- What is Atrial Fibrillation (AF)
- Statistics on Atrial Fibrillation (AF)
- Risk Factors for Atrial Fibrillation (AF)
- Progression of Atrial Fibrillation (AF)
- Symptoms of Atrial Fibrillation (AF)
- Clinical Examination of Atrial Fibrillation (AF)
- How is Atrial Fibrillation (AF) Diagnosed?
- Prognosis of Atrial Fibrillation (AF)
- How is Atrial Fibrillation (AF) Treated?
- Atrial Fibrillation (AF) References
What is Atrial Fibrillation (AF)
Atrial fibrillation (AF) is a disorder of the rhythm of the heart. It results from disorganised electrical activity in the atria of the heart, which causes rapid stimulation of the ventricles, leading to an irregular pulse rate.
Statistics on Atrial Fibrillation (AF)
Atrial fibrillation is the most common sustained rhythm disorder of the heart. It is more common in older people, and occurs in more than 5% of the population over 65 years in Western countries. In Australia, AF affects around 2% of the general population.
Risk Factors for Atrial Fibrillation (AF)
Many diseases of the heart can predispose to AF. This is particularly so for conditions that cause enlargement of the atria. In addition, there are also many non-cardiac disorders that predispose towards AF.
Common risk factors for atrial fibrillation include:
-
- Coronary artery disease, including heart attack;
- Diseases of the heart valves, especially rheumatic heart disease;
- Sick sinus syndrome;
- Hyperthyroidism;
- High blood pressure;
- Cardiomyopathies;
- Congenital heart disease (an abnormality of the heart that is present since birth);
- Chest infection;
- Pulmonary embolism;
- Pericarditis;
- Alcohol.
In 50% of patients with paroxysmal AF and 20% of patients with persistent or permanent AF, no underlying heart disease can be found. This is known as ‘lone’ AF.
Progression of Atrial Fibrillation (AF)
In AF, the atria are continuously activated by rogue electrical currents at a rate of 350-600 beats a minute. The ventricles are unable to respond to such a high rate of stimulation, and therefore only a proportion of the impulses are translated into contractions of the heart.
AF can be classified into three groups:
- Paroxysmal AF: The patient gets repeated, short episodes of chest palpitations that resolve spontaneously. In between these episodes, the heart is normal;
- Persistent AF: AF that does not resolve spontaneously, but resolves after treatment;
- Permanent AF: AF that persists or recurs despite treatment. It usually occurs in patients who already have diseased hearts.
If left untreated, AF can lead to various short- and long-term problems. In patients who have pre-existing heart failure, the rapid heart rate seen in AF can lead to low blood pressure, lung congestion, angina, or worsening of the heart failure. Untreated AF also increases the risk of stroke. This is because in AF the atria become dilated and contract ineffectively, which leads to blood clots developing in the atria. These clots can subsequently dislodge and travel to the brain and other organs, causing strokes and other organ damage.
The main risk factors for developing a stroke in patients with AF are:
- Prior stroke or transient ischaemic attack;
- The finding of left ventricular dysfunction on echocardiogram;
- Age > 65;
- High blood pressure;
- Rheumatic heart disease;
- Diabetes mellitus;
- Congestive heart failure.
Symptoms of Atrial Fibrillation (AF)
Often, AF causes no symptoms and is discovered incidentally during routine examination or ECG. On the other hand, some patients can experience palpitations, light-headedness, fainting, fatigue, or shortness of breath. In patients with pre-existing heart failure, an episode of AF can cause worsening of their heart failure. A rapid heart rate can also cause angina in patients with pre-existing coronary artery disease.
Clinical Examination of Atrial Fibrillation (AF)
As part of the assessment, the doctor may do an examination to look for signs of AF. This may involve feeling for the pulse and listening to the heart sounds. In addition, the doctor may also do a blood pressure measurement, check for signs of overactive thyroid (neck swelling, eye abnormalities, tremor), listen to the lungs, and check for leg swelling.
How is Atrial Fibrillation (AF) Diagnosed?
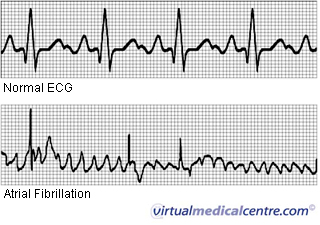
If the episodes of AF tend to come and go spontaneously and frequently, ambulatory ECG monitoring may be required. This involves wearing a device (Holter monitor) that records the ECG continuously over 24 hours so that any episodes of AF that occur during that period of time will be detected. For patients who experience less frequent but symptomatic episodes, a patient-activated event recorder may be used, whereby the patient activates the ECG recorder only when he/she experiences the symptoms of AF.
Sometimes a blood test may be needed to check for thyroid and electrolyte problems, both of which can cause AF. Lastly, some patients may need to have an echocardiogram, which uses ultrasound to look at the structure, size and functional capacity of the heart.
Prognosis of Atrial Fibrillation (AF)
Although the symptoms of AF can be distressing and worrying, AF is a common condition with a good outlook if treated appropriately. With treatment, most patients can control their heart rate and rhythm to an acceptable level.
How is Atrial Fibrillation (AF) Treated?
The main aims of treatment of AF are:
-
Restore the normal heart rhythm;
-
Prevent recurrence;
-
Optimise the heart rate;
- Reduce the risk of stroke.
