 200 pregnancies. The incidence has increased over time due to the rising incidence of caesarean section, which is a risk factor, and improved diagnostics. While abruption can occur in women with no risk factors, there are factors, listed below, that increase the risk of a mother experiencing placental abruption.
Risk Factors
The cause of placenta praevia remains unknown, however risk factors include:
- High parity
- Increased maternal age
- Uterine abnormalities
- Smoking
- Cocaine use
- Multiple pregnancy
- Previous placenta praevia
- Caesarean section
- Termination of pregnancy
- Intrauterine surgery
- Assisted reproductive techniques (in vitro fertilisation and intracytoplasmic sperm injection)

Progression
The lower uterine segment only develops fully in the third trimester. This means that prior to the third trimester many placentas may appear to be located close to the cervix and are termed low lying placentas. However, as the pregnancy progresses and the lower segment develops fully, a large number (>90%) of low lying placentas detected in early pregnancy move away from the cervical opening.
Symptoms
Classically patients present with an unprovoked, painless episode of vaginal bleeding. The amount of vaginal blood loss varies between minor to massive haemorrhage. Blood loss is most frequently intermittent with unpredictable recurrence.
Following an episode of bleeding, it is most likely that you will need to stay in hospital for a period of time so that both you and your baby can be monitored closely.
Clinical Examination
Other than your health, they will also be concerned with the health of your unborn child. They will be interested in if your baby is moving, its heart rate and how many weeks gestation your baby is. If there are any signs of foetal compromise, active bleeding, uterine activity or tenderness a cardiotocograph (CTG) will be applied for continuous monitoring.
Several blood tests will be ordered and an ultrasound may be necessary.
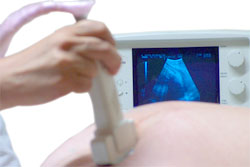
How is it Diagnosed
Placenta praevia is diagnosed using ultrasound. The most accurate method for diagnosing placenta praevia is by trans-vaginal ultrasound. This involves the insertion of the ultrasound probe into the vagina. Ultrasound using a probe over the abdomen (trans-abdominal) can be performed, however, this method is more likely to incorrectly identify cases of placenta praevia compared to trans-vaginal ultrasound.
Prognosis
For those women in which this does not occur, placenta praevia can be responsible for bleeding from the vagina either during pregnancy, during labour or following labour. This may result in anaemia, hysterectomy, a blood transfusion and/or possible infection. In the Western world, placenta praevia is a rare cause of maternal mortality, approximately 0.03%.
Foetal death is slightly higher than maternal mortality, approximately 4-8%, and is associated with pre-term birth (50%) and intrauterine growth restriction. While the cause is unknown, the risk of birth defects in the foetus are doubled.
Treatment

If the bleeding becomes life threatening, resuscitation and stabilisation of the mother is the primary focus followed by delivery of the baby by emergency caesarean section.
In cases where the foetus is pre-term and the bleeding is minimal, the goal is to delay the delivery to allow for maturation of the foetus without increasing the risk to the mother. In most cases this will involve admission to hospital where you and your baby can be monitored closely. Unless there is spontaneous labour of heavy sustained bleeding necessitating emergency caesarean delivery, delivery is by planned caesarean section at 37-38 weeks gestation.
References
- Baskett TF. Essential management of obstetric emergencies. 4th ed. 2004. Clinical Press Limited, Redland, Bristol.
- Sinha P, Kuruba N. Ante-patum haemorrhage: an update. Journal of Obstetrics and Gynaecology 2008; 28: 377-81.
- Benirschke K, Kaufmann P. 2000. Pathology of the human placenta. 4th ed. New York: Springer.
- Lam CM, Wong SF, Chow KM, Ho LC. 2000. Women with placenta praevia have a worse outcome than those who do not bleed before delivery. Journal of Obstetrics and Gynaecology 20:27-31.
- Crane JM, Vanden HofMC, Dodds L, Armson A, Liston R. 1999. Neonatal outcomes with placenta praevia. Obstetrics and Gynecology 93:541-4.
- Baker PN (Ed). Obstetrics by ten teachers. 18th ed. 2006. Edward Arnold, New York, New York.
- KEMH clinical guidelines B 2.3.1.1 MFAU Quick reference guide to APH. February 2009. Available from: < http://www.wnhs.health.wa.gov.au/development/manuals/O&G_guidelines/sectionb/2/b2.3.1.1.pdf> [18 September 2009].
- KEMH clinical guidelines B 2.3.1 Management of a woman with an APH. April 2009. Available from: < http://www.wnhs.health.wa.gov.au/development/manuals/O&G_guidelines/sectionb/2/b2.3.1.pdf> [18 September 2009].
- Wing DA, Paul RH, Millar LK. 1996. Management of the symptomatic placenta previa: a randomised controlled trial of inpatient versus outpatient expectant management. American Journal of Obstetrics and Gynecology 175:806-11.
- Love CD, Fernando KJ, Sargent L, Hughes RG. 2004. Major placenta praevia should not preclude outpatient management. European Journal of Obstetrics, Gynaecology and Reproductive Biology 117:24-9.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







