- What is Arachnoiditis
- Statistics on Arachnoiditis
- Risk Factors for Arachnoiditis
- Progression of Arachnoiditis
- Symptoms of Arachnoiditis
- Clinical Examination of Arachnoiditis
- How is Arachnoiditis Diagnosed?
- Prognosis of Arachnoiditis
- How is Arachnoiditis Treated?
- Arachnoiditis References
What is Arachnoiditis
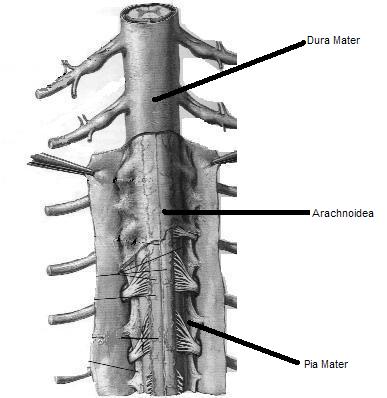
Causes of arachnoiditis include infections (bacterial, viral, fungal, and parasitic agents), irritation from chemicals, direct injury to the spine, chronic compression of spinal nerves, or complications of spinal surgery or other invasive spinal procedures.
Arachnoiditis as a result of neoplasia can be due to spread from cancers outside of the central nervous system (brain and spinal cord) or by direct spread from a cancer of the central nervous system.
The inflammation in arachnoiditis can sometimes lead to tethering and/or compression of the spinal cord through the formation of scar tissue and adhesions (spinal nerves sticking together).
Statistics on Arachnoiditis
Arachnoiditis can affect any age group, but is more common in adults between 40 and 60 years of age. It is equally common in both genders.
Arachnoiditis is uncommon, however, the number of cases is increasing worldwide due to the increasing number of immunocompromised patients including diabetics, alcoholics and intravenous drug abusers, people with AIDS, and transplantation and chemotherapy patients.
Risk Factors for Arachnoiditis
Factors that increase the risk of arachnoiditis include:
- Infection from bacteria or viruses;
- Patients with decreased immune function: diabetes, alcoholism, AIDS, chemotherapy and organ transplant patients;
- Surgery involving the brain or spinal cord;
- Contrast media, anaesthetics and steroids given intrathecally (into the subarachnoid space).
Progression of Arachnoiditis
Arachnoiditis does not tend to improve significantly with treatment. There is no clear relationship between the time of onset and pattern of symptoms, therefore complicating disease outcome prediction. For many, arachnoiditis is a disabling disease that causes chronic pain and neurological deficits.
Symptoms of Arachnoiditis
Arachnoiditis has no consistent pattern of symptoms, but it more frequently affects the nerves that supply the lower back and lower limbs. Arachnoiditis may interfere with nerve function and cause:
- Numbness;
- Tingling; and
- Stinging/burning pain in the lower back and/or lower limbs.
How is Arachnoiditis Diagnosed?
An MRI is the investigation of choice for diagnosing arachnoiditis however, a CT myelography can be used.
Prognosis of Arachnoiditis
As the disease progresses, symptoms may become more severe or even permanent. Many people with arachnoiditis are unable to work and suffer significant disability because they are in constant pain.
How is Arachnoiditis Treated?
There is no cure for arachnoiditis. Treatment options for arachnoiditis are similar to those for other chronic pain conditions. Most treatments focus on relieving pain and improving ability to perform daily activities. Often, healthcare professionals recommend a program of pain management, physiotherapy, exercise, and psychotherapy. Surgery for arachnoiditis is a controversial topic and is generally not recommended. Most treatments are aimed at relieving symptoms like pain and at improving daily functioning.
Arachnoiditis References
- Brammah TB, Jayson MI. Syringomyelia as a complication of spinal arachnoiditis. Spine. 1994;19(22):2603-5. Abstract
- Georgy BA, Snow RD, Hesselink JR. MR imaging of spinal nerve roots: Techniques, enhancement patterns, and imaging findings. AJR Am J Roentgenol. 1996;166(1):173-9. Abstract | Full text
- Hankey G, Wardlaw J. Clinical Neurology. New York, NY: Demos Medical Publishing; 2002. Book
- Holz A. Arachnoiditis imaging [online]. Omaha, NE: eMedicine; 2003 [cited 30 December 2005]. Available from: URL link
- Johnson CE, Sze G. Benign lumbar arachnoiditis: MR imaging with gadopentetate dimeglumine. AJR Am J Roentgenol. 1990;155(4):873-80. Abstract | Full text
- NINDS arachnoiditis information page [online]. Bethesda, MD: National Institute of Neurological Disorders and Stroke; 2005 [cited 30 December 2005]. Available from: URL link
- Sharma A, Goyal M, Mishra NK, et al. MR imaging of tubercular spinal arachnoiditis. AJR Am J Roentgenol. 1997;168(3):807-12. Abstract | Full text
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