If the episode of AF is precipitated by an illness such as pneumonia, pulmonary embolism or thyrotoxicosis, effective treatment of the primary illness will usually lead to spontaneous resolution of the AF.
When to seek medical help
Anyone who experiences persistent palpitations should see their doctor for medical advice. If there are symptoms of a heart attack (chest pain lasting for more than 10 minutes that may radiate to the neck, jaw, back, shoulders or arms; shortness of breath; nausea; and sweatiness) or stroke (sudden weakness or numbness on one side of the face, arm or leg; slurred speech; balance difficulties; or loss of vision), it is an emergency and an ambulance should be called immediately.
Pharmacological treatment and cardioversion
Paroxysmal AF
People who experience occasional attacks without symptoms do not usually require treatment for their condition. However, those who experience troublesome symptoms may benefit from medication to control the attacks. Two classes of drugs, the β-adrenoceptor antagonists and the class Ic antiarrhythmics (e.g. flecainide and propafenone), are drugs of first choice in this situation.
Persistent AF
A persistent episode of AF can be converted back to normal rhythm using electrical or pharmacological cardioversion. In electrical cardioversion, an electric ‘shock’ is given to the heart while the patient is anaesthetized, to restore the normal heart rhythm. In pharmacological cardioversion, medications are given as tablets or as an injection to revert the abnormal heart rhythm back to normal.
It is important to restore normal rhythm early because the chance of success decreases and the chance of recurrence increases with longer durations of AF. In some situations, the patient may need to take an anticoagulant medication for 3 weeks before the procedure to reduce the risk of forming blood clots. After successful cardioversion, anticoagulant medication has to be continued for at least 4 weeks because the atria may take time to recover.
Cardioversion is sucessful in around 65-90% of patients, but relapse of AF is common. Some patients may need to take long term medications to maintain the normal heart rhythm and reduce the risk of relapse.
Permanent AF
In permanent AF where normal rhythm cannot be restored, treatment is then directed towards controlling the heart rate and reducing the risk of stroke. Various medications, including digoxin, β-adrenoceptor antagonists and calcium antagonists (e.g. verapamil or diltiazem), are commonly used in these situations.
To minimize the risk of stroke, patients with AF may require long term medication (e.g. warfarin) to ‘thin the blood’ and stop it from forming blood clots. However, this is associated with an increased risk of bleeding complications. Aspirin has a lower risk of complications but is also less effective than warfarin. Therefore, the decision for ‘blood-thinning’ treatment has to be balanced between a patient’s risk factors for stroke and the risk of bleeding complications.
Surgical treatment
Surgical treatment of AF is rarely necessary because medications achieve satisfactory control in most cases. Occasionally, permanent atrial pacing (an artificial pacemaker is implanted) or radiofrequency catheter ablation may be used to treat paroxysmal AF. Radiofrequency catheter ablation is a procedure that is done to remove or inactivate areas of the heart that are thought to be responsible for generating the abnormal electrical signals in AF.
In patients with troublesome, permanent AF, a surgical procedure may be done as a last resort to stop the conduction of all impulses from the atria to the ventricles (complete heart block), together with the implantation of a permanent pacemaker.
Lifestyle management
AF is often associated with other forms of cardiovascular disease. Therefore, it is important to manage the other general cardiovascular risk factors such as blood pressure, diabetes, weight loss, exercise, smoking cessation, and healthy eating.1
For more information about exercise in patients with heart disease, go to the Virtual Medical Centre’s page on Advising Patients About Aerobic Exercise. Patients who are on warfarin should avoid contact sports where there is a significant chance of injury, due to the risk of excessive bleeding.
Atrial Fibrillation (AF) References
- Davidson S, Haslett C. Davidson’s Principles and Practice of Medicine (19th edition). Edinburgh: Churchill Livingstone; 2002. Book
- Feinberg WM, Blackshear JL, Laupacis A, et al. Prevalence, age distribution, and gender of patients with atrial fibrillation: Analysis and implications. Arch Intern Med. 1995;155(5):469-73. Abstract
- Hankey G. Atrial fibrillation [online]. Canberra, ACT: Heart Foundation; 2004 [cited 1 July 2008]. Available from: URL link
- Braunwald E, Fauci AS, Kasper DL, et al. Harrison’s Principles of Internal Medicine (16th edition). New York: McGraw-Hill Publishing; 2005. Book
- Peters NS, Schilling RJ, Kanagaratnam P, Markides V. Atrial fibrillation: Strategies to control, combat, and cure. Lancet. 2002;359(9306):593-603. Abstract
- Longmore M, Wilkinson I, Rajagopalan SR. Oxford Handbook of Clinical Medicine (6th edition). Oxford: Oxford University Press; 2004. Book
Treatments Used in This Disease:
Drugs/Products Used in the Treatment of This Disease:
- Amiodarone (Amiodarone hydrochloride)
- Astrix 100 Capsules (Aspirin)
- Atenolol (Terry White Chemists) (Atenolol)
- Clexane (Enoxaparin sodium)
- Deralin (Propranolol hydrochloride)
- Flecatab (Flecainide acetate)
- Lanoxin (Digoxin)
- Marevan (Warfarin sodium)
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







